Cutting-edge laser technology and new techniques are enabling amazing diagnostic and treatment advances in ophthalmology.
In 1981, Rangaswamy “Sri” Srinivasan, a researcher at IBM’s Thomas J. Watson Research Center, experimented with a pulsed argon fluoride (ArF) excimer laser on turkey leftovers, and lasers have had an ever-growing role in ophthalmology ever since. That landmark resulted in the first laser-based vision-correction techniques, including laser-assisted in situ keratomileusis (lasik) and photorefractive keratectomy (PRK) techniques.
Ophthalmology uses numerous photonic technologies – Nd:YAG and femtosecond excimer lasers, 3-D imaging techniques and OCT (optical coherence tomography) – to diagnose and treat eye diseases and vision problems. Today, these techniques are being combined into systems that are revolutionizing the eye surgeon’s job. Even moderately powered lasers can be dangerous to the eyes when mishandled (see sidebar), but (perhaps ironically) because of this ability to burn tissue, surgical laser systems have become indispensable in the operating theater for treatment of numerous eye conditions. They deliver less painful, faster, more reliable and precise results than traditional incision techniques.1
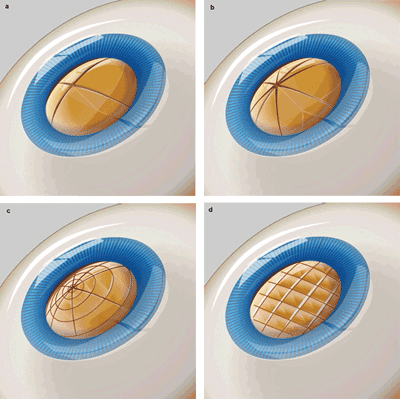
Surgical laser systems such as the Lensar Laser System break up the cloudy cataract via laser-scored
patterns (a-d: cross, pie, bull’s-eye and grid). The use of a laser reduces the amount of ultrasound
required, which reduces postoperative inflammation. Courtesy of Lensar.
Cataracts
Cataracts, a cloudiness of the eye’s clear crystalline lens, are the leading cause of vision loss in the world, affecting half of all individuals over the age of 60. Nearly 22 million cataract surgeries were performed globally in 2013, according to estimates from MarketScope. The global market for femtosecond lasers for cataract surgery is growing exponentially and will reach $2.4 billion by 2019, according to a market report from RnR Market Research of Dallas.
Cataract surgery involves fragmentation of the cloudy cornea, and its emulsification and removal (aspiration of the fragments), followed by the transplantation of an artificial intraocular lens (IOL) made of silicone or acrylic. Since the use of femtosecond excimer lasers became common in 2009, the surgery has evolved into an outpatient technique that takes only a few minutes. Use of lasers reduces or eliminates the use of ultrasound, typically administered manually to break up and emulsify the cataract. This helps reduce damage to epithelial cells in the eye. The results are more consistent, accurate and predictable.
Recent advances in cataract treatment include the development of better IOLs that can compensate for the natural ability of the cornea. One type of IOL, the multifocal IOL, mimics accommodation – the ability to focus from near to far distances – by providing multiple focal points at near, intermediate and far distances. Pseudoaccommodative IOLs flex to help restore near vision by using the muscles and natural physiological mechanisms of the eye to bring a focus from far to near.2 What is remarkable about the latest versions of IOLs is that they can be used not only to reclaim vision lost to cataracts, but also to address myopia (nearsightedness), astigmatism (blurred vision), hyperopia (farsightedness) or presbyopia (the need for reading glasses) at the same time. By some accounts, today’s cataract surgery may enable older patients to see as well as they did in their youth.
A new cataract diagnosis and treatment technique piloted in Edinburgh, Scotland, may offer improved evaluation and management of the condition. When Dr. S. Desmond Smith, professor emeritus of physics at Heriot-Watt University and founder of Edinburgh Instruments, required cataract surgery in his 80s, he and his surgeon – Dr. Baljean Dhillon, professor of clinical ophthalmology at the University of Edinburgh – decided to find a better way to diagnose cataracts. The inadequate current method requires an ophthalmologist to observe the scattering of visible wavelengths through a slit lamp microscope, which is subjective and unquantifiable, Smith said. “One cannot put a detector into a living eye to measure transmission.”
