Nicholas Harrop, !%DILAS Diodenlaser GmbH%!
Laser-based surgery is staking an increasingly important claim in operating theaters across the world. More specifically, a class of devices called high-power diode lasers (HPDLs) provides numerous advantages over instrument-based surgery as well as over other surgical lasers. The primary advantage of HPDLs is that they offer a wide range of wavelengths, which makes them attractive instruments for surgery.
One of the greatest benefits of an HPDL is that it can be directly modulated. The current semiconductor lasers respond to “power on” more or less instantaneously. Solid-state lasers such as Nd:YAG have a fluorescence lifetime in the range of milliseconds. Therefore, when operating a surgical HPDL, there is virtually no delay between the input of the operating surgeon and the emission of laser radiation. In addition, the HPDL can easily be adjusted to any power level from 0 to 100 percent, allowing carefully dosed optical power, whereas solid-state lasers have threshold-based operating conditions that typically permit power modulation only between 60 and 100 percent.
The range of wavelengths available makes the HPDL the perfect tool for a variety of medical applications, including surgery. For an overview of medical applications and corresponding wavelengths using HPDLs, see Table 1.
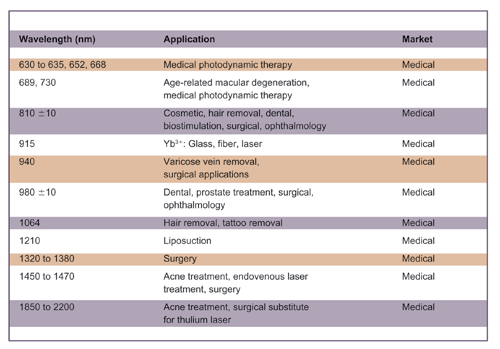 Table 1. Overview of diode laser wavelengths available for medical applications. Courtesy of Dilas.
Table 1. Overview of diode laser wavelengths available for medical applications. Courtesy of Dilas.
Because the basic function principle of semiconductor lasers is the same regardless of wavelength, the operation of such lasers is also the same. This eliminates lengthy – and sometimes expensive – teaching processes for surgeons when using a new wavelength. Furthermore, the scalability of HPDLs enables a wide range of power levels at each wavelength. At standard wavelengths such as 980 nm, the power ranges from 30 W with a single diode bar up to 500 W with 12 diode bars in continuous-wave operation. For a detailed overview of the wavelength-specific output powers available, see Figure 1.
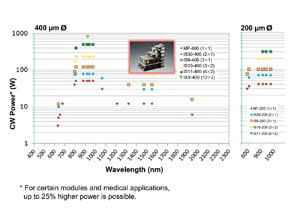
Figure 1. Overview of output power levels available from fiber-coupled modules. Courtesy of Dilas.
Because medical laser applications are based on fiber-coupled HPDLs, specific safety features that cater to the needs of the medical market have been developed. These modules include a monitor photodiode, temperature sensors, fiber connection interlock switches and an end-user-replaceable blast shield. Surgical fibers are disposable goods, so the centricity of these fibers is often of a lesser quality compared with industrial fibers. This can cause the fiber to overheat and burn off. The blast shield eliminates contamination of the diode element and fiber coupling optics from the burned fiber. Once the fiber and blast shield are replaced, surgery can continue within a matter of minutes, without a long interruption for the prepared, often sedated, patient. The fiber guarantees that minimally invasive keyhole surgeries can be performed, leading to reduced risk and shorter recovery times for patients.
Medical applications
Table 1 provides a general overview of medical applications for HPDLs. The wavelength range from 630 to 1940 nm enables these lasers to be used in a multitude of ways. Laser diodes in the 630- to 689-nm red wavelength range are used in photodynamic therapy. With this technique, a laser-active agent called a photosensitizer, which is wavelength-selective, is injected into the body. The agent accumulates in tissue such as cancer cells and absorbs laser radiation at the specific wavelength. Upon returning to the ground state, the molecules of the photosensitizer produce free oxygen radicals, which are highly reactive and deplete the cancerous cells.
In general, the wavelength range between 810 and 980 nm is the most established in HPDLs, yielding the highest efficiencies and output powers per bar. Aside from surgery, which will be discussed in greater detail, these wavelengths are used for cosmetic applications, hair removal, dentistry, biostimulation, ophthalmology and varicose vein removal. In addition, the 1064- and 1210-nm wavelengths are used in the cosmetic industry for hair and tattoo removal as well as for liposuction. Laser radiation at 1210 nm is absorbed by adipose tissue, which is depleted. HPDL wavelengths in the infrared range from 1320 to 1940 nm are used for dermatological treatment such as acne removal and for endovenous laser treatment. High-power diode lasers at 1940 nm can be used as surgical substitutes for thulium lasers.
