Photonics is making waves among the dental specialists known as endodontists – think root canals – finding success in the critical canal disinfection process and spawning a new opportunity for laser Raman spectroscopy.
The goal of endodontic treatment is to save a damaged or infected tooth through a systematic process of shaping, cleansing and sealing designed to kill bacteria in the canal and prevent its return. The process removes diseased dental pulp from inside the tooth and disinfects the root canals so no new bacteria can grow after the crown is replaced.
Conventional endodontic treatment is carried out through the use of hand and rotary tools, including files and high-speed drills, and sometimes requires two or more appointments for complete success. Some patients require painkillers to make the procedure more tolerable. Research is ongoing to improve disinfection, thereby increasing success and reducing the number of visits required to complete the treatment. Reducing patient pain and discomfort also is a goal.
Yikes! Sounds about as much fun as, well, having a root canal. But the use of lasers in endodontics has been studied since the early 1970s, and a couple of promising applications have emerged to address these challenges.
Enrico DiVito, DDS, a dentist for 33 years, recalls the early days of lasers in dentistry as less than successful. Big and bulky lasers used for thermal disinfection often damaged the treated teeth.
“Early lasers fried or burned the teeth while killing the bugs,” he said. Eventually, it was learned that various lasers have characteristics that work best on certain tissue types. For endodontics, lasers are used in both hard and soft tissue applications.
The FDA has approved lasers for use in all steps of endodontic treatment, from accessing the canal to cleaning, shaping, filling and sealing. Ever since the diode laser was approved for pulp tissue removal in 2000 and the Er,Cr:YSGG laser for complete endodontic treatment in 2002, research has focused on answering the question of whether the laser can effectively replace hand and rotary instruments. A number of laser types have been used in subsequent studies, and some are currently deployed in clinical settings, where much of the focus for their use is on killing bacteria in the canal.
In 2009, the American Dental Association’s Council on Scientific Affairs issued its Statement on Lasers in Dentistry, acknowledging an expanding landscape of research and applications. At that time, lasers were cleared for the endodontic applications pulpotomy, blood flow measurements and apicoectomy (root tip removal) as well as for illumination of the endodontic orifice and for softening gutta percha. Although the statement acknowledged lasers as a useful cleansing adjunct, it made it clear that there was no evidence that lasers provided a “higher clinical success rate than conventional instrumentation,” the holy grail of alternative tools and processes.
Today, researchers are investigating a number of incremental improvements to laser disinfection and some that may be considered more paradigm shifting. In root canal treatment, canal disinfection is a critical step that is classically achieved by introducing a chemical solution, frequently but not exclusively NaOCl, into the prepared canal and leaving it there for a period of time in a step called irrigation. Sometimes the irrigant is activated in the canal by any of a variety of agitation techniques, including by an ultrasonic device. It is here that lasers may ultimately be most useful in endodontics.
Light-activated disinfection
Through his own investigation, DiVito discovered that an erbium-pulsed laser has a dramatic effect in fluid. He found that placing a small tapered and stripped fiber tip into water and turning the laser on created a profound shock wave that travels throughout the canal system three-dimensionally, stirring up tissue, debris and bacteria that can then be removed from the canal. Medical Dental Advanced Technologies Group LLC, where DiVito is a partner, turned that discovery into a trademarked and patented endodontic cleaning and debridement technique known as PIPS, for photon-induced photoacoustic streaming.

Laser and photon-induced photoacoustic streaming (PIPS) being tested on an extracted human tooth. Images courtesy of Enrico DiVito, DDS.
DiVito recently led a study to compare the efficacy of conventional syringe irrigation with both irrigation with a solution that is ultrasonically activated and solution that is activated by laser light using PIPS. The team was particularly interested in the ability of the laser-activated irrigation to remove not only smear layer but even bacterial biofilm from root canal walls.
In the study, 6 percent NaOCl was deposited into one group of prepared teeth where, after 30 seconds, it was activated for another 30 seconds by a 2940-nm Fidelis Er:YAG laser manufactured by Fotona of Ljubljana, Slovenia, at 10 Hz and 50 mJ and fitted with a 21-mm-long, 400-µm tapered and stripped endodontic fiber, placed into the coronal reservoir only. Similar groups of prepared teeth were irrigated either conventionally or ultrasonically for the same amount of time.
