
Tracking disease for science and the law
It was a case of what, and then possibly who, dunit. In early 2009,
the Atlanta-based Centers for Disease Control and Prevention (CDC) announced that
it was tracking a salmonella outbreak that had sickened hundreds and killed a handful.
Ultimately the problem was traced back to contaminated peanut butter, which prompted
a massive recall and spawned a series of investigations.
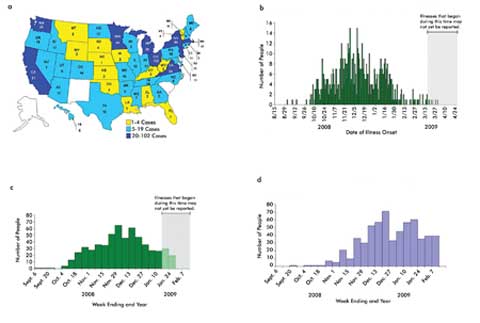 The 2009 salmonella outbreak mapped according to (a) state [as of
April 20 (n = 714)], (b) date of illness onset by day [as of April 20 (n = 696)]
and (c) week [as of Feb. 8 (n = 585)] and (d) date uploaded to the CDC [as of Feb.
8 (n = 600)]. Some illness onset dates indicated in panels (b) and (c) were estimated
from other reported information. Note the widespread nature of the outbreak and
the lag between illness onset and disease reporting. From the CDC report “Investigation
Update: Outbreak of Salmonella Typhimurium Infections, 2008–2009.”
The 2009 salmonella outbreak mapped according to (a) state [as of
April 20 (n = 714)], (b) date of illness onset by day [as of April 20 (n = 696)]
and (c) week [as of Feb. 8 (n = 585)] and (d) date uploaded to the CDC [as of Feb.
8 (n = 600)]. Some illness onset dates indicated in panels (b) and (c) were estimated
from other reported information. Note the widespread nature of the outbreak and
the lag between illness onset and disease reporting. From the CDC report “Investigation
Update: Outbreak of Salmonella Typhimurium Infections, 2008–2009.”
Evidence of the problem first surfaced in October 2008. Reported
cases peaked in December of that year, with more than 50 people a week falling ill.
The cause wasn’t pinpointed until January 2009, four months after the first
cases started appearing.
The length of time it took to identify the source isn’t
surprising, said Pittsburgh-based forensic epidemiologist Steven A. Koehler. “In
cases of food poisoning, it’s not going to show up as if somebody raised a
flag. It’s just going to simmer – a case here, a case there.”
Forensic epidemiologists try to figure out where a particular
disease came from and whether it’s a naturally occurring event or whether
somebody deliberately caused it. They do so by analyzing data derived from microscopy,
gene sequencing, image analysis and other analytical techniques.
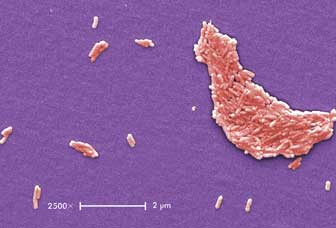
Shown is a colorized scanning electron micrograph of Salmonella typhimurium bacteria,
the type responsible for a multistate outbreak traced by forensic epidemiologists
to peanut butter. Photo credit Janice Haney Carr. Courtesy of Bette Jensen, CDC.
They have to do this in a way that will stand up in court, if
legal action eventually is pursued. A look at the field shows what is being done,
how photonics helps and what technological advances are needed.
“Forensics by definition is the application of science to
law,” explained Koehler, who runs a consulting firm. He has worked with the
CDC as well as the FBI and the Drug Enforcement Administration of Arlington, Va.
He’s also an associate professor of epidemiology at the University of Pittsburgh’s
graduate school of public health.
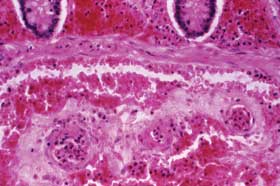
A case of fatal human anthrax due to gastrointestinal infection. This micrograph reveals
a submucosal hemorrhage in the small intestine. Courtesy of Dr. Marshall Fox, CDC.
Forensic epidemiology, then, is the intersection of the science
of epidemiology, which deals with the transmission and control of disease, with
the legal system. That definition carries certain implications. For one thing, the
field is not just about dead people. Nearly all of those sickened by the peanut
butter salmonella outbreak lived. Given that, there can be civil as well as criminal
legal action.
Survival is also the norm in bioterrorism incidents. In the 2001
anthrax attacks, for example, five died, while 17 other infected people lived.

Hand washing is a defense against salmonella bacteria, which are found on turtles and
elsewhere. The disease and some possible bioterrorism agents occur naturally, making
it difficult to determine the origin of an outbreak and whether it was accidental.
Photo credit James Gathany, CDC.
The intersection of science and law also means that some instruction
is involved, as illustrated by the continuing cross training that takes place between
the CDC and FBI and elsewhere (see sidebar). In part, this is because the primary
training for those in the legal system is not in the sciences. Hence, some education
of law enforcement and legal professionals is needed about how epidemiology can
be used in an investigation.
Another reason for the training is that, for many health professionals,
preserving evidence is a secondary concern, at best. The focus is on treating the
patient, not identifying, collecting, cataloging, photographing and storing his
or her belongings. Thus, successful forensic epidemiology involves some education
of nurses, doctors, emergency room personnel, medical examiners and others on the
importance of the chain of custody.
