Surgeons have long used microscopes to help them perform their delicate work. But, in this setting at least, microscopes have traditionally done little more than magnify.
Two devices aim to change that by helping to differentiate healthy and diseased tissue in ways that are practical and speedy enough for use in the operating room. One microscope takes advantage of stimulated Raman scattering (SRS); the other, near-infrared (NIR) fluorescence.
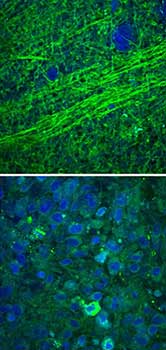
Images collected using an SRS microscope show that normal brain contains sparse cells with bundles of axons (top), but brain tumor tissue is full of cells in a disordered pattern (bottom). Courtesy of University of Michigan Health Services.
The SRS device, developed by researchers at the University of Michigan in Ann Arbor and Harvard University in Cambridge, Mass., can rapidly detect signs of cancer in tissue samples taken during surgery.
The system includes tissue classification software that weighs factors like the ratio of protein to lipid, axon density and degree of cellularity to determine — with >99 percent accuracy — whether cancer cells have infiltrated the tissue sample.
"It allows the surgical decision-making process to become data-driven instead of relying on the surgeon's best guess," said Dr. Daniel Orringer, a Michigan professor and neurosurgeon. "We're able to visualize tumor that otherwise would be invisible to the surgeon in the operating room."
In clinical use since June, the microscope has assessed samples from 60 patients so far. Depending on continued test results, the technology could be submitted for FDA review within two years, the university said.
The team aims to create a product about the size of a microwave that would sit close to the operating table, providing surgeons with a quick way to examine tissue samples and determine whether more surgery is needed. Currently such assessment takes about half an hour and must be carried out by a pathologist.
The SRS microscope would also be more affordable than current clinical imaging systems like intraoperative MRI.
"This technology has the potential to resolve a long-standing issue in cancer surgery, which is the need for faster and more effective methods to assess whether a tumor has been fully removed," said Dr. Richard Conroy, director of the Division of Applied Science & Technology at the National Institute of Biomedical Imaging and Bioengineering.
Development funding came from that and three other branches of the National Institutes of Health, as well as the American Association of Neurological Surgeons and the Michigan Institute for Clinical and Health Research.
The work was published in Science Translational Medicine (doi: 10.1126/scitranslmed.aab0195).
Augmented Microscopy
Meanwhile, an NIR device developed at the University of Arizona in Tucson can be used to augment surgical stereomicroscopes mounted on articulated arms and used in neurosurgery and other procedures.
The device superimposes NIR imagery at 20 fps onto the standard visible-light field of view of the stereomicroscope, allowing visualization of subsurface diagnostic information such as blood flow and cancerous tissue. It can also reveal beams used in laser surgery, which would otherwise be invisible.
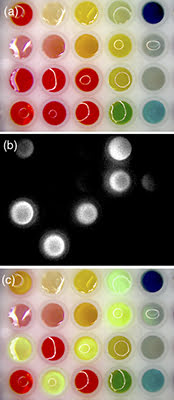
Dye solutions are imaged with visible light through a microscope (a), in the near-infrared as seen on a computer monitor (b) and in an augmented view combining the visible and NIR signals as seen in real time through the ocular of the augmented microscope (c). Courtesy of the Journal of Biomedical Optics.
NIR fluorescence imaging has been used in surgery for about a decade, but previous systems could only toggle between visible and NIR imagery rather than combine them. Moreover the NIR images were 2D, meaning they lacked the spatial cues that would help surgeons identify anatomical points of reference.
By utilizing the optical path of the stereomicroscope, the device maintains full 3D stereoscopic vision. The system is described in the Journal of Biomedical Optics (doi: 10.1117/1.JBO.20.10.106002).
"Surgeons want to see the molecular signals with their eyes, so that they can feel confident about what is there," said journal associate editor Brian Pogue of Dartmouth College. "Too often what they see is a report of the signals depicted in false color on a monitor. By displaying information through the surgical scope itself, the surgeon then sees the information with his or her own eyes."
The technology could be especially useful in surgery to remove brain tumors. Such procedures are dangerous because they can damage healthy tissue. At the same time, any cancerous tissue left behind can grow into a new tumor. The NIR-augmented view could allow surgeons to remove tumors more completely and with better precision.
The Arizona team's work was funded by National Institutes of Health.