Techniques that leave cell systems and organisms intact could provide a means to screen whole populations for disease less invasively and less expensively than traditional tests.
In vivo optical techniques provide a wealth of information about the workings of cells, organs and even entire systems, and thus have advanced a range of basic science studies. But how can they contribute to clinical applications? Is it possible, for instance, that they might someday supplant conventional histology methods in the diagnosis of disease?
“Many groups have looked at how optical techniques can differentiate cancerous from normal tissue,” said Vadim Backman of Northwestern University in Evanston, Ill. “We asked the question, ‘Can we do something different? Can we do something that histopathology cannot?’”
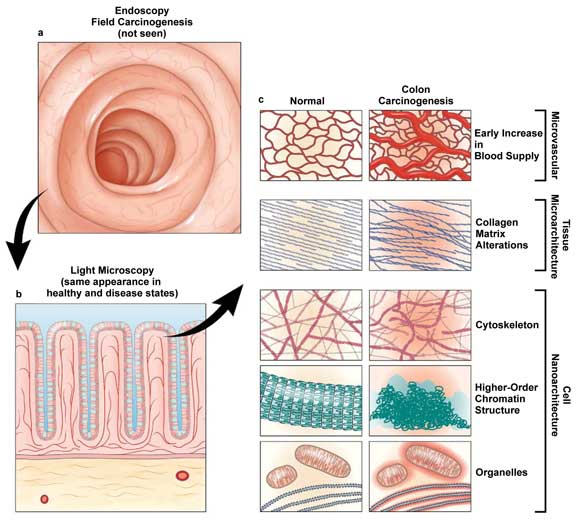
Field carcinogenesis manifests itself in a variety of ways at the tissue physiology and morphology levels that neither endoscopy nor histopathology can detect. The low-coherence enhanced backscattering spectroscopy (LEBS) technique can uncover these manifestations, which include alterations in microvasculature and tissue microarchitecture, and thus can enable early detection of field carcinogenesis. Courtesy of Gastroenterology.
The answer was, in fact, yes. The significance of the technique – with respect to cancer management – lies in its sensitivity to the field effect. The field effect concept holds that molecular abnormalities can be found in histologically normal tissues in the initial stages of carcinogenesis, and that these can be used as a predictor of disease.
Backman offered the analogy of a bad neighborhood in describing the concept. You don’t know when or where a crime is going to happen here, he said, but, statistically, you can state with some certainty that a crime will take place.
He and his colleagues, including graduate students Andrew J. Radosevich and Nikhil N. Mutyal, are developing a technique called low-coherence enhanced backscattering spectroscopy, or LEBS, which enables users to detect the ultrastructural properties of tissue.
The LEBS phenomenon was first observed by Young L. Kim, then a graduate student working with Backman and now an assistant professor at Purdue University in West Lafayette, Ind. As Backman explained in a recent phone interview, the technique could have important implications for cancer management.
The researchers found that LEBS could detect the field effect even in histologically normal sites and, based on this, could predict the occurrence of cancer with remarkable accuracy. Thus, it could identify bad neighborhoods, so to speak, on organs. This had interesting implications for basic science studies of the initial stages of cancer progression. But it also suggested a “very big” clinical application, Backman said: cancer screening.
Screening is, of course, a significant aspect of cancer management. However, although we have well-established second-tier screening strategies for almost all cancers, in many cases we are still missing the initial screening test – the fast, inexpensive test that can be used to screen entire populations. Take, for example, cervical cancer. Fifty years ago, this was the No. 1 cancer in women. Now it’s No. 14. Why? “Not because we changed how we treat it,” Backman said, “but because of the Pap smear.” The introduction of the Pap smear made it possible to screen every woman and to identify those at risk for cervical cancer.
Similarly, a technique that can detect the field effect could provide a means to screen whole populations less expensively and less invasively than is currently possible with many cancers.
Backman and colleagues have focused on screening for colorectal cancer. Colonoscopy is an effective but highly inefficient screening method, with more than 90 percent of procedures not showing relevant neoplasia. For this reason, a less invasive initial screening test to identify patients who should undergo a colonoscopy is desirable.
Using the LEBS technique to detect the field effect, the Northwestern researchers have come up with a means to do this. In a 2009 Cancer Research study, they demonstrated that they could accurately predict colonic neoplasia using LEBS analysis of microscopically normal rectal biopsies. Now, in a talk at Digestive Disease Week in San Diego in May and in a paper in preparation, they have reported an in situ validation trial with a recently developed LEBS fiber optic probe.
“We showed that we can accurately predict, just by taking rectal measurements” – that is, without a colonoscopy – “which patients harbor early precancerous lesions in the colon and which do not, and therefore do not have to have a colonoscopy,” Backman said.
The researchers are exploring use of the technology with other cancers, while also moving forward in seeking FDA approval for the precolonoscopy application. If all goes well, the LEBS technique could be ready for clinical implementation – as an initial screening test for colorectal cancer – within the next several years.
Here, as in many cases, in vivo techniques can best serve as complementary approaches in an overall cancer management strategy. They are not likely to replace conventional histology for diagnosis of disease, at least not anytime soon.
“I think pathologists are interested in technologies that can provide more targeted biopsies,” said Adam Wax, a researcher at Duke University, in Durham, N.C. Wax and colleagues are developing a technique – angle-resolved low-coherence interferometry (LCI) – for in vivo depth-resolved nuclear morphology measurements to detect dysplasia in patients with Barrett’s esophagus (see: “Moving Noninvasive Cancer Imaging into the Clinic,” in the March issue of BioPhotonics).
