A new model focusing on translational research draws on the collective expertise of students, engineers and practicing physicians, encouraging collaboration from the earliest stages of the research.
Dr. Gregory P. Crawford, Brown University, and Dr. Gregory D. Jay, Brown University and Rhode Island Hospital
The direct application of engineering to medicine is a notable trend of the past decade. Noninvasive diagnostic technologies, high-resolution imaging, advanced materials implants and controlled-release drug delivery systems are just a few examples of innovations arising from the application of the principles of electrical, mechanical, computer, chemical and materials engineering to problems in medicine.
Approaches that combine the fundamental aspects of engineering with medicine are likely to yield a wealth of new directions for research and development; ultimately, these methods will lead to additional early diagnostic techniques and treatments. Advances in the medical-engineering partnership require engineers who are trained in methods that transcend the boundaries of traditional engineering disciplines.
The axiom “necessity is the mother of invention” characterizes our new collaborative model. The research and education partnership model drives advances in medicine through interdisciplinary collaboration of graduate and medical school students, engineering faculty and practicing physicians. This type of environment eliminates traditional disciplinary boundaries.
The model catalyzes a tight cooperation between engineers and practicing physicians. A network of physician/engineer teams clusters into focused research groups and addresses an interdisciplinary research problem arising from an identified medical need.
Initially a grassroots effort between several engineering faculty and physicians, the growing initiative between Brown University engineering faculty and local hospitals (Rhode Island Hospital, Memorial Hospital of Rhode Island and The Miriam Hospital, all located in Rhode Island and all working in partnership with the university’s Warren Alpert Medical School) has facilitated a larger research network of physicians, engineering faculty and students solving medical problems with photonics technology and engineering expertise. The research network capitalizes on resources from government and industry to create an efficient pathway for breakthrough medical innovations that will benefit society.
The model
Rather than relying on curiosity-driven research, the model is based on translational research — solving a medical problem with novel science and technology approaches and translating it to the bedside. The process usually begins with a formalized gathering of physicians and engineers focused on an a priori defined theme — a brainstorming session, so to speak. With one or two slides, the participants “pitch” their idea in a few minutes. Practicing physicians identify current medical problems in need of a science or technology solution, and engineers define science and technology that potentially could solve the problem. From this initial session, ideas are selected by groups of researchers based on participant interest and resident expertise, thereby forming an interdisciplinary interest network.
Before the onset of the project, the necessary approvals and infrastructure are addressed by the team; for example, health information protection training is given to participants, and institutional review board approvals necessary for human subject involvement are obtained. The team, in both the university laboratory and in the hospitals, then formally launches the research project. Because study preliminaries are set in motion at the onset of the project, the approvals are usually in place as the science and technology solution matures to a point where it is ready for clinical evaluation and for use on human subjects.
For successful projects to benefit society, a mechanism must be in place to transfer the team’s solution to the marketplace. In our model, we leverage the university’s entrepreneurship programs, where participating students in cooperation with faculty and physician mentors as well as the local business community can engage in intellectual property due diligence, in market definition and feasibility studies, and in business planning in parallel with their science and technology thrusts. The entrepreneurial approach often is initiated at the onset of the projects as well, so those that successfully culminate in a working prototype are ready to be launched into product development (Figure 1).

Figure 1. The authors have described a collaborative model designed to facilitate advances in medicine by taking advantage of the collective expertise and interdisciplinary efforts of graduate and medical school students, engineering faculty and practicing physicians. HIPAA = Health Insurance Portability and Accountability Act; IRB = institutional review board.
Diagnosing anemia
Given the nature of the biophotonics field and the promise of noninvasive diagnostic technologies and rapid diagnostic techniques, our model has focused largely on projects with an underlying photonics thrust. The case studies described below demonstrate examples of the engineer-physician model of cooperation.
One problem we have addressed using this model is the diagnosis of anemia. The World Health Organization reports that anemia is the single largest global illness adversely affecting mortality and the second leading cause of disability. To determine whether a patient is anemic, the physician either can visually inspect the palpebral conjunctiva (lower eyelid) or perform a cell blood count test.
