
New technology permits 3-D visualization of breast cancer
Gary Boas
Mammograms can be unpleasant enough. But then, women are often called
back to the hospital because of uncertainties about the x-ray image. Many times
these turn out to be nothing significant, simply the results of especially dense
breast tissue. Still, the anxiety of having to wait even longer to find out whether
she has cancer is very stressful for the patient. And then there are the added time
and increased costs of the follow-up exams.
Dr. Steven Poplack, co-director of the breast
imaging center at Dartmouth College in Hanover and an associate professor at the
Dartmouth Medical School in Lebanon, both in New Hampshire, is working to improve
the specificity of mammograms for screening and diagnosis of breast cancer. He and
his colleagues already have adopted a digital mammography system that offers greater
image quality and better control over contrast. In fact, they are preparing to replace
their analog mammography system with the digital one. Also, Dartmouth is one of
a handful of medical centers that are currently evaluating a technique known as
digital tomosynthesis for breast imaging in clinical settings.
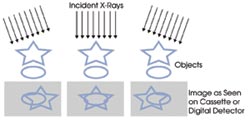
Researchers recently described the potential of a technique known
as digital tomosynthesis for breast cancer screening and detection. In contrast
to conventional mammography, the technique acquires images from different angles,
thus revealing anomalies in the breast that might otherwise remain hidden.
Digital mammography allows radiologists
to manipulate the contrast in images of the breast, providing them with much greater
detail than is possible with analog, film-based systems. This improved contrast
helps to reduce the number of callbacks, making the overall process much less stressful
for women. They may feel more at ease while still in the examination room because
the images can be viewed almost instantaneously on a screen, technicians don’t
have to go elsewhere for image processing, and the patient isn’t left alone
for a seemingly interminable time, wondering what the results might be.
Finally, because it provides better
information, digital mammography involves less exposure to radiation. This is always
an important consideration with x-ray imaging — and with mammography in particular
— because women are asked to have annual examinations beginning at a relatively
early age.
The breast imaging center at Dartmouth
uses a full-field digital mammography system made by Hologic Inc. of Bedford, Mass.
It is built around a selenium-based digital detector that converts x-rays into digital
images in a single step, thus avoiding the resolution degradation and poor quantum
efficiency noted with other, indirect-capture digital detectors. Selenium is a nonmetallic
element that is a photoconductive semiconductor in its amorphous crystalline form.
It offers high x-ray absorption efficiency and intrinsic resolution, as well as
low noise. A high transmission cellular grid technology developed by the company
helps to reduce radiation scatter in the system, contributing to better contrast.
Poplack is working with the company
to develop digital tomosynthesis. Conventional x-ray mammograms are two-dimensional
images, essentially shadows of anomalies in the breast, obtained by transmitting
x-rays from one side of the breast and detecting them on the other. Pathologies
can get lost amid the signals from other, dense tissue, and this tissue can appear
on the image as cause for concern.
Multiple angles
Tomosynthesis overcomes these problems by providing
3-D visualization of lesions in the breast. The technique obtains images from a
variety of x-ray source angles, using even lower dose exposures and the same selenium-based
detector technology as in the digital mammography system. The data is then used
to reconstruct 3-D images of the breast, consisting of a series of thin, 1-mm slices,
much like computer tomography images, which can be viewed either as individual images
or through ciné display. This allows clinicians to zero in on specific regions
of tissue and thus discriminate between pathologies of interest and simple tissue
overlap. The total radiation exposure used to obtain this 3-D information is no
larger than that used with conventional 2-D mammography.
Furthermore, the technique requires
only enough compression to minimize motion artifacts and to pull tissue away from
the chest wall, thus making the scans much more comfortable for patients than conventional
mammograms.
Developing the technique has had its
share of challenges, said Andrew Smith, principal scientist at the company. First,
3-D visualization of the breast requires high-resolution dynamic imaging with several
x-ray frames per second. There are also mechanical issues because the x-ray must
be moved around the breast rapidly and accurately. Finally, storing and processing
approximately a gigabyte of data for each image and manipulating the 3-D image calls
for considerable computational power. Still, Smith noted that these were not insurmountable
problems. “Each had known solutions.”
Perhaps the more daunting task will
be convincing physicians that they should adopt tomosynthesis. Most doctors are,
by nature, conservative, he added, and they don’t like trying new techniques
until they’ve been proven to work better. The company has addressed this challenge
by building a dual system that performs both mammography and tomosynthesis, enabling
doctors to use conventional mammography but also to familiarize themselves with
tomosynthesis over time. As they gain confidence in using the new technology and
come to understand its benefits, they may be more willing to adopt it.
Indeed, in a presentation at the 2005
meeting of the Radiological Society of North America in Chicago, Poplack reported
a study that underscored the potential of the technique. The study looked at 98
women who had been recalled to the hospital because of uncertainties about their
initial mammograms and concluded that screening with tomosynthesis could have avoided
approximately 40 percent of those visits.
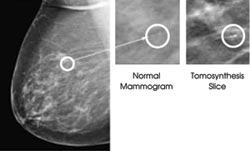
The improved contrast offered by digital tomosynthesis not only could
help to reduce the number of false-positives in breast cancer screening —
the researchers reported that roughly 40 percent of the return visits in a recent
study could have been avoided — but also could identify tumors earlier, thus
contributing to reduced mortality rates.
In addition to reducing the number
of false-positives, screening with the new technique simply might find more cancers
early on, as it allows radiologists to visually peel away the layers of the breast
and find tumors that might otherwise have remained hidden. Hence, it could contribute
to a lower mortality rate.
Poplack and colleagues are preparing
to start clinical trials to demonstrate the efficacy of the technique for FDA approval.
A commercial tomosynthesis system could be available within a year and a half.
Contact: Jim Culley, Special Projects,
Hologic Inc., Bedford, Mass., +1 (781) 999-7583; e-mail: [email protected].
Published: September 2006