
The Age of the Tricorder
The medical device of the future is already here.
The Star Trek television series and movies have proved remarkably prescient in anticipating future technologies – from flip phones to iPads – decades before they appeared in everyday life. Now, nearly half a century after the debut of the original series, the science fiction classic featuring Captain Kirk and the alien Mr. Spock, we are beginning to see modern-day equivalents of another iconic Star Trek device: the tricorder.
In the series, tricorders are handheld medical instruments used to detect, diagnose and treat any number of injuries or maladies, either terrestrial or alien. The design has evolved over the decades, but in all cases the device is portable, requires no external power source and provides some sort of sensing capability.
This description also can be applied to a new generation of sensing and imaging devices in our own time. Recent advances enabling miniaturization of the technologies, the advent of smartphones with cameras and data-transmission capabilities, and other factors have led to the development of a host of instruments that might be described as tricorders, or at least as tricorder-like. And there’s undoubtedly more to come.
Early this year, the X PRIZE and Qualcomm foundations announced the launch of the $10 million Qualcomm Tricorder X PRIZE, a global competition in which teams will leverage innovative technologies such as wireless sensing to develop a mobile platform that can make medical diagnoses independently of a physician or health care provider. The top prize will go to the team whose platform most accurately diagnoses a set of 15 diseases involving 30 consumers in three days, while also providing a compelling consumer experience.
There’s no telling what the winning design will look like, or what technology it will employ – the only constraint is that the system and its components together can’t weigh more than 5 lb – but many assume it will involve a smartphone running custom-developed apps, in no small part because smartphones already carry sophisticated cameras and displays as well as other technology essential to the sort of home health monitoring envisioned by the sponsors of the competition.
Importantly, from a technology standpoint, such a platform is possible today. A variety of research groups and companies have already taken advantage of advances in imaging technology to turn smartphones into microscopes and sensor systems. One example: Philips offers an iPhone and iPad app called Vital Signs Camera, which can measure heart rate from a distance, extrapolating heartbeats from a slight flushing of the skin.
Where does the Qualcomm Tricorder X PRIZE fit in, then? The competition is about technology development, said Bruce Tromberg, director of the Beckman Laser Institute and Medical Clinic at the University of California, Irvine, but it is just as much about determining what information people need to make a diagnosis, to know when to see a doctor, when to take medicine, and so on, and determining how best to obtain and use that information.
As the health care landscape continues to change, he said, activities like screening and follow-up – monitoring, generally – will move into the home, into the hands of the patient.
One possible scenario: Sensors on a smartphone or some other device will monitor a patient’s physiological parameters and send the data to a server for analysis. The results will be considered in the context of the patient’s overall health (his or her entire medical history will also be stored there), and if any further action is needed – “call the doctor,” “pick up a prescription” – an email or text will be sent.
The tricorder competition will help us envision what all this will look like.
Home testing is only one potential use for tricorder-like devices, however. Such instruments could help to advance a range of additional applications, both within and beyond traditional clinical settings.
Point of care
In the clinic, Tromberg and colleagues are developing devices for physicians that can impact patient care and even change clinical outcomes: for example, a handheld laser scanner for use in detection, diagnosis and treatment of breast cancer. By measuring parameters such as hemoglobin concentrations and fat and water content, the device can help distinguish between potentially malignant and benign tumors. It can also be used to evaluate the effectiveness of chemotherapy – at bedside and during the course of treatment – allowing the oncologist to adjust the therapy based on how the patient responds.
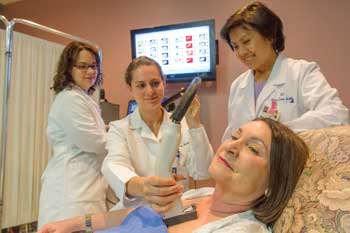
Researchers at the Beckman Laser Institute at the University of California, Irvine, have developed a handheld laser scanner to distinguish between potentially malignant and benign tumors in the breast. The device uses diffuse optical spectroscopy imaging and a new analysis method called self-referencing differential spectroscopy analysis. A recent Cancer Research study demonstrated the potential benefit of this method. Courtesy of Paul Kennedy.