Visual inspection (qualitatively assessing the redness of the conjunctiva) is inaccurate even for the experienced physician; thus, typically it is used only as a quick screening approach. Hung et al showed that physicians today are less accurate than those of the past.1 The cell blood count test is very accurate, but it is painful to the patient, expensive to perform, takes time to analyze and often is not part of a routine physical exam.
In one of our formalized gatherings, we noted a compelling need for a tool that can measure hemoglobin accurately, quickly and inexpensively and which could be as ubiquitous and useful to health care professionals as a stethoscope or sphygmomanometer. We then assembled a physician-engineer team consisting of a PhD student in biomedical engineering, a faculty member in electrical engineering and three emergency medicine physicians. The group developed a technique and device to monitor blood hemoglobin concentration noninvasively (without needles).
The concept is a handheld visible spectrometer manufactured on a wafer using inexpensive liquid crystal technology that examines the optical properties of blood vessels in the conjunctiva — the same location that physicians currently visually inspect for a qualitative assessment of hemoglobin. The spectroscopic imaging platform enables the measurement of hemoglobin in patients in less than 1 s by taking a visible spectrum of the palpebral conjunctiva.
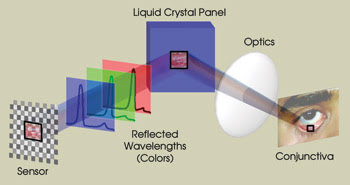
Figure 2. One result of the collaborative efforts is a liquid crystal spectrometer, a tool that can measure hemoglobin accurately, quickly and inexpensively and, thus, can contribute to the diagnosis of anemia. This spectroscopic imaging platform acquires the visible spectrum of the palpebral conjunctiva and enables clinicians to perform measurements in less than 1 s.
The conjunctiva is irradiated with visible light, and the reflected optical signal is imaged using a tunable reflective liquid crystal display-type panel (Figure 2).2 The panel is tunable so that it can reflect various wavelengths at various times — typically very fast, less than 1 ms per wavelength — which are recorded on a sensor so that the true spectrum of the conjunctiva can be reconstructed. An algorithm, based on a partial least squares approach, transforms the spectrum into a measurement of the hemoglobin level to assess the degree of anemia.
To date, clinical studies on two evolving prototypes of the optical device have been conducted,3 the first in 2005 at the Davol emergency department at Rhode Island Hospital and the more recent one in 2006 at the new Andrew F. Anderson Emergency Center at the same hospital, with more than 150 patients enrolled in these studies (Figure 3).
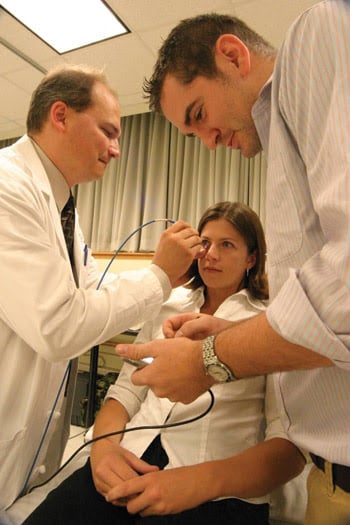
Figure 3. The work has produced two prototypes of the liquid crystal spectrometer that have been tested in clinical studies. More than 150 patients have been enrolled in the studies.
Another problem we have addressed is fetal twin-to-twin transfusion syndrome, which occurs when fetal blood vessels in the placenta between twins are erroneously joined together rather than to the maternal vessels. Mortality rates are extremely high for both twins if this condition goes untreated.4 Fetal twin-to-twin transfusion syndrome disorder currently is treated with a laparoscopic ablation of problematic vessels, identified by subjective visual observation by the surgeon through a camera using a fiber laser.
