The concept behind a picture archiving and communications system, or PACS, is pretty straightforward: Acquire medical information about a person, including digital images and basic health-related and personal data, and make it all accessible to doctors, hospitals and their staffs at anytime and at any location.
Until two decades ago, this was just a pipe dream – and a feverish one at that. Medical imaging primarily comprised analog x-ray scans that were printed on film, then passed among technicians, readers and physicians. If you had more than one doctor helping you with a sore knee – say, a family doctor and an orthopedist – copies of the relevant x-ray images would have to find their way to both.
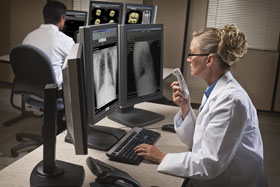
Picture archiving and communications systems (PACS) continue to spread out across the medical community. Courtesy of Agfa Healthcare.
There was already a building hue and cry for a better way to track patients’ image-related records when the first digital imaging technologies arrived in the late 1970s and early 1980s. Computed tomography (CT) came along at about this time and, although not adopted quickly or widely, the technique did trigger a thought that perhaps all imaging could be acquired, stored and passed along in a digital format.
That thought has very nearly become a fully realized reality, with PACS equipment installed in about a quarter of all hospitals in the US. Increasingly, doctors, dentists, radiologists and even emergency responders are adopting PACS as part of their everyday functions, and PACS manufacturers are developing new features to lure more users into deploying it.
A little history
In the 1980s, CT and similar digital diagnostic tools firmly began to capture the imagination of people working in various fields of medicine. By 1983, the American College of Radiology (ACR) and the National Electrical Manufacturers Association decided that there was enough interest in digitization that they should work together to develop new standards to deal with the capture, storage and manipulation of digital information. Over the course of about a decade, the two groups created DICOM (Digital Imaging and Communications in Medicine).
 DICOM features a number of tenets for practical communication of medical imaging data, but it essentially was meant to forestall one particular expected problem. Beyond CT and digital x-rays, existing imaging modalities were expected to go all-digital, and new modalities would be created; if each had its own set of standards, chaos would ensue. Too many standards, and the complete information required to treat a patient could never be brought together in the system. Medical staff would require banks of monitors to see every image or dataset needed to treat a patient, various types of data would have different storage requirements and recall abilities, and important correlating information would not become available, such as matching electrocardiogram data with an x-ray or an MR or CT image.
DICOM features a number of tenets for practical communication of medical imaging data, but it essentially was meant to forestall one particular expected problem. Beyond CT and digital x-rays, existing imaging modalities were expected to go all-digital, and new modalities would be created; if each had its own set of standards, chaos would ensue. Too many standards, and the complete information required to treat a patient could never be brought together in the system. Medical staff would require banks of monitors to see every image or dataset needed to treat a patient, various types of data would have different storage requirements and recall abilities, and important correlating information would not become available, such as matching electrocardiogram data with an x-ray or an MR or CT image.
Movers and shakers
The earliest ideas that a single system could corral pictures and information from widely different technologies and locations and make them available to anyone had been floating around since the early 1970s, but the development of the DICOM standards made the possibility come to life.
Pioneers such as Steven C. Horii, now of the Hospital of the University of Pennsylvania in Philadelphia, and Samuel J. Dwyer, the “Father of PACS,” who died in 2008, pushed through the early attempts at a unified, all-digital system.
Dwyer, for example, oversaw the installation of the first fully realized PACS setup, which was built in 1983 at the University of Kansas. Horii, for his part, led the way in convincing manufacturers of imaging equipment to jump onboard. The ACR and the US Food and Drug Administration added pressure of their own on the device makers, but also provided relief that the manufacturers would not be charged with collusion if they used the same standards of interoperability.
By the mid-1990s, going digital was the driving force in the imaging industry, although there have always been holdouts who maintain – often rightly, some studies have shown – that analog images are easier to read and, thus, better for diagnosing some diseases. Radiologists who work primarily in mammography, for example, are only now starting to use digital scans more, as quality improves.
Challenges remain
PACS is not yet ubiquitous. About 22 percent of all hospitals in the US have some variety of it installed, mostly in larger hospital systems, not in rural centers. Medical and dental offices and emergency rooms and clinics are adopting PACS at a steady rate as well. Vendors offer systems that excel at one type of imaging modality; other vendors sell beefed-up versions that span the gamut of possible needs (see Table for a short list of available modalities).
“PACS is already expanding to support other imaging and nonimaging departments, such as ophthalmology, pathology, cardiology and others,” said Neville Skudowitz, product line manager at Carestream Health in Rochester, N.Y. “Modern PACS platforms are adept at managing and storing images within the radiology department, which is a complex process. What PACS, in general, lacks is the ability to deliver similar work flow for other, nonradiology, departments.”
Despite the steady, if protracted, rollout, PACS is hampered by uncertainty in several technical and logistical areas. Chief among these is the overall efficiency of the systems. Manufacturers and vendors from Agfa Healthcare to Siemens to GE and others report that tighter integration of imaging and patient data is required to shorten the time it takes to get from diagnosis to treatment, and then to track treatment efficacy.
Part of the efficiency equation concerns security; any data must be stored securely and transmitted in an encrypted format to be safe from hackers. Data from a variety of sources must be properly matched as well to ensure that one patient’s lung x-rays aren’t mixed in with another patient’s MR images.
Another big challenge ahead is to unlock PACS from displaying to only one spot within an organization. Data must be able to appear wherever medical personnel are; it must be portable where it has not been until now. That does not mean simply that a doctor can view patient data in the ER, then in the surgical suite, then in her office. It means that the images and other information are available to radiological readers working from average PCs at home, to nurse practitioners using netbooks inside rural clinics, to telemedicine practitioners accessing records from smart phones.
Several PACS manufacturers, including GE, are embracing Internet access, using Web 2.0 principles to provide data sharing and interoperability between products and systems, even among those from different vendors. With Web-based access, a reader or physician does not need to install proprietary software at any new station he might use.
Metasystems also can provide interoperability among systems. According to Skudowitz, Carestream Health’s SuperPACS allows radiologists in particular to gain access to a unified set of imaging studies created from other vendors’ PACS.
A social push toward digitization of all patients’ records, including imaging, plus a technological impetus for all-inclusive availability, means that PACS will continue to evolve rapidly. Someday, perhaps, there may even be an iPhone app for that.