Innovation is what keeps biomedical systems on the cutting edge, advancing human health and wellness through analysis, diagnosis and treatment. Much novel design begins in university biomedical engineering programs and other multidisciplinary college courses, where today’s academic collaborators turn out tomorrow’s technologies and products.
The University of Virginia (UVA) in Charlottesville offers a “bio-innovation” class that involves biomedical engineering students as well as those from programs as diverse as business, architecture and nursing, along with faculty members representing each discipline. As described by Philippe Sommer, director of entrepreneurship programs at UVA’s Darden School of Business, one student is taken from each discipline to form a group.
Subsequently, that group is sent off to a hospital to observe what works and what doesn’t, with the goal of identifying problems that only a multidisciplinary approach can solve. Sommer said it takes interviewing, observing, listening and even paying attention to body language to understand what the problems are. To understand the problems and design a solution, the students must explore more than what the medical personnel perceive the difficulties to be.
At Vanderbilt University’s Institute for Integrative Biosystems Research and Education (VIIBRE) in Nashville, Tenn., biomedical engineering professor John Wikswo sees the multidisciplinary approach as necessary for advancing current biological solutions. VIIBRE was created with the core mission of interdisciplinary research in biophysical sciences and bioengineering. Researchers in biology, physics, medicine, engineering and education are collaborating on the development of cellular biosensors for cancer research, chemical and biological disease detection systems, and more.
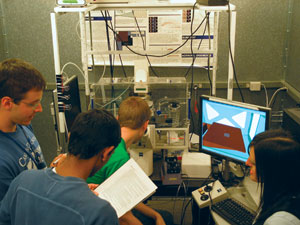
In the VIIBRE lab at Vanderbilt University, four students are shown collaborating on an automated microscope that they’re using in conjunction with a state-of-the-art ion-mobility mass spectrometer.
VIIBRE works closely with CFD Research Corp. of Huntsville, Ala., and Hypres of Elmsford, N.Y., and the institute is in discussions with other biotech companies. VIIBRE is focusing on research enabled by its development of low-cost microfluidic devices for automated, real-time, high-content imaging. The institute is also working on mass spectrometer approaches to answering complex biological questions.
Wikswo said that in VIIBRE’s lab, cancer biologists, pathologists, chemists, physicists and bioengineers work side by side. “In the past, each individual discipline went after the low-hanging fruit,” he said, explaining that many of the simple problems in biology have already been identified and addressed. In recognition of the fact that “biology is phenomenally complicated,” Wikswo and colleagues have assembled multidisciplinary teams that address integral, multifactorial problems such as tissue repair, immune system activation, angiogenesis and tumor cell dissemination.
He pointed to the work of Andries Zijlstra, assistant professor of pathology and cancer biology, as especially inspiring. Zijlstra came to Vanderbilt from The Scripps Research Institute three years ago and has been working with scientists skilled in microfabrication, photonics, biology and physics to develop tools for live-cell fluorescence microscopy.
By integrating the various disciplines, Zijlstra said they’re “taking biological imaging to the fifth dimension.” His team is constructing novel systems for both in vitro and in vivo imaging by incorporating microfluidics, engineered cultured environments and biophotonics. Besides his academic accomplishments, Zijlstra has achieved business success as co-founder of a small biotech company, Innovascreen of Halifax, Nova Scotia, Canada, which uses biophotonics for in vivo drug discovery and validation. Wikswo points out that “the future of biology may rest on the strength of interdisciplinary and corporate collaborations like this one.”
Competitions
A number of contests pit design against design, with an emphasis on advancing the plan through the many stages that lead to commercialization. As biomedical engineering deals with human health and wellness, today’s engineering programs place an increased emphasis on “doing good” for society, which in terms of biomedical systems translates to developing ones that will somehow benefit society in general, or underdeveloped or underserved populations. Several design competitions emphasize this societal element.
The Biomedical Engineering Innovation, Design and Entrepreneurship Award (BMEidea) emphasizes entrepreneurship and potential commercialization. Sponsored in part by the National Collegiate Inventors and Innovators Alliance, the prize recognizes projects that involve a health-related technology and meet a “relevant clinical need.” Criteria used by the judges include the project’s technical, economic and regulatory feasibility as well as its contribution to health care and quality of life. Technical innovation is also important, as is its potential to be commercialized or to benefit underserved populations and improve their access to health care.
In a presentation on innovation given at a recent BMEidea meeting, Peter DeComo, co-founder and former chairman and CEO of Renal Solutions in Warrendale, Pa., summarized that entrepreneurship/innovation is about recognizing big opportunities, mitigating risk and creating structure amidst chaos. The time to innovate, DeComo said, is when a great possibility for disruption of equilibrium exists, when a significant problem can be solved and when a competitive advantage can be gained. And considering potential commercialization, he sees the time to innovate as when sources of funding are clear, when customers are willing to pay a premium price and when the financial model shows that revenue, margin and profits are substantial.
The path to commercialization
At Beth Israel Deaconess Medical Center in Boston, Dr. John Frangioni knows that the path to commercialization is riddled with testing, paperwork, licensing, trademarks, developing partnerships and more. His team developed a real-time surgical imaging technology called Fluorescence-Assisted Resection and Exploration (FLARE), which integrates novel imaging instrumentation and consumable contrast agents. These imaging agents effectively light up (in color) diseased tissue that otherwise might be overlooked by surgeons seeking to remove it. And the technology can highlight healthy tissue to prevent surgeons from damaging, for example, blood vessels or nerves.
The FLARE system includes cameras (both visible and near-IR) and LED light sources for near-IR fluorescence. The instrumentation integrates with a video monitor, computer and software. The way it works is that near-IR fluorophores glow with a fluorescence that’s captured by IR imaging cameras. Images of the glowing cancer cells are superimposed on visible-light images of the surgical field, so that the surgeon can see the cancer cells even when the background is crowded by blood vessels and other structures. What makes this system innovative is the combined use of visible and near-infrared images, providing surgeons with visual landmarks for performing highly effective operations. A surgeon can attach a near-IR fluorophore to any targeting ligand to “drag” it to whatever he or she needs to see. Frangioni explained that, someday, we’ll have targeting ligands for the breast cancer itself, which will help the surgeon “see” the cancer and cut it out using FLARE.
In developing FLARE, Frangioni collaborated with several outside partners, including General Electric Healthcare in Chalfont St. Giles, UK, and Siemens Healthcare in Munich, Germany. Currently no license agreements are in place with GE or Siemens, and the patents and trademark in the FLARE technology portfolio are available for licensing for human clinical applications. FLARE is currently in clinical trial. Dr. Susan Troyan, director of the breast care program at Beth Israel Deaconess Medical Center, is using it in a study that maps sentinel lymph nodes in breast cancer patients.

These images were taken of a female patient who needed sentinel lymph node mapping to see whether her cancer had spread. The color video image on the left is what is seen without fluorescence. In the middle panel, the sentinel lymph node, which was imaged using FLARE and invisible near-IR fluorescent light, is obvious as a bright-white object. The exact location of the sentinel lymph node is shown in the color image on the right.
Troyan noted that this is only the first use of this innovative system and that “the exciting part will be in the future when we learn how to attach fluorophores to different types of tissue such as cancer cells and help direct the extent of dissection.” She added that it will be particularly useful in distinguishing the location of cancerous tissue in relation to nerves, such as in prostate surgery. Several people have used near-IR cameras to look at fluorophores, but being able to take a real-time video and overlay the fluorescence is a real benefit, Troyan said.