To improve the precision of the procedure, a team consisting of a biomedical engineering PhD student, an undergraduate biomedical engineering student, an electrical engineering faculty member and a pediatric surgeon retrofitted the spectroscopic tool described in the first case study into a laparoscopic device to aid in accurate, quantitative identification of problematic blood vessels in fetal twin-to-twin transfusion syndrome.
This tool, a fiber optic probe fed through an endoscope equipped with a spectrometer, aids the surgeon in identifying blood vessels linked between the twins by using additional fibers and by quantifying blood flow, saturation and total hemoglobin concentration of the individual vessels using fluorescence, Doppler shifting and spectroscopy. This solution enables the surgeon to identify the linked vessels accurately, with a method that is quantitative, rather than visual, to determine precisely which vessels to ablate.
Since late 2006, clinical studies with the tool have been under way at Hasbro Children’s Hospital, the pediatric division of Rhode Island Hospital, with seven patients enrolled in the laparoscopic data collection to date. The team is perfecting the method of vessel identification and is working with partner hospitals to integrate this technology into laser vessel ablation tools for fetal twin-to-twin transfusion syndrome therapy.
Determining age of bruises
Another problem solved using our model involves the ages of contusions. Pediatricians and other physicians who care for acutely injured patients often are asked for an opinion regarding the age of externally visible contusions (e.g., bruises); however, studies have shown that this assessment is highly inaccurate and seems to be no better than chance alone. There is a need to date accurately the age of a bruise. For example, in a suspected child-abuse case, a physician who notices a suspicious bruise usually tries to determine whether the age of the bruise and its appearance correspond with the explanation from the child and guardian of how the injury was sustained — in many cases, the age of the bruise is needed for this correlation.
The team that addressed this problem consisted of an undergraduate premedicine major, a PhD student in biomedical engineering, an electrical engineering faculty member and a pediatric emergency medicine physician using a spectroscopic tool to quantify the age of a bruise for forensic and child protection purposes. This physician/engineer team is exploring diffuse reflectance spectroscopy and digital image analysis to develop a quantitative model for extravascular hemoglobin breakdown and to determine noninvasively the age of a bruise.
This team has been enrolling patients at Hasbro and at other Rhode Island hospitals since 2005, with more than 30 adults and children recruited for the analysis. Further work from this group involves investigating infrared signals from contusions as well as quantifying bruise depth to add to the optical model.
Sepsis detection
Sepsis is the systemic response of the body to a localized infection. Bacterial infections are responsible for 90 percent of the reported cases of sepsis. In 2000, there were nearly 660,000 cases of sepsis in the US alone, with an in-hospital mortality rate of 17.9 percent.5 Currently, however, no bedside diagnostic is available to positively identify patients with sepsis.
A PhD student in biomedical engineering, a PhD student in physics, an electrical engineering and a physics faculty member, and two infectious disease physicians therefore are using adaptations of liquid crystal display technology to develop a bedside diagnostic device for rapid diagnosis of sepsis.
The sensor, which utilizes the unique properties of liquid crystals to detect optically the presence of a biological marker for sepsis, has shown the ability to detect very low, clinically relevant levels of lipopolysaccharide, which is released from the outer membrane of bacteria during infection. Brake and co-workers6 first demonstrated the technology, where liquid crystals in open-faced liquid crystal pixels (300-μm containers) were placed in direct contact with biological molecules. Ongoing research has shown that the interaction of a lipid in the biomarker with the liquid crystal results in a configuration change in the liquid crystal and a subsequently observable optical effect (Figure 4a).
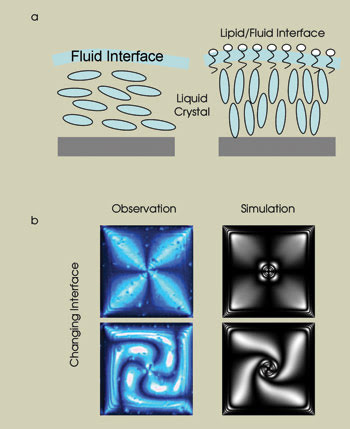
Figure 4. The physician-engineer teams also are developing a sensor that utilizes the unique properties of liquid crystals to detect optically the presence of a biological marker for sepsis. A lipid in the biomarker interacts with the liquid crystals in such a way as to produce a configuration change in the crystals and a subsequently observable effect (a). In b, images of the liquid crystal pixels are modeled, along with subsequent optical modeling of the macroscopic texture. The interaction energy at the liquid crystal-lipid interface is correlated with the concentration of the target biomarker.