Surgical applications
The field of surgery also benefits greatly from the range of HPDL wavelengths. The absorption and coagulation properties of various tissues of the human body differ, and wavelengths can be chosen according to which part of the body is undergoing surgery. These wavelengths also can be used in combination to capitalize on the benefits of each individual wavelength. For example, a laser with two wavelengths can benefit from good ablative and coagulative properties, leading to greatly reduced blood loss during surgery.
In general, laser surgery is used for treating the abdominal organs, including the intestines, esophagus, stomach, colon, liver and bile ducts. Other surgical applications include laser-induced thermotherapy of liver tumors, esophagotracheal fistulae, colorectal carcinomas, angiodysplasia, erosion of the gastric membrane, colonic polyps, esophageal stenosis and hemorrhoids. Here, surgical lasers can be used for coagulation, vaporization and cutting.
Coagulation is the irreversible denaturization of proteins, both functional and structural. Superficial coagulation can be achieved by using high laser power density, short application times and no overlapping of irradiated areas. Deep coagulation is achieved by heat diffusion into deeper tissue layers. In this case, the laser light is still absorbed only in the first few millimeters below the surface. Coagulated volume is generated by the combination of medium power density, long irradiation times and a cooling of the surface.
Higher power densities or longer radiation times lead to tissue vaporization. Before the tissue vaporized, its surface is carbonized by laser radiation, resulting in higher absorption rates and immediate vaporization. Below the vaporized volume, a coagulation zone leads to the immediate occlusion of capillary vessels, resulting in reduced bleeding. In the case of strongly perfused tissue such as tumors or larger vessels, hemostasis can be achieved by precoagulation of the tissue to be vaporized, or by a well-selected combination of laser wavelengths.
Lightguides (fibers) with bare tips or with special application tips can be used to cut or vaporize tissue efficiently during contact. Carbon deposits form upon contact with laser radiation, and the application tips become slightly blackened. This in turn causes the tip to heat up to several hundred degrees, which carbonizes the tissue on contact due to the radiation absorption caused by this procedure. As the cutting radiation always meets carbonized tissue, it leads to immediate vaporization. This method of contact cutting is possible in both air and liquid environments. Even though the cutting is only between 0.3 and 0.5 mm wide, it provides sufficient hemostatic reliability.
Laser resection is used to treat endoluminal lesions in both curative and palliative ways by applying laser energy through a fixed and/or flexible fiber-coupled bronchoscope. The effect of the laser is influenced by the type of laser used, the tissue characteristics and duration of the application. In addition to vaporization, bronchoscopy lasers also provide fine coagulation of tissue. Hence, Nd:YAG lasers have been used for such applications in the past.
However, an increasing number of users are turning to diode lasers for laser resection. In single-wavelength diode lasers, coagulation is achieved by increasing the distance from the fiber tip to the tissue, whereas vaporization is achieved by reducing this distance. The selected tactic depends upon the availability of fixed bronchoscopy. When using fixed bronchoscopy, the tumor is coagulated first using laser radiation and then ablated mechanically with a fixed pipe. The flexible bronchoscopy procedure also coagulates the tissue. Afterward, the tumor is either vaporized completely or ablated mechanically.
Today, HPDLs are in wide use in the range between 1320 and 1380 nm – essentially Nd:YAG wavelengths formerly used in medical applications – and at 1470 nm. These diode lasers show results that are comparable to, if not better than, those of Nd:YAGs. Light at these wavelengths is absorbed by cellular water, which is heated until the cell bursts.
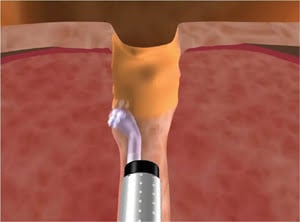
Figure 2. Function principle of side-firing fiber for benign prostatic hyperplasia surgery. Courtesy of biolitec AG.
This is an effect that, among other methods, is used for tissue removal in treating benign prostatic hyperplasia. Specially formed fibers, such as the one shown in Figure 2, are used for this purpose. By using local anesthesia and flushing the affected area with cold water during treatment, there is no pain for the patient, and the cell debris is removed. The results of benign prostatic hyperplasia laser surgery can be seen in Figure 3, where the first image shows a contraction of the urinary tract, and the following images show two stages of the procedure.
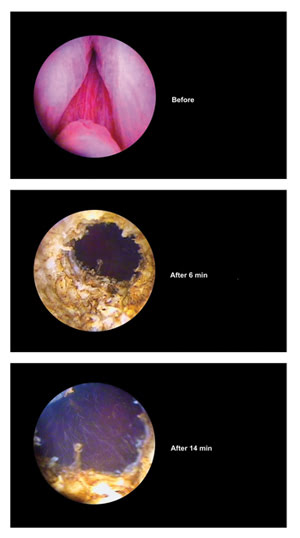
Figure 3. The process of benign prostatic hyperplasia surgery is shown at different stages. Courtesy of biolitec AG.
Meet the author
Nicholas Harrop works in sales at Dilas Diodenlaser GmbH in Mainz-Hechtsheim, Germany; e-mail: [email protected].