As with the LEBS technique developed at Northwestern, angle-resolved LCI can help determine which patients are at risk and must undergo additional procedures. Currently, using conventional technology, endoscopists will perform biopsies in each of the four quadrants of the esophagus. Even with considerable effort, however, they might see only 2 percent of the tissue there.
With angle-resolved LCI, clinicians can scan an entire quadrant, point by point, more quickly than taking a biopsy. The best part, Wax said, is that it offers nearly 100 percent negative predictive value. “If our device says there are no precancerous lesions, there’s a nearly 100 percent chance there are none. So you’re justified in not taking a biopsy.”
Taking on traditional blood tests
Some in vivo technologies might replace conventional diagnostic methods, but only under certain circumstances – in global health applications, for example – where conventional techniques either are not available or do not meet a particular need.
At the Israel Institute of Technology, or Technion, researchers have developed a device that might do just this. The device takes advantage of the natural movement of blood cells flowing inside a vessel to uncover blood parameters that, otherwise, could be measured only with a traditional blood test, in real time using a static, compact probe with no moving parts.
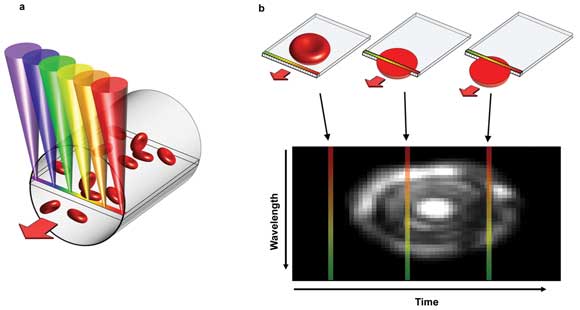
Researchers have reported a device that noninvasively measures blood parameters that otherwise could be obtained only by traditional blood test. The device relies on a technique called spectrally encoded confocal microscopy, or SECM. Here, a single line within a blood vessel is imaged with multiple colors of light that encode lateral positions (a). A single cell crossing the spectral line produces a 2-D image, with one axis encoded by wavelength and the other by time (b). Courtesy of Biomedical Optics Express.
To achieve this, they used a technique called spectrally encoded confocal microscopy, or SECM. SECM creates images by splitting a beam of light into its constituent colors and spreading them out in a line from red to violet. A probe is applied against the skin, and this line of light is transmitted across a blood vessel near the surface. Blood cells scatter light as they cross the line. This scattered light contains spatial information that is used to create 2-D images of the cells.
To assist in locating the target blood vessels below the skin, said Lior Golan, a graduate student at Technion and one of the authors of a Biomedical Optics Express paper reporting the device, the researchers added an auxiliary wide-field imaging channel, which enables users to identify optimal imaging sites across the chosen vessels. This channel employs green light, which diffusively illuminates the tissue in question and is well absorbed by the blood vessels. The vessels consequently appear as dark channels against a bright background.
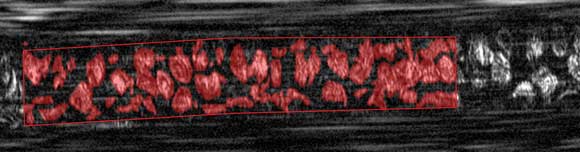
An in vivo image of red blood cells within a microvessel, obtained using the SECM-based device. The area occupied by red blood cells in the images can be used to calculate the percent volume of red blood cells, a key measurement for many medical diagnoses.
The researchers chose the inner lip as a test site – the inner lip is rich in blood vessels, has no light-blocking pigment and maintains blood flow in trauma patients – but other imaging sites may become possible as they improve the penetration depth of the system.
Golan and colleagues do not expect the technology to replace traditional blood tests entirely anytime in the future. Rather, they anticipate its use in cases where traditional blood tests do not provide results quickly enough to be relevant.
Potential applications include monitoring of hematocrit in intra- and postsurgery patients who are prone to internal bleeding; assessment of patients with hemoglobin disorders; and online monitoring of white blood cells in critical care patients, which could provide an early warning at the onset of a bacterial infection.
Another possible application is screening of large populations for common blood disorders in rural and other underserved areas. Golan noted, for example, that some disorders – such as hemoglobinopathies – are widespread in rural areas of Africa.
Here, he said, the technology could contribute in important ways, helping to improve the availability of care in underserved areas.
“Traditional blood tests require extraction of blood samples, preparation of slides, and examination in a laboratory setting to get results,” he said.
“We believe that our future device could be carried and used by a single doctor, providing immediate diagnosis at the point of care.”
In a 2011 review of light-scattering technologies for field carcinogenesis detection in Gastroenterology, researchers Vadim Backman and Hemant K. Roy describe how low-coherence enhanced backscattering spectroscopy (LEBS) can identify epigenetic/genetic alterations of the field effect. Such alterations can lead to significant ultrastructural consequences, they wrote, and although visualization of such small structural changes is impossible with microscopy, light scattering enables measurement of their statistical properties.
Here is where it gets a little bit technical. LEBS can measure the mass-density correlation function, which quantifies the extent to which spatial correlation between structures depends on distance – which, itself, offers a means to describe tissue ultrastructure. Using the technique, researchers can determine the shape of the correlation function, the average amplitude and the length scale of mass-density variations, all of which serve as ultrastructural markers of field carcinogenesis.