Leveraging the early work of Brake et al, the team set out to quantify the subtle features of the optical microscope images using optical simulation algorithms to model the observed optical texture (Figure 4b). The team is conducting concentration studies of the lipopolysaccharide marker at Memorial Hospital of Rhode Island to understand the lower limits of concentration that can be detected.
Lifelike mannequins
Finally, we are working to address some limitations of medical training. A solely practice-based approach to teaching clinical skills is increasingly inadequate because of the speed and complexity of medical advances, cost-containment issues, patient safety concerns and time pressures. Thus, there is an increased reliance on simulation technology to strengthen learner knowledge, to provide a safe and risk-free practice environment and to shape the acquisition of health care professionals’ clinical skills.7
High-fidelity mannequin simulators allow basic procedural practice and enable immersive scenario situations for trainees to home in on and perfect, and during which they can reflect on critical diagnostic and management skills. However, a lack of situational realism still remains — in particular, the inability to create accurately a lifelike mannequin skin. Mannequin skin is passive (with no functionality) and does not replicate accurately human skin color, appearance, or responses to physiologic or pathophysiologic changes and external inputs.
To remedy this, faculty members in physics and in electrical engineering, and four emergency medicine physicians and specialists in medical simulation therefore are developing a novel electro-optic technology that would emulate various skin appearances on medical-simulation mannequins.
This solution involves unifying electro-optical materials and medical science expertise to develop materials that emulate the cutaneous characteristics of skin for medical-simulation mannequins. The approach involves the innovative integration and development of liquid crystal and polymer materials that are electro-optically active to create, for example, changes in skin color (a yellow skin color to mimic jaundice, grayish-blue skin for cyanotic patients and reddish lesions for petechiae). This technology also creates tunable topological features to emulate rashes and goose bumps, and polymer approaches to mimic piloerections (raised hair). To change the skin color, for example, the paint-on cholesteric liquid crystal material technology used in reflective flat panel displays can be integrated with flexible substrates and conformed to certain areas of the mannequin skin to create a new set of simulated ailments (Figure 5).
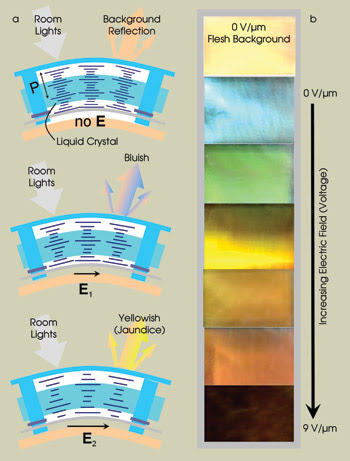
Figure 5. Another team has drawn on the expertise of its members to develop materials that mimic the cutaneous characteristics of skin for use in medical-simulation mannequins. The effect is shown in a, where the reflected color of a liquid crystal panel changes with applied voltages (electric fields). The applied electric fields change the inherent chiral pitch, P, of the liquid crystal material, which Bragg-reflects incident room lighting. The material reflects blue light at low voltages and shifts into the red for higher applied voltages, as demonstrated in b.
Integrated novel cutaneous responses in medical-simulation mannequins will enable improved training for health care professionals by greatly expanding the scope of simulation scenarios and introducing a greater sense of realism into the medical-simulation theater. The team currently is working on developing larger-area sample sizes and on evaluating them in the medical-simulation theater at Rhode Island Hospital’s Medical Simulation Center.
Translation and transfer
We have integrated into our model the requirement that research be translated into societal and human value. In our model, it is not enough to bring the biophotonics technology to the clinic and to test the approach. Rather, it is our philosophy that to truly benefit society more broadly, these projects must be accelerated toward potential commercialization.