But something else can. After several years of collaborating with a long line of scientists at Edinburgh Instruments (and spinoff Edinburgh Biosciences), the team came across a technique that quantifies the amount of cataract damage via the autofluorescence of tryptophan in the eye lens.3 Whereas the tryptophan spectral emission in healthy eyes peaks at 330 nm, it begins to emit more at 430 nm instead as the eye becomes cloudier. This quantifiable technique can enable a more reliable diagnosis and a more accurate yes/no answer as to whether surgery is required. The team hopes that such an advance may reduce the amount of premature, invasive and expensive cataract surgeries.
As a further benefit of the research, a group at Glostrup Hospital and the University of Copenhagen, led by professor Michael Larsen and Dr. Line Kessel, simultaneously found that when lenses with cataracts are exposed to the two-photon absorption effect at 400 nm of an 800-nm femtosecond laser, the IR radiation causes a photobleaching effect that slightly improves the transmission of donor lenses.4 After treating only a small portion of the lens volume in donor lenses, the researchers measured an 8 percent transmission improvement. The Edinburgh work may enable in vivo monitoring of this treatment.
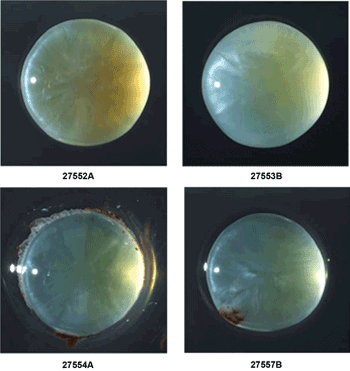
Human donor lenses from the Bristol Eye Bank reveal spectral responses similar to those obtained with pigs’ lenses in an experiment to explore early cataract diagnosis via tryptophan fluorescence: 80-year-old female (27552A); 79-year-old male (27553B); 60-year-old female (27554A); and 66-year-old male (27557B). Courtesy of B. Dhillon/Edinburgh Instruments.
In January, the project received several international development grants totaling €2.6 million (about $3.6 million) to continue the work.5 The researchers hope that the development “could save millions of pounds” in unnecessary operations and enable nonsurgical treatment of certain cases of cataract impairment.
Vision correction
Refractive laser surgery is the treatment of the cornea to correct myopia, hyperopia, astigmatism and presbyopia. One recent development in surgical vision correction is the use of wavefront aberrometry to measure the eye front to back. The technique maps in 3-D the subtle optical aberrations that affect vision. Called adaptive optics by astronomers – who use it to measure and correct aberration introduced by the atmosphere in real time – wavefront mapping enables custom lasik treatment. The map is transferred to the laser system and matched to the eye’s position. Surgeons then use the system’s cool blue excimer laser to resurface the cornea and correct for aberrations.
In all-laser refractive surgery, advanced femtosecond lasers replace the mechanical instruments called microkeratomes, which use a steel blade to create the thin circular flap on the outermost layer of the cornea. Also called IntraLasik, the technique has been in commercial practice for several years to treat myopia, hyperopia and presbyopia.
Late last year, laser system developer Lensar Inc. of Orlando, Fla., announced a clinical trial to study the use of a technique called lenticular softening to restore accommodation of the crystalline lens in presbyopic patients. Presbyopia is caused by a loss of elasticity in the lens, hardening it so that it has less accommodating (zoom) power to focus on nearby objects. The condition typically occurs in middle and old age and affects a billion people worldwide, according to the Archives of Ophthalmology.
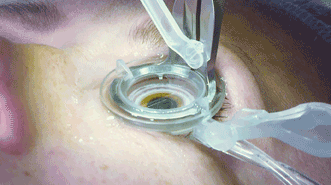
The Lensar Laser System prepares the patient for a surgical procedure using a liquid interface of a balanced salt solution to irrigate the eye and reduce laser incision pressure. Courtesy of Lensar.
“Presbyopia is the holy grail in ophthalmology,” said Lensar CEO Nick Curtis.
“We look forward to studying and expanding the body of data on the use of a femtosecond laser for lenticular softening with the eventual goal of accommodation restoration.”
An initial advanced feasibility study of 80 subjects demonstrated the Lensar laser system’s ability to soften the lens and restore accommodation, with notable improvement in BDCNVA (best distance-corrected near visual acuity).
