Getting around the elephant in the room
There’s a prodigious pachyderm in the parlor, but nobody is able to agree on just how big it is or whether it is about to rampage through the house. The beast, of course, is the Patient Protection and Affordable Care Act (The baby hanging onto momma’s tail is the Health Care and Education Reconciliation Act). While the acts – more commonly known together as health care reform – were not the only story affecting the biophotonics industry in the first half of the year, they certainly trumpeted loudly and often enough to keep one’s attention.
 The original impulse behind health care reform legislation was to get more uninsured Americans into some sort of insurance program, thus providing cost reduction pressures that could ease the strain on existing programs such as Medicaid. In theory, the $940 billion of spending needed to implement the bill over the next decade would be offset by the total amount saved on such existing programs. The new law, however, also derives some funds from additional fees and taxes on medical device makers, including those developing and building photonic devices.
The original impulse behind health care reform legislation was to get more uninsured Americans into some sort of insurance program, thus providing cost reduction pressures that could ease the strain on existing programs such as Medicaid. In theory, the $940 billion of spending needed to implement the bill over the next decade would be offset by the total amount saved on such existing programs. The new law, however, also derives some funds from additional fees and taxes on medical device makers, including those developing and building photonic devices.
Beginning in 2013, a 2.3 percent excise tax will be levied on many medical devices. Consumer products commonly found in retail stores, such as eyeglasses and hearing aids, are not subject to the tax; however, CT scanners, surgical lasers, endoscopes and a host of other devices large and small, which are sold chiefly to clinics and hospitals, are.
Under health care reform provisions affecting government reimbursements, CT and MRI scanners and any other medical device that costs more than $1 million will be presumed to be used 75 percent of the time a clinic is open. That is up from 50 percent and will likely reduce reimbursements to smaller, more rural – and less active – imaging clinics.
According to some estimates, this tax would put a $20 billion burden on manufacturers, even as some struggle to recover from the recent deep recession. Younger companies, especially startups, may be most adversely affected because they usually have just one product in the market. This is a disadvantage compared with more mature companies, which typically get revenues from a catalog of low-cost retail items that aren’t subject to the excise tax. The smaller companies also are not well positioned to sell into the international market, where taxes are less extant.
Trade associations such as the Advanced Medical Technology Association and the Medical Device Manufacturers Association, both based in Washington, have decried the device tax. They argue that it will harm companies’ bottom lines in general and slow (or cease) innovation because smaller companies are responsible for most of the advances in medical device technology.
A presumptuous assumption
The health care reform and reconciliation acts also make an important change to Social Security’s consideration of imaging services. Until now, government reimbursement for medical imaging has been based on the assumption that any given piece of equipment is used half the time the technician’s office is open for business. The difference between the actual availability and the assumed availability drives the fee.
The new law stipulates that the assumption increase to 75 percent for any imaging equipment that costs more than $1 million, which would include CT and MRI devices, among others. Nuclear medicine and positron emission tomography systems – initially included in the reform act – were spared by the reconciliation act.
According to the American College of Radiology (ACR), the immediate effect of the new utilization assumption will be to decrease the total amount of imaging that takes place. The rationale is that smaller, more rural imaging clinics – which typically have utilization rates below 50 percent – will be forced to end services because of a drop in reimbursements. Furthermore, patients will be forced to drive to larger, more urban hospitals and imaging centers, increasing commutes and wait times. Presumably, many patients will opt out of imaging altogether if it is unavailable closer to home.
The reform act made a couple of other changes that nibble at reimbursements for imaging services: The discount rate for imaging contiguous body parts on a patient increased from 25 percent to 50 percent. An identical rate change was enacted for same-day patient imaging.
Whither imaging?
There is disagreement over whether the overall amount of imaging will increase. The framers of the legislation expect that 32 million Americans will newly become carriers of health insurance, thus leading to more preventive care and fewer trips to the emergency room for nonurgent care. The further assumption is that various diagnostic services, including imaging, will expand. The ACR, however, disagrees, asserting that imaging today is mainly performed on anyone requiring medical care, whether they are insured or not. Therefore, despite the expected increase in the number of people who will have insurance, there will be a limited number of new patients receiving imaging services.