This is accomplished largely through a one-semester class. “Innovation and Entrepreneurship,” a graduate-level course offered by the division of engineering at Brown University, engages students in a series of value-creation exercises revolving around their research project. The result is a full business plan addressing the market space, intellectual property barriers and opportunities, marketplace competition, billing and reimbursement mechanisms for the hospitals, further clinical evaluations, FDA approvals, expansion of the team to include business professionals, etc.
The course usually is taken at the onset of the project; if the project culminates with a successful clinical evaluation, the team can move forward immediately to retain its momentum. We believe that this entrepreneurial approach will increase the probability that the research will have an impact on society; if the group cannot implement its findings right away, the training will influence greatly the team’s outlook on future research projects. It is interesting to note that the early market and intellectual property due diligence greatly benefits the basic research as well, uncovering new ideas and approaches to the problem at hand.
To date, one of these projects has spun off into a company, and others are in the intellectual property or business planning process and building toward a spin-off company or technology transfer to industry. Irrespective of the outcome, however, students, faculty and physicians find great value in competencies and skills associated with entrepreneurial exercise.
Furthermore for students, the entrepreneurship experience fosters independence, innovation and the feeling of being the sole proprietor of one’s future career; the experience matures students at a time when they are thinking carefully about postgraduation career options. Through our model, the students acquire interdisciplinary training in engineering and medicine, an in-depth knowledge base in their chosen discipline, the necessary skills to create societal value out of translational research, and the requisite skills to become leaders and creative agents of change.
The physician-engineer model provides a mechanism whereby those involved in traditionally strong engineering programs that do not necessarily have a biomedical component can be brought to the interface between the engineering and medical communities in a way that ensures effective problem selection by the engineers. The model is a directed effort at cutting to the technical heart of a problem identified by practicing physicians and providing a mechanism by which faculty and students with deep knowledge in a traditional engineering field can become involved in a partnership to create a solution. It emphasizes the step beyond the traditional publication of results, bringing the participants into the actual development and implementation phases of inherently translational research.
The model strives to enable a greater proportion of the engineering community to become involved in medical engineering and translational research. It does so without requiring a large investment of time developing a background in biology and medicine and instead draws upon the concept of a team building upon each other’s in-depth expertise and core training in clinical and translational research.
Meet the authors
Gregory P. Crawford is dean of engineering and a professor of engineering and physics in the engineering division at Brown University.
Gregory D. Jay is the associate chairman of research and an associate professor of emergency medicine at Warren Alpert Medical School at Brown University, and he is the director of research in the emergency department at Rhode Island Hospital; he is jointly appointed as an associate professor of engineering.
References
1. O.L. Hung et al (2000). Evaluation of the physician’s ability to recognize the presence or absence of anemia, fever, and jaundice. ACAD EMERG MED, Vol. 7, pp. 146-156.
2. J.W. McMurdy et al (Aug. 21, 2006). Monolithic microspectrometer using tunable ferroelectric liquid crystals. APPL PHYS LETT, 081105.
3. J.W. McMurdy et al (Jan. 1, 2006). Diffuse reflectance spectra of the palpebral conjunctiva and its utility as a noninvasive indicator of total hemoglobin. J BIOMED OPT, 014019.
4. F.I. Luks et al (July 2005). What — and why — the pediatric surgeon should know about twin-to-twin transfusion syndrome. J PEDIATR SURG, pp. 1063-1069.
5. G.S. Martin et al (April 17, 2003). The epidemiology of sepsis in the United States from 1979 through 2000. N ENGL J MED, pp.1546-1554.
6. J.M. Brake et al (Dec. 19, 2003). Biomolecular interactions at phospholipid-decorated surfaces of liquid crystals. SCIENCE, pp. 2094-2097.
7. J. Vozenilek et al (November 2004). See one, do one, teach one: Advanced technology in medical education. ACAD EMERG MED, pp. 1149-1154.