Other conditions
For treatment of diabetes-related macular disease, a new treatment is available using a pattern scanning laser system (PASCAL). Developed by Stanford University spinout Optimedica of Sunnyvale, Calif., and acquired in 2010 by Topcon Medical Laser Systems of Santa Clara, Calif., the technology combines a PASCAL laser and proprietary software called Endpoint Management, which uses advanced titration algorithms that precisely control laser power and exposure times to optimize the therapeutic effect of the laser at less damaging levels. The laser therapy creates a user-defined pattern to treat the diseased area of the eye. The system produces subvisible photothermal stimulation, along with an option to enable visible reference dots so the physician can outline the treated area. The burns also can be left invisible.6
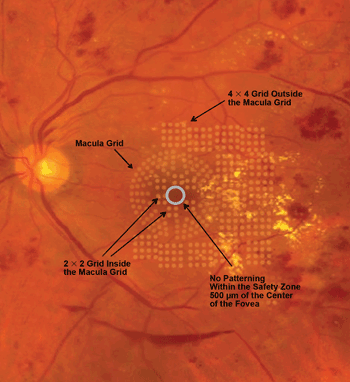
The fundus of the eye shows a pattern of grids placed by the PASCAL laser. The Endpoint Management software enables physicians to choose whether the burns are invisible or barely visible to provide a visual reference. Courtesy of Topcon Medical Laser Systems.
The technique significantly speeds up laser therapy for physicians by eliminating manual placement of spots one by one. The laser places patterns that automatically advance from point to point.
In February, Dr. Daniel Palanker – associate professor of ophthalmology in the Experimental Physics Lab at Stanford and a key contributor to the development of the PASCAL technology – received the SPIE Translational Research Award for his studies on nondamaging laser therapy.
His clinical partner in the research was Dr. Daniel Lavinsky, professor of ophthalmology at Federal University of Rio Grande do Sul in Porto Alegre, Brazil.
“The most exciting aspect of this advance is that it enables subvisible therapy,” Palanker said. “Physicians don’t have to see visible burns unless they need to. The shorter pulses also generate less pain, so patients love it.”
The technique leaves less scarring of the fragile surfaces of the eye. In current clinical trials of nondamaging therapy, this is especially important in the central area of the eye called the macula, where 90 percent of central vision is, Palanker said.
References
1. M.H. Niemz (2007). Laser-Tissue Interactions: Fundamentals and Applications. 3rd ed. Springer Berlin Heidelberg New York, p. 154. ISBN: 978-3-540-72191-8.
2. Dr. Sandra Belmont, Belmont Eye Center, New York, www.belmonteyecenter.com.
3. D. Gakamsky et al (April 2011). Exploring the possibility of early cataract diagnostics based on tryptophan fluorescence. J R Soc Interface, Vol. 8, p. 1616 (doi: 10.1098/rsif.2010.0608).
4. L. Kessel et al (March 2010). Non-invasive bleaching of the human lens by femtosecond laser photolysis. PLOS One, Vol. 5, No. 3, p. 1 (doi: 10.1371/journal.pone.0009711).
5. www.catacure.eu.
6. D. Lavinksy et al (2013). Subvisible retinal laser therapy: titration algorithm and tissue response. Retina, Vol. 0, p. 1-11.
7. S. Alsulaiman et al (February 2014). High-power handheld blue laser-induced maculopathy. J Oph, Vol. 121, pp. 566-572 (doi: 10.1016.j.ophtha.2013.09./006).
The Dangers of Blue Lasers
A wide variety of commercially available high-power blue laser devices can cause serious eye damage, according to a study published by the American Academy of Ophthalmology (AAO) in February.7 The study reports various types of maculopathy in 14 young patients who lost vision after brief exposure from a handheld blue laser device (wavelength 450 nm; measured output power 750 mW). It also found that only four of the injured eyes of the patients (29 percent) improved spontaneously, while 10 of the injuries required medical intervention, including vitrectomy (removal of blood and scar tissue).

Photo courtesy of Shinp.
The FDA, the Laser Institute of America and the American National Standards Institute have released warnings to the public that laser devices with an output power of more than 5 mW can severely damage the retina, even after momentary exposure.
However, handheld lasers of 1200 mW often are advertised online as “children’s entertainment.” Laser “stage show” lighting, common in the nightclub/entertainment industry for lighting up the smoky air with colorful animation, is also commercially available at output powers exceeding those considered eye-safe.
All too often, the actual wattage of the laser devices sold is actually higher than the manufacturers’ claims. The time it takes to cause injury is shorter than the eye’s blink reflex. The researchers who conducted the AO-published study emphasized that governments should take action, such as banning the importation of these high-power laser devices; consumers should be wary of looking directly at questionable laser sources.