 The combined in situ/in vitro study showed that, although activated disinfection failed to completely remove bacteria from the apical root canal and dentinal tubules, two challenging areas in any disinfection, laser-activated irrigation resulted in a greater number of negative bacterial samples and did a better job on removing bacteria and biofilm than ultrasonic activation, warranting further investigation.
The combined in situ/in vitro study showed that, although activated disinfection failed to completely remove bacteria from the apical root canal and dentinal tubules, two challenging areas in any disinfection, laser-activated irrigation resulted in a greater number of negative bacterial samples and did a better job on removing bacteria and biofilm than ultrasonic activation, warranting further investigation.
The study, “Disinfection of Root Canals with Photon-initiated Photoacoustic Streaming,” by O.A. Peters et al, was reported in July 2011 in the Journal of Endodontics (doi:10.1016/j.joen.2011.03.016).
PIPS is not without its challenges, however, DiVito said. “As with any new methodology, training is of utmost importance.” On the plus side, laser PIPS may reduce chair time needed to treat the patient to one visit, he said, adding that his results show that PIPS reduces postoperative pain without jeopardizing either the quality of care or the result.
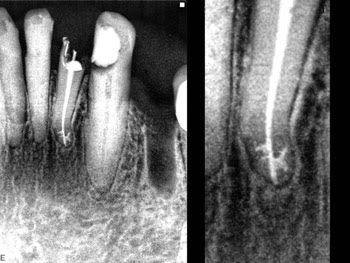
An example of effective cleaning of the very intricate and complicated root anatomy after use of photon-induced photoacoustic streamimg (PIPS).
“When we do our procedures with laser, patients heal faster; this elegant delivery of energy is a win/win in all directions,” he said. Although it is making some gains among endodontists, the laser is still not a prevalent technology, said Dr. Ove A. Peters, a widely published researcher as well as a professor and director of endodontic research at the University of the Pacific, Arthur A. Dugoni School of Dentistry in San Francisco, who participated with DiVito in the study mentioned above.
Hard tissue preparation by lasers is not mainstream in endodontics but has some proponents, he noted. He also said that some experimental data suggest that photodynamic therapy may be useful.
Research into photodynamic therapy in endodontic treatment appears in the literature beginning around 2006. It involves the use of photosensitizer material such as methylene blue and light to render micro-organisms inactive. In early 2010, Tom C. Pagonis, DDS, MS, an assistant clinical professor of restorative dentistry and biomaterials sciences at Harvard School of Dental Medicine in Boston, and his team published the results of a study that loaded the methylene blue onto nanoparticles of polylactic-co-glycolic acid as a delivery system to be used with 665-nm red light in the root canal. Findings suggest that it may hold promise when used with other forms of endodontic disinfection.
Laser Raman spectroscopy takes root
Ridding the root canal of bacteria is, as has been said, the primary goal of endodontic treatment. Bacteria in numbers beyond an acceptable level left behind after a root canal treatment can result in recurrence of the infection and may require retreatment.
Scott C. Howell, DDS, DMSc, a dentist and microbiologist in Laguna Niguel, Calif., performs root canals in clinical practice and is interested in rapid identification of microorganisms so patients can be properly treated without delay.
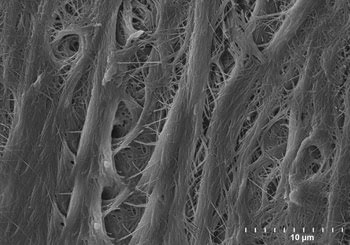
Dentin is very clean and undisturbed after an endodontist uses a laser with photon-induced photoacoustic streaming (PIPS).
“In certain instances, you can save lives by quickly identifying the infectious agent involved,” Howell said. He speaks from experience. He knows someone who almost died from a bacterial infection because of a delay in determining the offending agent and initiating the most appropriate treatment for it.