Lastly, the health care reform and reconciliation acts also put in place a general fee on the medical device industry as a whole. The new fee will collect $2 billion per year from 2010 to 2017, and $3 billion annually after 2017. Device makers (and importers) with US sales of $5 million or less are exempt from the fee; companies with US sales of $5 million to $25 million would pay half the tax.
Another possible effect of the aforementioned increase in the imaging equipment utilization assumption is that the smaller, rural clinics might artificially inflate usage to meet the 75 percent figure. Overprescription of imaging services would likely lead to unnecessary increases in patients’ radiation exposure.
There already has been concern over too much patient exposure to radiation, and the US Food and Drug Administration and various trade groups are working together to improve patient safety. Much of the impetus will be to improve safeguards on machines to reduce accidental overexposure, but the Medical Imaging & Technology Alliance, based in Arlington, Va., has noted that manufacturers also are helping hospitals and imaging centers to set maximum radiation dose limits.
Changes in dosing policy have not had an effect on imaging companies thus far this year, but future changes may have a trickle effect on manufacturers’ profits as they change designs and production lines to keep up with regulations.
Expecting a bounce
In general, medical device companies did not fall as far as other manufacturing sectors did during the “Great Recession,” although some argue that no one is out of the woods just yet. For example, according to analyst Angelos Angelou, the recession caused many industries to focus on reducing costs, consolidating facilities and holding back on expansion plans. Medical device manufacturers, he said, are among the rare exceptions that are still actively pursuing sites upon which to build new facilities.
Having spent months tightening their belts, CEOs in a broad range of industries are feeling better about the global economy, and some see specific signs of rising fortunes in the health care industry as a whole. The Chicago-based outplacement consultancy company Challenger, Gray & Christmas noted recently that, of the 119 chief executives who left their jobs in March, 56 were from the health care sector. To Challenger, this indicates a strong but volatile industry.
Another sign of volatility is merger and acquisition (M&A) activity. The Brunswick Group LLC reported that more than three-quarters of respondents in a recent survey expect M&A activity to increase this year across all industries. Health care and technology companies are among those most expected to see a rise in M&A transactions.

Use of lasers in surgeries and other medical procedures is on the rise and expected to continue growing for the next five years. Courtesy of Dilas.
Medical lasers are among the most dynamic segments in the health care field right now, and the long-term outlook for the field is good. The global value of medical lasers is expected to grow from about $2.3 billion in 2009 to $4.8 billion by 2014, according to Global Information Inc., a market research company based in Kawasaki, Japan. The same group noted earlier this year that the recession adversely affected the medical laser market because of a slowdown in elective procedures such as lasik. However, the downturn apparently hasn’t altered some people’s affection for minimally invasive laser-based treatments such as body contouring. With lasers increasingly being adopted into surgical suites and dental practices, medical lasers should soar for years to come.
Also expected to multiply over the next few years are 3-D medical imaging devices, picture archiving and communications systems, and electronic health records systems, which should all benefit from a push toward integrated health data and a drive by patients to take charge of their care. Last year’s federal stimulus bill promotes the use of electronic health records, funding the push with $19 billion. However, the adoption will be a slow-going process as clinics, hospitals and physicians catch up with both the new technologies arriving and the backlog of records.
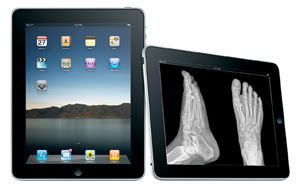
Adoption of the Apple iPad and similar tablet computers and e-readers could revolutionize the ways in which doctors and patients communicate with each other. iPadtm is a trademark of Apple Inc., registered in the US and other countries.
One new piece of technology that may have a surprising effect on the electronic health records rollout is Apple’s iPad, which some foresee as a possible interface that brings patients and health professionals to common ground. Some envision the iPad as a device for storing medical data, for filling out forms and for displaying CT, x-ray and other images in an interactive way that makes it easier for physicians to describe health issues or surgical procedures.
Over the course of the next year, the full effect of new technologies and health care legislation will have a chance to sink in. It looks to be an exciting time.