It’s no surprise that William Brown is certain the future of lasers in dentistry is bright. After all, he is a vice president at dental laser maker Biolase Technology Inc. in Irvine, Calif. But that feeling is based on more than his job. It rests, in part, on his being the father of a child who has had cavities filled without ever getting shots or encountering a drill. “It’s just been wonderful. Her first experience with going to the dentist was totally different than mine.”
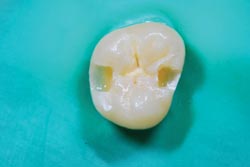
Side-by-side cavity preparations made with a dental laser system from Biolase Technology Inc. (left) and a high-speed drill (right), both completed in ~40 s. Courtesy of Biolase Technology.
The whirr of the drill hasn’t been replaced by the flash of a laser – at least not yet. But advances are allowing lasers to work their way increasingly into dental diagnostics and treatment. Laser-based optical coherence tomography, for example, soon could help highlight disease, while laser treatment of teeth could make them more resistant to cavities. When cavities do occur, lasers could remove the diseased tissue with less trauma. They even could make root canals more pleasant and successful.
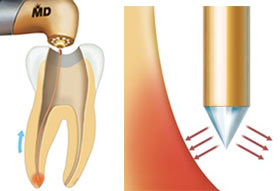
A specially designed radial firing tip provides disinfection during root canal procedures, achieving results that the manufacturer says are superior to those with conventional treatment. The design aims the laser energy deep into the wall of the canal to reach bacteria and prevents perforation of the bottom of the tooth. Courtesy of Biolase Technology.
Improvements such as different wavelengths and shorter pulses also promise to make lasers even more effective. However, problems, such as the cost of equipment and the speed of treatment, still loom.
On the treatment front, lasers offer significant advantages, said Joel White, professor in the department of preventive and restorative dental sciences at the University of California, San Francisco (UCSF). “All of the laser applications are less invasive and less destructive than conventional modalities.”
Lasers have been cleared for use in dentistry for years and, in some areas, have had significant market penetration. According to White, cavity detection by laser fluorescence is used by about half of the ~160,000 dentists in the US. The scheme works by highlighting the porphyrin rings present in the bacteria found in the pits and fissures of teeth, thereby revealing caries that a dentist might miss. The technique also does a good job of finding the disease early.
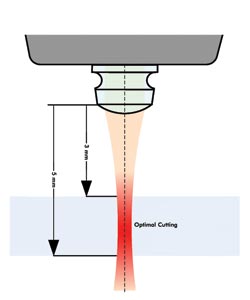
The speed of ablating hard tissue with a laser is increased, thanks to a new optical tip that refocuses the laser 3 to 5 mm beyond the tip. Courtesy of Biolase Technology.
However, in the treatment of those cavities, the speed of hard-tissue removal is important. A laser typically is more expensive than a drill and so can be a significant capital investment for a dentist. In the past, White said, lasers have been slower at removing tissue than a drill. The combination of cost and speed explains why the penetration of laser use for removal of hard and soft tissue runs only a few percent.
That may be changing, however. At the beginning of March, Biolase announced an upgrade that works with its existing lasers. It achieves speeds roughly comparable to those of a drill. It does so, Biolase’s Brown said, because of improvements in a number of areas. “It has to do with beam characteristics and pulsing and all the key parameters related to the laser. It’s the optics. It’s really a major refinement of the delivery system.”
The company also recently demonstrated laser root canal procedures without anesthetic on national TV. Again, the key is the delivery of the light. Typically, laser light arrives as a focused beam. If the wavelength is right and the pulses are of the correct duration, the energy from a laser will be absorbed by the tissue of interest, removing it with minimal effects on the surroundings. The result is little pain and almost no bleeding.
