As life expectancy increases, our eyes bear the brunt of aging; many of the elderly suffer from vision problems. One of the leading causes of eye problems in the Western world is macular degeneration. To correct this, retinal implants, generally consisting of about 60 electrodes, have been inserted into the back of the eye. The patient wears glasses incorporating a tiny camera that views what the patient normally would, and the camera sends the image data to a minuscule computer. The computer converts the data to electrical signals, which are sent to the implant and processed by the brain. While garnering attention, these implants have yet to truly restore vision that’s any sharper than fuzzy images.
A multidisciplinary team led by Daniel Palanker from Stanford University in California is taking implants a step further using LCD technology, the infrared spectrum and photovoltaics. While the study subject is wearing what look like goggles with an LCD screen inside, the image on the LCD screen – the image the patient would normally see – is projected with pulsed infrared light onto photovoltaic cells implanted under the retina. The photovoltaic cells convert the light signals into electrical impulses, which then stimulate retinal neurons above them. The current design includes about 1000 photovoltaic pixels.
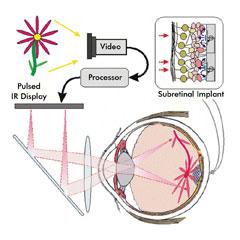
A diagram of the photovoltaic retinal prosthetic system includes a video camera, an image processor, a pulsed infrared microdisplay inside video goggles and a subretinal photovoltaic array.
There are some important differences between this approach and a traditional implant. One is the quality of the image produced, and another is the fact that patients don’t have to move their heads, rather than their eyes, to perceive an image. With traditional implants, the image changes when the camera moves – that is, when the head rotates. In normal-sighted people, on the other hand, visual perception is dependent upon continual eye movement, which refreshes the image. The photovoltaic retinal prosthesis retains this natural link between image perception and direction of gaze.
Another advantage to this new method is that the implant is made of flexible silicon, so it can fold and bend over the shape of the retina. This allows for a close fit, which helps maintain a close contact between the electrons and neurons.
In people who are suffering from retinal degeneration, the photoreceptor cells slowly deteriorate while many of the retinal neurons that process the signals from the photoreceptors and send them to the brain still survive and are able to function. When those neurons are mechanically stimulated, so-called “phosphenes” are produced, which give the perception of light.
The challenge, however, is that thousands of pixels are needed to restore sight to a useful level. In addition, those pixels must be delivered at video rate, the electrodes must be very close to the target cells, and signal processing must sufficiently compensate for the partial loss of the retinal neural network, among other complications. The system designed at Stanford, therefore, was, by necessity, a multidisciplinary effort.
Included in the new implant system is a data stream from a video camera, which is processed by a computer. The images displayed on the LCD microdisplay are illuminated by a pulsed 0.5-ms near-infrared light (900-nm wavelength), which projects the image through the optics of the eye onto the retina. The infrared image is received by the photovoltaic pixels in the chip implant.
The team is currently working on fabricating and testing the photovoltaic arrays in vitro and in vivo. The researchers are also studying the effects of retinal degeneration on circuitry and are developing software that will take over some of the retina’s functions, allowing patients to fine-tune their implants, much as an optometrist adjusts lenses according to our vision.