Tricorder-like devices could help to advance care in other settings as well, including any number of sites where advanced diagnostic devices wouldn’t normally be found.
Chris Myatt is founder and CEO of MBio Diagnostics, which develops optics-based solutions for disease diagnosis and research. In an article in the February 2011 issue of BioPhotonics (“Not Your Father’s Microscope,” pp. 21-23), he said, “We look at point-of-care, home testing and world health together as resource-limited settings, where users are not formally trained medical technicians and the ‘lab’ facilities are not sophisticated. This is true of a clinic in Mozambique, a mobile STD van in San Diego, or in a home in New York.”
“Point of care” refers to testing or monitoring performed at or near the site of care, although it is more commonly used today to describe clinical services provided in nontraditional settings. For example, especially with the shifting health care landscape in the US, we will see an increasing demand for long-term monitoring of chronic diseases – including cardiovascular and autoimmune – in pharmacies and other retail outlets (both CVS and Wal-Mart have explored the possibility of keeping diagnostic kiosks in their stores) as well as in community clinics and outreach centers.

MBio Diagnostics has developed a multiplexed fluorescence immunoassay system for rapid diagnosis of complex infectious diseases like HIV and hepatitis. Among the applications the company is exploring: antenatal screening for HIV/syphilis in Kenya. Courtesy of MBio Diagnostics.
Also consider point-of-care HIV testing. Testing is already done in nontraditional settings including the mobile STD vans in San Diego and elsewhere and, with a new program in Washington, testing sites in grocery stores and high schools and even at the Department of Motor Vehicles. And demand for this point-of-care application continues to increase.
Optics-based technologies are well suited to meet this demand. The technologies may not look exactly like the tricorders in Star Trek – devices roughly the size of an electric razor that you operate by waving them around in the air somewhere near the patient – but they meet all the criteria that matter: portable, rugged and reliable.
Since April of last year, the Antiviral Research Center at the University of California, San Diego, has been evaluating the performance of an MBio system designed to deliver absolute CD4 counts at the point of care in minutes; CD4 count is essential to monitoring disease progression in HIV patients. The system – a fluorescence imaging cytometer with single-use disposable cartridges – offers a rapid read time of 3.5 min and a simple design, with passive fluid handling (no pumps or valves) and minimal biohazard (all waste stays onboard). The system weighs about 2 kg, with dimensions of 12 x 8 x 20 cm.
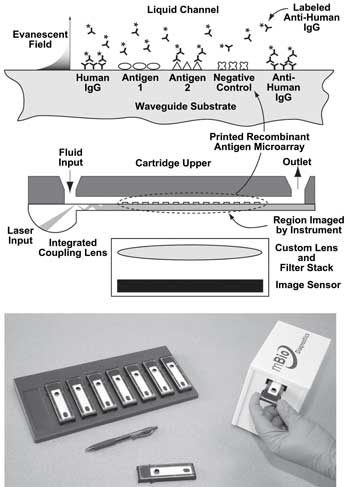
The MBio Diagnostics system combines single-use disposable array cartridges with a simple reader instrument – a USB peripheral device that connects to and draws power from a laptop computer – to provide simultaneous measurement of multiple analytes from a single sample. Illumination and imaging of fluorescence immunoassays is achieved using a multimode planar waveguide technology developed by the company. Courtesy of the Journal of Clinical Microbiology.
Preliminary findings from the study, presented at the 2012 Conference on Retroviruses and Opportunistic Infections held in Seattle in March, showed that the system had “minimal bias” relative to the gold standard, flow cytometry – thus underscoring the potential of the system for point-of-care applications.
Imaging in the developing world
Tricorder-like devices – particularly optics-based ones – can also contribute to a host of global health applications. There is little access in developing nations to the sophisticated lab tests and the training needed to run them that can be commonplace in the developed world.
Health care workers use a variety of inexpensive, portable tests to meet the many global health demands they face, but these can have limited efficacy. In recent years, researchers and medical device companies have shown that optics-based technologies can bridge this gap.