In a root canal, however, the soft tissue inside the tooth is removed. The challenge for a laser is to do this at the bottom of the tooth without perforating it. Biolase solved this problem by developing 200-µm-wide fibers that send the laser energy out to the sides and not down. The fiber is inserted into the root of the tooth and then drawn back, removing tissue from the bottom of the tooth up and providing 99.7 percent disinfection, results that approach complete sterilization. That’s a better figure than conventional methods claim. Because bacteria remaining in the canal after the procedure are a major cause for re-treatment, disinfection that is more complete could reduce the re-treatment rate.
The medical model
Lasers can be used as more than simply a drill replacement. On the diagnostic front, there is optical coherence tomography (OCT), a high-resolution imaging technique that penetrates tissue. Lantis Laser Inc. of Denville, N.J., hopes to win approval soon for a system and to bring one to market in the first half of 2010.
According to Stan Baron, president of Lantis, the system will use a swept-source microelectromechanical systems (MEMS) laser OCT engine based on frequency-domain OCT, which is a faster version than the time-domain implementation. The Lantis product, Baron said, will provide two-dimensional images of tissue in the mouth to a depth of 3 mm, courtesy of the OCT engine and a Lantis-developed handheld probe about the size of a pen.
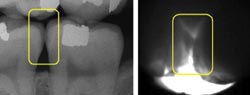
X-ray (left) and in vivo near-IR (right buccal-lingual view) images show two class II lesions on adjoining molars. A bitewing shows slight rarefied zone in lesion areas. Courtesy of Daniel Fried, UCSF.
“Utilizing a MEMS scanning mirror, the probe will give easy access to all areas of the mouth,” Baron said.
The system also will have near-infrared transillumination, which operates at the same wavelength as the OCT. The near-IR modality can highlight areas of interest that need further examination by OCT to determine severity and depth of a lesion. The development of cost-effective sensors now makes near-IR imaging commercially viable, Baron noted.
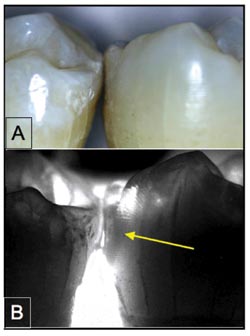
Shown are visible (A) and near-IR transillumination images at 1300 nm (B) of extracted teeth positioned in contact. The tooth on the right has an interproximal lesion (yellow arrow) that is visible with high contrast. Courtesy of Daniel Fried, UCSF.
Lantis is developing an imaging platform with OCT, near-IR, x-ray and intra-oral camera technologies in one system. The result, Baron explained, will be a device that can provide complete imaging diagnostics.
Dan Fried, a professor in the division of biomaterials and bioengineering at UCSF, noted that advances in technology could help dentists move more into a medical model. Diseases would be detected and treated. OCT, for example, allows dentists to see the beginning of a lesion and determine how deep it is. The area then can be remineralized, preventing the problem from developing into a cavity that must be removed and filled.
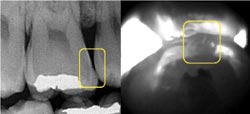
This comparison is of x-ray (left) and in vivo near-IR (right occlusal view) images of a class II lesion on a first molar. A bitewing shows that the lesion is small and only halfway through the enamel. Amalgam restoration appears in the center of the tooth. Courtesy of Daniel Fried, UCSF.
Perhaps the ultimate in prevention is being researched: Clinical studies with lasers are under way that could make teeth much more immune to disease, reported Fried. Natural tooth enamel has defects that make it susceptible to attack. Those weak points disappear if the enamel is heated above 400 °C. A short laser pulse can provide such heating on a spot basis without harming the patient.

In a new technique dubbed in vivo polarization-sensitive optical coherence tomography, B-scans for both linear polarizations of a sound premolar tooth can be scanned from the crown to the root. The dentin-enamel junction is visible along the entire scan. Courtesy of Daniel Fried, UCSF.
A UCSF research group led by John Featherstone is investigating low-energy-density pulses from carbon dioxide lasers as a means to heat up the outer few microns of the enamel and create a tough veneer.
The key, Fried said, is to have pulses of the right duration. “It’s on the order of a few microseconds.”