Economy and aging population affect adoption and success of laser-based techniques.
Lasers are helping to advance a range of ophthalmic applications. At the same time, ophthalmology is proving an important market for manufacturers of lasers and laser-based systems.
This is in no small part because of its unique blend of insurance-reimbursed (photocoagulation) and elective procedures (lasik and laser cataract surgery), said Matthias Schulze, Coherent Inc.’s director of marketing in the life sciences. Demand for elective procedures will ebb and flow with fluctuations in the economy, as it is strongly dependent on consumer confidence and how people feel about spending money from their own pocket. But changes here will be counterbalanced by demand for other, insurance-reimbursed procedures.
To be sure, we’re seeing an ever-greater need for photocoagulation for treatment of age-related macular degeneration (AMD). As the name implies, this condition predominantly affects older populations – either atrophy of an epithelial layer below the retina or abnormal blood vessel growth can lead to loss of vision. AMD is a major cause of visual impairment and blindness in adults over 50. And because of the aging population, more people are suffering from it today than have in many years (see sidebar).
The increasing prevalence of age-related macular degeneration has spurred interest in developing ways to treat it. Drugs and photodynamic therapy are both widely used options. Also, in some cases of wet AMD – that is, AMD caused by retinal bleeding – doctors will use laser photocoagulation, stemming the bleeding by finely cauterizing the vessels.
One risk of laser photocoagulation is the possibility of retinal scarring – a complication of burning the blood vessels in the eye – possibly causing blind spots in the patient’s visual field. In part to address this risk, Coherent introduced the OPSL 577-3 solid-state laser, which delivers 3 W of yellow output at 577 nm. Because it is exactly matched to the main absorption peak of oxygenated hemoglobin, it provides a higher degree of tissue selectivity than other wavelengths and, thus, less risk of scarring.
On the elective side, use of femtosecond lasers is helping to advance lasik and laser cataract surgery, offering considerable advantages over conventional approaches to these procedures.
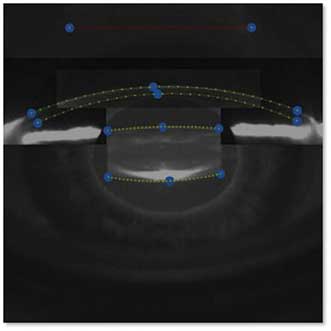
In the past several years, ophthalmologists have been using femtosecond lasers to perform cataract procedures. Here, Scheimpflug images of the anterior segment of the eye allow detection of the critical surfaces (anterior and posterior cornea, anterior and posterior lens capsule). Images courtesy of LensAR Inc.
Using femtosecond lasers in cataract surgery helps to automate procedures so they are more standardized, more reproducible and more predictable – and ultimately safer and more effective – said Dr. Mark Packer, clinical associate professor at Oregon Health & Sciences University and president of Mark Packer MD Consulting Inc.
“It’s like going from a single-artisan approach to making a pair of shoes to all of a sudden having a shoemaking factory,” Packer said. A single artisan can turn out a great pair of shoes, but it will take a while, there will always be variability in the quality of the shoes, and so on. With the femtosecond laser, he continued, “a lot of people can have a really good pair of shoes.” In other words, the laser provides a degree of precision that isn’t guaranteed otherwise – and it also ensures consistent precision from one procedure to the next.
The introduction of femtosecond lasers has enabled automation of several “very critical parts” of the cataract procedure. First: the incisions, both the original incision through which instruments are passed and the “corneal relaxing” incision that serves to correct the astigmatism. Next: the capsulotomy, the opening of the anterior surface of the lens capsule. This is the most technically challenging step in cataract surgery, the one that surgeons spend the most time perfecting during their training. It’s also the most prone to error and complications.
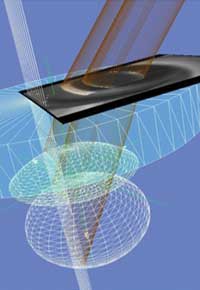
A computer-generated image of the anterior segment of the eye translates imaging into guidance for laser treatment.