The idea of using laser Raman spectroscopy (LRS) to identify bacteria came from reading cancer studies, which used similar techniques to identify human cancer cells. Although he readily admits that his recent Raman paper is probably more medically useful than endodontically useful, he is a dental specialist with access to The Forsyth Institute’s dental microbiology labs, so he tested the portable Raman system on orally important and, in some cases, medically important bacteria. He believes the concept explored in this paper could be especially useful in areas of the world where modern microbiology labs are not readily available.
As a first step toward the goal of rapid, chair-side bacteria identification, he and his team designed an experiment to determine whether LRS can “discern uniqueness among 10 different species of bacteria contained within a medium in unprocessed and processed samples,” according to the study.

A laser with a tapered and stripped endodontic fiber PIPS tip.
The Raman system assembled for the study comprised a 784-nm, 300-mW external temperature-stabilized diode laser, the BRM-785, made by B&W Tek Inc. of Newark, Del., as the light source; a Holospec f/2.2 transmissive imaging spectrograph from Kaiser Optical Systems of Ann Arbor, Mich.; and a near-infrared optimized back-illuminated, deep-depletion, thermoelectric Peltier-cooled CCD array (400 x 1340 pixels at 20 x 20 mm per pixel), the Spec LS785 400BR, made by Princeton Instruments of Trenton, N.J., to measure the intensity of the dispersed light. A specially designed probe and two stages of optical filtering completed the system.
Howell’s team demonstrated that the system could generate unique spectral signatures for each bacterial species put to the test, leading to the conclusion that “chair-side LRS is a promising technique that differentiates among oral bacterial species with a high degree of specificity.”
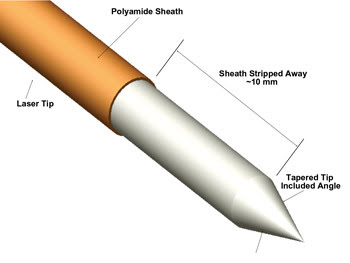
A schematic of a PIPS tip showing the stripped and tapered tip.
A proof-of-concept study, “Laser Raman Spectroscopy as a Potential Chair-side Microbiological Diagnostic Device,” by Howell; Anne D. Haffajee, BDS, DDPH; Pagonis; and Kevin A. Guze, DMD, DMSc, was reported in July 2011 in the Journal of Endodontics (doi:10.1016/j.joen.2011.03.027).
Future studies will focus on developing a library of Raman spectral signatures for a variety of infectious agents, with an eye toward minimizing harm to the patient during signal acquisition.
Although his system worked for his proof-of-principle study, it would have to undergo major changes to become the portable device he imagines for wide acceptance and use. The current system is mobile, but not iPad mobile, weighing 50 lbs and kept on a cart.
“It would have to be lighter, rugged and NOT an energy hog. It would be especially useful if it ran off battery power,” Howell said. His study showed this Raman system did not require sample preparation or a complicated room setup. His ultimate vision is for a point-and-shoot LRS. “Almost like the tricorders on Star Trek. Ultimately, that’s what this should translate to.
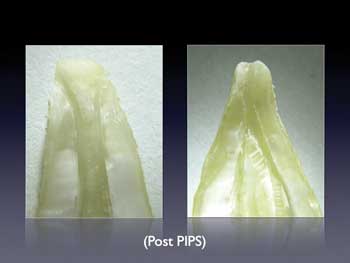
The laser PIPS process, which uses a specially designed fiber tip to activate the irrigant, can result in very clean root canals.
“I think the system has huge potential. However, the technology is not there yet, and it is very expensive. If I had to go out on a limb with a time line, I’d say a workable unit could be ready in five years if significant resources were dedicated to its development.”
High cost limits acceptance
Tests may show that laser-driven disinfection is at least as effective as conventional and ultrasonic methods, but high cost may be the last, most difficult barrier to wider use of lasers in endodontic treatment.
“Money is the number one challenge to widespread use of laser PIPS,” DiVito said. He does see that barrier breaking down, however, with the price of a PIPS unit now down to around $30,000.
Howell said he is not using laser in his practice because of the cost. “Even the Raman machine was $75K.” He does believe that, as technologies get better, the price will come down.