When to collect evidence can be difficult to determine. Arthur
Reingold, a professor of epidemiology at the University of California, Berkeley,
noted that salmonella is a fairly common disease and that outbreaks of it are not
necessarily suspicious. Likewise, anthrax is naturally occurring, although not common.
As a result, an isolated case may or may not warrant preservation of evidence, although
he said that someone who had anthrax and had not traveled outside the US to an anthrax-endemic
area might trigger suspicion and alarm.
But that uncertainty is not the case for all infections, Reingold
said. “If someone were investigating a suspected case of smallpox, it would
be an immediate suspicion that it is a forensic episode, because there is no smallpox
in the world.”
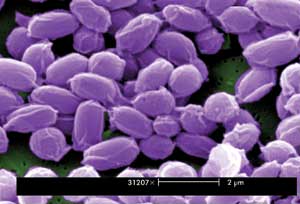
Pictured in this scanning electron micrograph are anthrax spores,
which can lay dormant for years but are potentially a biological terror weapon.
Photo credit Janice Haney Carr. Courtesy of Laura Rose, CDC.
In the aftermath of the events of 2001, concerns about possible
bioterrorism attacks of this nature have had an effect. Forensic epidemiology, at
least that part involving response to potential and actual terror attacks, has attracted
attention and funding, in part because it has become a national security issue.
As a result, three-letter government agencies won’t comment
on it. In the case of the FBI and the CDC, the second refers everything about the
technology behind forensic epidemiology to the first, which refuses to say anything.
However, in the past decade, the field has benefited from advances
in imaging, gene sequencing, image analysis and other technologies. The advent of
digital photography, for example, has made it possible for pathologists to easily
transmit images and data around the country or the world, which enables easier consultation
and more accurate disease determination. Because the findings of pathologists often
form the basis for the data that epidemiologists work with, this innovation helps
in pinpointing disease episodes and their causes.
Gene sequencing also has proved beneficial. In the case of the
salmonella outbreak, for instance, one piece of evidence came from pulsed-field
gel electrophoresis. A pattern – what the CDC termed an unusual DNA fingerprint
– showed up in samples taken from the field and was first noticed by the agency’s
staff in November 2008. Similarities to samples collected later helped convince
agency scientists that what appeared to be two outbreak patterns was actually only
one.
Similar genetic fingerprinting was used in the anthrax attacks.
Also, in a nonforensic, but still epidemiological, case, gene sequencing helped
decipher the H1N1, or swine, flu last year.
Image analysis advances have helped forensic epidemiology in a
number of ways. For one thing, those in the field often do a lot of mapping, looking
at the relationship between cases in time and space. Being better able to present
the data in meaningful ways makes this task easier. It also can help in the other
aspect of the job: the presentation of data to public officials or those in a court
of law.
“Any of those things that are investigated can be plotted
and shown a myriad of ways, by age, by mechanism, by sex, by race. Any way you want
to do it, it can be shown, and that can be helpful. Because, you know, a picture
is worth a thousand words,” Koehler said.
As for future capabilities, he’d like to get more detailed
data, noting that the CDC currently gets its initial epidemiological information
from what is on a death certificate. At one time done on paper, death certificates
have gone digital, as has everything else. Such certificates, however, still don’t
contain all of the information generated by the medical examiner’s office,
doctors or police.
Autopsy photos, for instance, aren’t there. Neither is a
complete medical history or evidence such as crime scene pictures. The ongoing switch
to digital data and electronic medical records makes it possible to include all
of this information, which would be a boon to epidemiologists and others.
But not everything can simply be swept up into some new database.
Whereas information such as a death certificate is currently a matter of public
record, data such as an autopsy photo is not. Some information – death from
a communicable disease, for instance – falls into a gray area. These have
to be reported to the CDC and the family but not to the neighborhood of the deceased.
Settling such issues may take some time and involve new privacy
protections. Koehler noted that the pace of technological advance in the legal system
can sometimes be much slower than that outside of it.
An example can be seen in crime scene photography. Years ago,
color images were not allowed by some courts, on the theory that the images would
inflame passions. Today, color is widely permitted.
However, the emergence of digital imaging has raised another issue.
It’s one that pertains to all the digital data used in forensic epidemiology.
As Koehler said in explaining this concern, “Was the image
tampered with? It’s hard to tamper with a 35-mm negative. You can do a lot
with Photoshop.”
Training to detect crime and bioterrorism
While there may have been only a handful of bioterrorist incidents
over the past few decades, the possibility of more threats has caused concern. That’s
one reason why the CDC and the FBI created the Criminal and Epidemiological Investigation
Handbook in 2002. The CDC also developed a course designed to enhance the joint
effectiveness of law enforcement and public health staff in the event of the use
of biological weapons.
Within three years of the Sept. 11, 2001, and anthrax attacks,
this forensic epidemiology training had been given to more than 8500 public health,
law enforcement and first responder professionals in 42 states and territories.
That instruction is ongoing. The University of North Carolina at Chapel Hill, for
example, developed a free online version for awareness level training.
Forensic epidemiology instruction is not confined to specialized
courses, however. At the University of North Carolina, research assistant professor
of epidemiology Pia MacDonald covers the intersection of public health and law enforcement.
“I teach a two-week module about forensic epidemiology as
part of another semester-long course,” she said.
Published: September 2010