Finally, surgeons can use the femtosecond laser for phacofragmentation, the process by which the cataract is broken up. This is important because the process is currently achieved using ultrasound: When applied inside the eye, ultrasound can release a fair amount of energy, causing “subtle but real damage” to the tissues of the eye – possibly including damage to the corneal endothelial cells, which do not regenerate.
‘Laser surgery is better’
The first femtosecond lasers became available for cataract surgery in 2009, but the technique is already attracting considerable interest from patients.
“There’s a perception that laser surgery is better,” Packer said. “And, in fact, we have data that shows it is better – in terms of accuracy and in terms of how well patients see afterward.”
At the 2011 meeting of the American Academy of Ophthalmology, for example, he presented a study that assessed the safety of laser cataract surgery in terms of loss of corneal endothelial cells, as measured after cataract surgery. The study showed no loss of endothelial cells in 225 eyes in which laser lens fragmentation was used, as compared with a 1 to 7 percent cell loss in 63 eyes that received standard treatment. Packer led the research group that conducted this study.
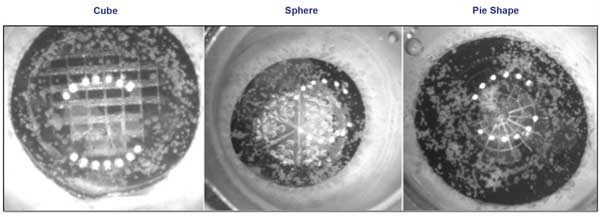
Various femtosecond laser patterns are possible to fragment the lens nucleus in preparation for its aspiration by a fluid pump system.
“It’s not ‘completely knock your socks off’ improvement,” he said. “But it is significant. And it’s going to get better.”
Laser cataract surgery will become standard within the next five to 10 years, he believes. This is a relatively short time to achieve widespread adoption of a technique. Ultrasound imaging, for example, didn’t move into the mainstream of medical practice until the 1980s, some 25 or 30 years after it was first demonstrated.
Laser-based cataract surgery is indeed growing at “a substantial rate,” said Coherent’s Schulze – two to three times the typical growth rates in the medical field. And this is with the relatively weighty price tag (upward of $400,000) attached to the femtosecond laser systems used. If companies could find a way to cut the price in half, he said, they could speed up adoption considerably.
Packer offers a vision of how this might happen. “The current cost of the technology represents the highest hurdle to adoption,” he said, “but we have yet to see any real impact from competition.” Only one of the three major players in ophthalmology (Novartis Alcon) has a system that is fully approved, he added. Bausch & Lomb recently introduced its product, but it doesn’t yet have the full suite of necessary approvals (incisions, capsulotomy and phacofragmentation). Abbott Medical Optics’ laser is approved for incisions only.
“Once all of the ‘big three’ are fully engaged in the game, I believe we will start to see some competitive pricing,” he said, “which will make the technology more affordable.”
The impact of the aging population
The rapidly aging population is leading to increased incidence of cataracts and, therefore, to increased need for cataract surgery. In the US, the number of people over 60 increased by more than 20 percent in the most recent decade for which numbers are available: from roughly 46 million in 2000 to roughly 57 million in 2010, according to a Department of Health & Human Services report. The number is expected to reach nearly 76 million by 2020.
The incidence of cataracts in the US is also on the rise. It has increased 19 percent since 2000, according to a 2012 Prevent Blindness America report, Vision Problems in the US. The report also notes that more than half of all Americans will develop cataracts by age 80, leading to considerable demand for procedures to treat the cataracts.
Will insurance pay for laser cataract surgery?
Not right now. And it could be years before it will. This is because the Centers for Medicare and Medicaid Services, which typically set insurance standards, do not pay differently for the same outcome – i.e., a successful procedure.
“Payment is about the work done, not how the work is done or the technology needed to do it, assuming each produces a quality result,” said Dr. Michael X. Repka, the American Academy of Ophthalmology’s medical director for governmental affairs. If a half-cent needle can achieve the same result as a laser that costs $3000 to use, “the Medicare payment will be based lower.”
This could change if care shifts to the femtosecond laser, he said, but that will take time. Currently, only a small percentage of the 3.5 million cataract procedures performed every year uses a femtosecond laser. The technique will need to be much more prevalent before it is considered the standard.