
Near-IR spectroscopy jumps to the rescue
Clinicians are using near-IR spectroscopy to study normal blood oxygenation levels in the lower extremities, noninvasively and in real time. The results could help investigators understand perfusion abnormalities and complications resulting from various leg injuries, such as acute compartment syndrome (ACS), a condition occurring in approximately 10 percent of closed tibial fractures and in 20 percent of all intensive care injuries. Perfusion is the delivery of nutrients to tissue via the bloodstream.
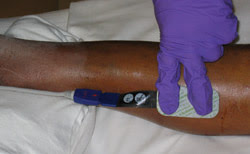
Near-IR spectroscopy measures oxygenation levels by using small adhesive sensor pads placed over a muscle compartment of the extremity at the mid-tibia level. Measurements corresponding to four compartments – anterior, lateral, deep posterior and superficial posterior – were taken for each leg.
“To understand abnormal perfusion, we must first understand normal perfusion,” said Dr. Michael Shuler, lead researcher of a study published June 1 in The Journal of Bone & Joint Surgery (JBJS) and a specialist in micro- and upper-extremity surgery at Athens Orthopedic Clinic.
His research has increased understanding of the functional changes involved in ACS, which is the swelling of a closed muscle compartment and the resulting reduction of perfusion to the injured site. In response to an injury, oxygen saturation surrounding a traumatized area is increased. “Oxygen delivery is required for healing at the injury site,” Shuler said.
Natural restoration
Shuler’s study examined hemoglobin oxygen saturation levels in 51 patients. A group of 26 subjects had acute unilateral tibial fractures, while the control group of uninjured subjects numbered 25. Tibial fractures were examined because of their association with ACS.
Hemoglobin oxygen levels were measured from 2 to 3 cm below the skin’s surface at wavelengths of 690 to 880 nm. Two wavelengths were used to solve for two unknowns, oxygenated and deoxygenated hemoglobin values, as hemoglobin’s absorption of light varies according to its oxygenated state. Each subject’s contralateral –that is, uninjured – limb served as an internal control for comparison of oxygen levels.
In both groups, four compartments of each leg – anterior, lateral, deep posterior and superficial posterior – were measured using an in vivo optical spectroscopy cerebral oximeter at the mid-tibial level. The device used disposable adhesive sensor pads, which were placed on the leg for approximately 30 to 60 seconds. “A value was obtained after a consistent reading for four consecutive cycles of six seconds,” Shuler said.
For the control (uninjured) group, the average tissue oxygenation level was 54 percent for anterior, 55 percent for lateral, 60 percent for deep posterior and 57 percent for superficial posterior. The lower-extremity trauma group presented a mean oxygenation level of 69 percent for anterior, 70 percent for lateral, 74 percent for deep posterior and 70 percent for superficial posterior. Those with injured legs averaged 15.4 percent higher hemoglobin oxygen saturation levels than the control group.
Monitoring ACS
Currently, to diagnose ACS, doctors insert a large-bore needle into the muscle at the fracture to measure intramuscular pressure in the tissue. However, the results can be unreliable if the method is not performed correctly, and the needle must be inserted in all four compartments of the leg for an adequate analysis.
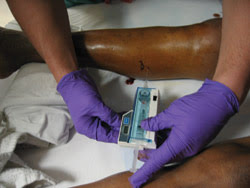
To diagnose ACS, a large-bore needle must be inserted into each compartment of the leg to obtain intracompartmental pressure measurements. Current treatment for ACS involves a fasciotomy, which relieves pressure but can lead to muscle and nerve ischemia or infection. Researchers hope that near-IR spectroscopy will help detect the disorder earlier, reducing the need for fasciotomies.
Treatment for ACS involves a complex surgical procedure called a fasciotomy, which requires an incision to relieve pressure and can result in severe functional deficits or infection. “If not treated acutely, the hypoperfusion can lead to muscle and nerve ischemia and ultimately necrosis,” Shuler said.
In a follow-up article submitted to JBJS, Shuler studied near-IR spectroscopy as a real-time, noninvasive and continuous monitoring system for hemoglobin oxygenation saturation in ACS patients. The method may allow for early detection and treatment, reducing the number of unnecessary fasciotomies.
Published: September 2009