Researchers complete preclinical trial of device on blood samples from patients.
David L. Shenkenberg Associate News Editor
According to the 2005 World Malaria Report by the World Health Organization and UNICEF, as many as 500 million malaria cases are recorded each year, resulting in at least 1 million deaths. Although a microscopic examination using a special stain has enabled accurate diagnosis of malaria for more than a century, most cases are contracted in poor countries that cannot afford numerous microscopes or trained microscopists.
Alternatively, antibody-based rapid diagnostic tests can diagnose malaria without a trained operator or the initial cost of the microscope. However, no current rapid diagnostic test can recognize all strains of the malaria parasite, and antibodies tend to degrade in the heat of the tropical and subtropical regions where the disease mostly occurs. Finally, these tests cost $1 to $4 per use. Although a few dollars might seem insignificant, the total testing costs amount to $500 million to $2 billion per year, considering the worldwide annual caseload.
In general, because people in malaria-ridden countries cannot afford existing diagnostic methods, anyone with symptoms receives malaria drugs. However, because of overprescription, several strains of the malaria parasite have developed a resistance to these drugs. Furthermore, the drugs can cause bad side effects.
Now, a collaborative effort worth €1.4 million in funding from the European Commission is producing a novel magneto-optical device that potentially would diagnose malaria without a trained operator at a cost of a few cents per use, which should help reduce the problem of overprescription. Additionally, unlike existing methods of malaria diagnosis, which require at least a finger prick of blood, it would operate noninvasively.
Currently, the magneto-optical device is in the prototype stage and is moving rapidly toward the final field instrument stage because its developers have proved that it can differentiate accurately between preclinical blood samples of patients with malaria and those with related diseases.
The magneto-optical device was conceived by Dave M. Newman at the University of Exeter and by John Heptinstall at Coventry University, both in the UK. Newman brought his magneto-optical engineering background to Heptinstall, a blood biochemist specializing in malaria. Newman’s group performed the development and testing, except for the preclinical testing on blood samples from patients, which was performed by researchers from Royal Tropical Institute in Amsterdam, the Netherlands
Like Polaroid
Newman and Heptinstall knew that the Plasmodium protozoan parasites that cause malaria live in the bloodstream and eat hemoglobin from red blood cells. Some of the hemoglobin breaks down into heme, which is toxic to the parasite. Therefore, the parasite nullifies the heme by converting it into hemozoin crystals, which are stored in its vacuoles. These crystals are always rod-shaped, some 800 nm long by 220 nm across and contain iron because they are derived from hemoglobin.

Researchers used a magnetic field to align these hemozoin crystals, which were produced by the malaria parasite, and then to interrogate the aligned crystals with a polarized laser. The change in transmittance related linearly to the concentration of hemozoin. Images reprinted with permission of Biophysical Journal.
The crystals therefore are weakly paramagnetic and will respond to magnetic fields. Their shape also gives them unique optical properties. Thus, the researchers use a magnetic field to align the hemozoin crystals and to focus a polarized laser on a blood sample. The aligned crystals absorb light from only one plane of polarization, and the concentration of hemozoin is revealed by the fractional change in transmittance as measured by a photodetector; that is, the transmittance after the application of the magnetic field is gauged as a fraction of the transmittance before. “So you have a weak polarizer like Polaroid sunglasses,” Newman said.
In initial experiments, the scientists used the device on blood samples to which they added hemozoin from either a strain of the parasite or from a synthetic analog of the crystal. They observed a striking linear relationship between the concentration of the hemozoin and the fractional change in transmittance. They could detect the low amount of hemozoin present in the ring stage of the parasite — an early stage in which not much hemozoin has been produced.
In the preclinical experiments at Royal Tropical Institute, the researchers compared the accuracy of the device against that of rapid diagnostic tests, in terms of their ability to correctly identify disease from blood samples. The patients had either confirmed malaria, fever symptoms, rheumatic-associated disease or hemoglobin disorders. The operator was blind to the status of the samples.
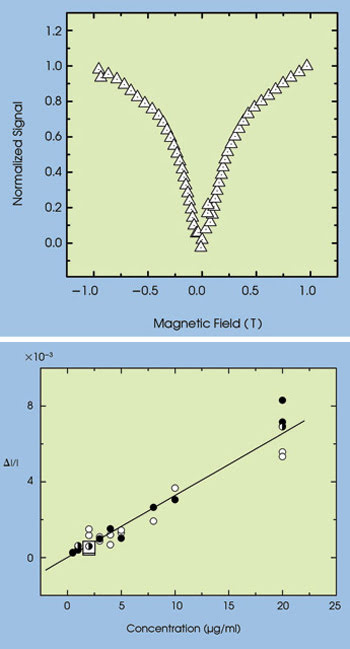
The image on the top shows that the polarity of the signal from hemozoin changes strikingly in response to a magnetic field cycled between 21 and +1 Tesla. The image on the bottom shows that the change in the transmittance (I) divided by the transmittance before the application of the magnetic field relates linearly to the concentration.
The investigators found that the magneto-optical device correctly identified 100 percent of the samples as either positive or negative for malaria, as verified by the rapid diagnostic tests. They noted that it was sensitive enough to detect P. ovale, which is known for its low concentration in the blood, as reported in the April 4 online publication of the Biophysical Journal. Although not a co-author of this paper, Philips Electronics has been working with the group to transform its concepts into a field instrument.
Into the wild
Further experiments are needed to refine the device into a field instrument. In the current prototype, a magnetic field of 1 Tesla is generated with an electromagnet. In their final field-ready instrument, they probably will use permanent magnets, Newman said. Because 1 Tesla is relatively strong, they hope to significantly scale down the magnetic field. Therefore, they need to determine the threshold field strength necessary to obtain a signal from hemozoin.
On the other hand, the prototype laser and detector may simply be miniaturized in the field-ready instrument using already-available small lasers and detectors, such as lasers used in displays. In the prototype instrument, a Blue Sky Research polarized laser at 660 nm is focused on the blood sample, and a Hitachi silicon photodetector detects the light transmitted through the sample. The team is likely to keep the 660-nm wavelength because small lasers are available in that wavelength, because it exploits a weak band in the spectrum of hemozoin, and because skin is transparent to it, which will be important for the noninvasive version of the device.
“This concept is the only one that really offers the possibility of noninvasive technology,” Newman said. He envisions that a patient with malaria symptoms would put his or her finger in an aperture of the noninvasive instrument. When the medical professional operating the machine presses a button, a magnetic field and laser would be applied to the finger, and results would be displayed on-screen instantly. He said that they have already semiautomated the procedure.
Newman said that both the invasive and noninvasive versions of the instrument will be transported to Africa, where local health professionals will use the devices on real patients. The location is particularly appropriate because most malaria cases and deaths occur south of the Sahara Desert.
He and his colleagues have devised a clinical trial that is expected to take place either at the end of this year or at the beginning of 2009. He noted that they must establish the relationship between the concentration of hemozoin and the severity of malaria infection.
He pointed out that global warming could lead to an increase in the Anopheles mosquitoes, which carry and transmit the malaria parasite outside of their tropical and subtropical regions. Thus, the malaria epidemic could spread beyond developing countries in the Americas, Asia and Africa to fully developed industrialized nations, rendering this instrument important not only for humanitarian purposes, but also for our continued way of life.