The technique could advance diagnosis and management of this growing public health issue.
Chronic wounds might not seem a major public health concern – they don’t often make the evening news – but the burden of treating them is significant and growing rapidly.
Often masked as a comorbid condition, chronic wounds affect a surprising number of people: 6.5 million patients in the US alone. And because of the aging population and the increase in the incidence of diabetes and obesity – both of which are associated with such wounds – the prevalence and the cost are on the rise.
Currently, assessment of chronic wounds depends on visual inspection and biopsy of samples from a wound’s surface. But this approach can be time-consuming and expensive, and it can even delay healing or cause new wounds.
For this reason, researchers are exploring the potential of hyperspectral imaging, or HSI. Given its strengths, they say, the technique could significantly advance diagnosis and management of chronic wounds, and thus help to address this growing need in the public health arena.
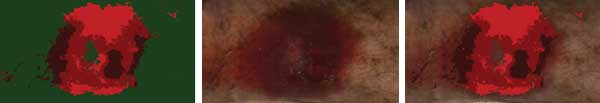
Researchers are developing hyperspectral imaging methods to quantitatively assess wound tissue composition for the detection and management of chronic wounds. Shown here are unsupervised statistical image classification, distinguishing between wound and ‘normal’ skin (top), an RGB representation of the hyperspectral data (center), and wound classes superimposed on the RGB image (bottom). Images courtesy of Martin Denstedt, Norwegian University of Science and Technology.
Hyperspectral imaging has its origins in remote sensing applications – NASA’s Jet Propulsion Lab spearheaded the initial hardware development beginning in 1983 – but in more recent years has moved into the life sciences, where it could serve a range of applications (see sidebar).
Using the technique, researchers can acquire sets of images from across the electromagnetic spectrum, producing an “image cube” where each slice represents a different wavelength. By combining select wavelengths, they can reconstruct images showing the tissue properties of interest.
The full spectrum provided by HSI helps researchers to understand the biological processes in question and to “make sure you don’t overlook anything,” said Martin Denstedt, a graduate student at the Norwegian University of Science and Technology. Working with Lise L. Randeberg, Denstedt is investigating the use of HSI as a diagnostic tool for chronic skin ulcers and other applications.
“As compared to other types of imaging using only a few wavelength bands,” he said, “a ‘full’ spectrum allows for better signal processing – noise filtering in the spectral dimension, component analysis, etc. – and statistical classification of images.” At the same time, it provides information in different regions that allows researchers to establish, for example, hemoglobin oxygenation at different depths, maps of water content, melanin and lipids, and so on – “all available from the same data set.”
Using this information, HSI can aid in quantitative assessment of wound tissue composition and thus contribute to the
detection, staging and treatment of chronic wounds.
There’s still work to be done, though, before the technique is ready for clinical use. While studies have demonstrated the potential of HSI for detection of chronic wounds and other such applications, these were done using bulky and expensive research tools, said Murali Jayapala, a senior researcher in integrated imaging at Imec, a nanoelectronics research center in Heverlee, Belgium. Moving the technique into the clinic, he said, will require access to compact, low-cost HSI cameras.
To this end, Jayapala and colleagues developed “micro-HSI” technology that can be incorporated into medical devices. Conventional hyperspectral camera systems typically use discrete optical components such as diffraction gratings/prisms and image sensors, making the systems generally bulkier. To address the size issue, the researchers monolithically integrated many of the optical components directly on top of the image sensor – and also replaced the diffraction grating with a Fabry-Perot staircaselike filter, which helps to reduce the overall size. “In our current prototypes, the height of these filters, on top of the image sensors, is less than 1 micrometer,” Jayapala said. Integrating the components in this way also contributed to considerably lower costs.

Imec researchers showed a prototype of the ‘snapshot’ version of their micro-HSI technology at Photonics West 2013. This technology can perform real-time classification at video rates (approximately 30 hyperspectral cubes per second). The full readout of hyperspectral data can be much higher: approximately 340 hypercubes per second (or limited by the camera interface). Imec has also built an evaluation system (shown here) that allows potential partners or customers to try out the technology for their specific applications. Courtesy of Imec.
Other groups also are working to develop HSI for clinical use.
Denstedt gives several examples of the hurdles to be addressed before the technology is ready for such applications: automatic focusing, mounting, data-processing speed, quality of illumination, general workability and more.
For its camera – a push-broom-scanning hyperspectral instrument, a VNIR 1600 made by HySpex of Oslo, Norway – the group has developed an automatic system for initial focusing and focus tracking, enabling collection of high-quality data from live patients. The team has also constructed a bedside scanner for use in the clinic. The latter is “quite flexible,” Denstedt said, letting the researchers scan at arbitrary angles.
The researchers have a system in the prototype and testing stage in the clinic, and are currently working on improving their diagnostics algorithms and collecting additional clinical data.
The Imec investigators have developed two prototypes of their micro-HSI technology – a line-scan version, presented at Photonics West 2012, and a snapshot version, presented at Photonics West 2013 – and are looking ahead to clinical validation of the technology and ultimately to commercialization.
“We have already taken the first steps in creating two demonstrator and evaluation versions of this technology (line-scan-based and snapshot-based), along with a camera in a smaller form factor than what is available,” Jayapala said. “We hope this will enable our partners to validate their applications and bring this technology to market. Together, we will be able to further customize this to specific clinical applications, depending on specific application requirements.”
What exactly is a chronic wound?
Chronic wounds are, simply, wounds that fail to heal as anticipated. One of the most well-known forms is pressure ulcers – otherwise known as bedsores – injuries resulting from pressure to the soft tissue of the heels or hips, for example, or the elbows, knees or back of the head. Pressure ulcers often affect elderly, sick or disabled people who are bedridden or confined to a wheelchair. Increasing numbers of obese people are also at risk, as the additional weight can put pressure on the skin. In many cases, poor nutrition and other factors can slow healing of these wounds.
Hyperspectral imaging in the biomedical arena
Researchers are exploring the potential of hyperspectral imaging for a range of biomedical applications. These include, in addition to the diagnosis and management of chronic wounds:
• Cancer detection: Scientists at Emory University in Atlanta are looking into the possibility of using hyperspectral imaging to detect prostate cancer – for diagnosis as well as to determine tumor margins during resection. To this end, they have developed an advanced image processing and classification method for analysis of HSI data and demonstrated its utility both in vitro and in vivo. Other groups are exploring hyperspectral imaging of gastric and other types of cancer.
• Monitoring renal oxygenation during partial nephrectomy: Hyperspectral imaging can provide a highly sensitive, real-time oxygenation map enabling doctors to monitor renal perfusion/oxygenation during partial nephrectomy procedures, says a team of researchers from the University of Wisconsin School of Medicine and Public Health and several University of Texas campuses. Using the technique, they showed, for example, that baseline renal oxygenation could help to determine the risk of postoperative renal insufficiency.
• Studies of peripheral arterial disease: A group at Vanderbilt University in Nashville, Tenn., has employed HSI to investigate vascular recovery in models of peripheral arterial disease, using it to quantify blood oxygenation. In addition to elucidating the mechanisms of vascular recovery, they say, the technique can help to evaluate novel therapies in preclinical studies.