Take, for example, rapid diagnostic tests (RDTs) – assays designed to detect target analytes in blood or fluid samples. Using RDTs, and with only minimal training, health care workers have been able to detect a range of diseases – including HIV, malaria, tuberculosis and syphilis – leading to better management of disease and more efficient surveillance of outbreaks.
Conventional RDTs have their limitations, though. Because they are read manually, there is potential for error, especially as the workers often administer a variety of different tests at the same time. Cell-phone-based, tricorder-like devices could help to eliminate this potential for error by offering automated readings of the diagnostic tests.
At the annual conference of the American Association for Clinical Chemistry held in Los Angeles in July, Holomic LLC – a company launched in 2011 to commercialize the biophotonic technologies invented in Aydogan Ozcan’s lab at UCLA – introduced its cell-phone-based rapid diagnostic test reader, the HRDT-1.
Weighing only about 65 g, the device mechanically attaches to the existing camera unit of a cell phone. An app on the phone digitally processes captured images – within 0.2 s per image – then provides a reading of the diagnosis, and finally sends the image and accompanying data to a central server.

Cell phone-based technologies such as this recently announced device developed by researchers at UCLA can help to address a range of global health needs. Courtesy of Ozcan Research Group at UCLA.
Uploading images to the server offers a means to store them; the color changes in RDTs don’t last more than a few hours in the field. But it has other advantages too. “The cloud angle and the Google Maps-based interface could especially help over the long run to study the data that accumulates,” Ozcan said. “In the shorter term, it can also help manage epidemics or get prepared for them.”
HIV/AIDs is, of course, another health concern in the developing world, especially in sub-Saharan Africa. In 2009, an estimated 33.3 million people worldwide were living with AIDS, according to the UNAIDS Report on the Global AIDS Epidemic 2010. Of those, an estimated 22.5 million were in sub-Saharan Africa. The number of new infections is dropping, but there is still a considerable need for screening and monitoring of the disease.
MBio is also seeking to tackle HIV in Africa and other parts of the developing world. In addition to the CD4 test for staging of the disease and ongoing monitoring of therapy, the company is developing tests for co-infections, and panels of tests for applications such as antenatal screening. “We have an HIV/syphilis combination test currently in a study in rural Kenya, testing pregnant moms for these diseases where intervention can prevent the transmission to the child,” Myatt said.
The latter application, in particular, has been in the spotlight recently. In July, in a keynote address at the biennial conference of the International AIDS Society, Secretary of State Hillary Clinton called for elimination of mother-to-child transmission of HIV, worldwide, by 2015.
Currently, HIV/syphilis screening in resource-limited areas uses an HIV rapid test and the RPR (rapid plasma reagin) syphilis test. The latter, though, requires a skilled operator with laboratory facilities and a “cold chain” for the reagents (where reagents are shipped and stored cold throughout the supply chain), and it generates many false positives, particularly in pregnant women. “While inexpensive,” Myatt said, “the RPR test’s complications limit its use.”
Innovation and entrepreneurship
Few would argue the importance of developing optics-based and other medical devices for global health applications, but sustainability of the model can still prove challenging. “At the end of the day there has to be a market,” said Utkan Demirci, director of the Bio-Acoustic-MEMS in Medicine (BAMM) Laboratory at Brigham and Women’s Hospital in Boston, and an assistant professor there as well as at Harvard Medical School and Harvard-MIT Health Sciences and Technology. The lab develops microfluidics for CD4 counts and viral load for HIV in resource-limited and other settings. These technologies also have been adapted for isolating and detecting bacterial pathogens in produce (e.g., milk, spinach), and for primary care blood sensing applications; they have potential military applications as well.
Additionally, as a part of his educational efforts in the field, Demirci developed and taught a course at Harvard-MIT Health and Sciences Technology titled “Designing and Sustaining Technology Innovation for Global Health Practice.” The course – which has been offered several times in the past five years – is based on the premise that innovation in this area requires leaders to think and act like entrepreneurs. There’s been considerable interest in the course, Demirci said. “It’s amazing how people are motivated to help.”
Published: September 2012