Victor Matylitsky, Herman Chui and Rajesh Patel, Spectra-Physics
New femtosecond lasers are enabling the development and fabrication of bioabsorbable and ultrafine metal stents for novel treatments.
Implantable medical devices such as stents, intraocular lenses, prosthetics and catheters are becoming increasingly complex. The feature sizes of these devices are shrinking both to address new usages and to improve patient outcomes. Stents are now being used for peripheral arteries with tiny dimensions, for example. Additionally, new device materials are being developed and incorporated to address new applications and to improve results. For instance, bioabsorbable materials that serve their targeted function and then dissolve are being pursued.
These advances in device features and materials are proving challenging for the fabrication process: As the quality of the cut edge becomes more critical with shrinking stent-strut dimensions, the degree of precision becomes more difficult to achieve. With tiny-diameter tubes, heat effect can be a problem, according to one stent manufacturer, who noted that putting heat into the tube changes its metallurgy.1 In other words, damage from heating or the heat-affected zone (HAZ) starts to become a limiting factor. For the smaller stents, it is difficult or impossible to repair the damage by post-processing.

Figure 1. The Spirit industrial femtosecond laser from Spectra-Physics delivers high-energy femtosecond pulses at high repetition rates. Images courtesy of Spectra-Physics.
Ultrashort-pulse lasers increasingly are becoming the tool of choice for fabricating these devices. Here, pulse durations are reduced to hundreds of femtoseconds – some 100,000 times shorter than pulses of conventional nanosecond lasers – and some very different physics occurs when they hit the target material. With a small dose of energy delivered in a pulse of such shorter duration at the laser’s focal spot (some microns in dimensions), the material disintegrates very precisely. And since the laser energy is delivered so quickly, this all occurs before the energy can propagate to any remaining material near the target area.
The result often is called cold or athermal laser ablation. Its salient characteristic is the remarkably clean microscale machined features it produces, generally free of burrs, melting, recast and HAZ. And its application to medical device machining is under way.
Ultrashort-pulse lasers have been around for several decades. Until recently, though, their use in manufacturing environments was limited due to their complexity, concerns about robustness, and slow materials-processing speeds.

Figure 2. Ultrafine structures micromachined in a nitinol stent with the Spirit industrial femtosecond laser by Spectra-Physics, without any post-processing. Tube diameter is 4.25 mm, wall thickness is 45 μm, and strut width is 35 μm.
An industrial femtosecond laser such as Spectra-Physics’ Spirit addresses the needs of manufacturing applications. The laser delivers high-energy femtosecond pulses at high repetition rates. The repetition rate is an important factor governing how quickly the beam may be moved over the workpiece during micromachining operations, which dictates processing speed.
Micromachining ultrafine stents
In the case of metal stents, including drug-eluting ones, shrinking dimensions allow their deployment in smaller coronary, peripheral and neurovascular blood vessels – important target areas for treatment. Some studies have also suggested a correlation between clinical outcomes and the amount of metal deployed within the vessel. Stent makers have therefore been motivated to work with thinner-walled and smaller-diameter tubes with more complex features. In 2011, an expert with extensive experience both in stent design and manufacturing forecasted that the next generation of coronary stents would have features – including struts and links – nearly half the size of then-present-day stent features.2 Another trend is to add a controlled surface texture or geometry to stents and prosthetics to improve biocompatibility, for example to reduce the risk of restenosis.
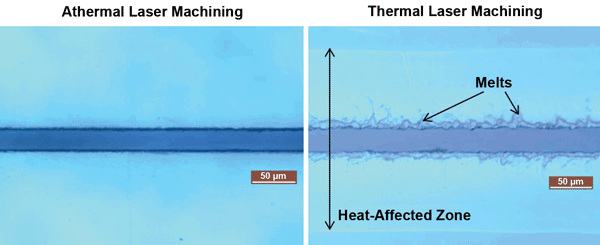
Figure 3. Laser micromachining of polylactic acid (PLLA) bioabsorbable stent material. Thermal and athermal regimes depend on laser parameters and process conditions.
To demonstrate the capability of femtosecond lasers for the fabrication of these devices, we micromachined ultrafine stent structures in thin-walled nitinol tubes. Out of a 4.25-mm-diameter tube with a wall thickness of 45 µm, a stent-like structure was machined, leaving only 35-µm-wide struts. The resulting as-cut structure, without any post-processing, is shown in Figure 2 – both the entire structure and detailed views. The cold machining process resulted in clean edges and precisely cut structures across a long length of tube with no heat-induced damage or distortion of the delicate lattice structure.
Bioabsorbable stents
Bioabsorbable stents are polymer-based devices that dissolve in the human body after serving their targeted function for a prescribed duration. This temporary implant thereby reduces the risk of complications arising from permanently implanted devices.
From a manufacturing perspective, however, these polymer-based materials cannot tolerate being heated and are extremely difficult to machine. Common polymer materials, including polylactic acid (PLLA) and polyglycolic acid (PLGA), which have low damage thresholds and melting points, are now undergoing clinical trials. PLLA, for example, has a glass transition temperature of only 61 °C and melts at 188 °C.
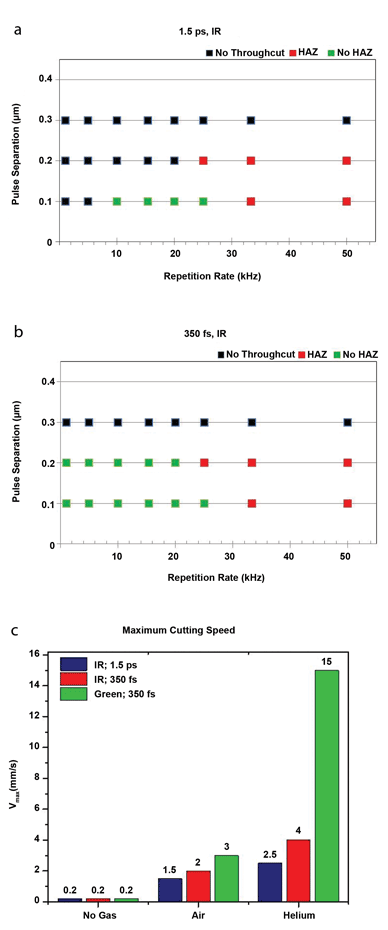
Figure 4. Machining results for 80-μm-thick PLLA. Athermal process windows (green area) as a function of laser repetition rate and pulse separation distance for: (a) 1.5-ps and (b) 350-fs pulse widths. (c) Maximum athermal cutting speed dependence on pulse width, wavelength and assist gas. HAZ = heat-affected zone.
We studied the effect of various laser parameters and assist gases on the quality and speed of machining PLLA. Two regimes in the laser-material interaction were observed, as shown in Figure 3: a thermal regime where undesirable melting and resolidification of the PLLA is seen, and an athermal or cold machining regime with melt-free features and no heat damage or HAZ.
We further systematically studied the effect of laser pulse width, wavelength and assist gas to determine athermal process windows and maximum athermal cutting speeds for 80-μm-thick PLLA – the results are summarized in Figure 4.
Femtosecond pulse widths result in significantly wider process windows for producing clean athermal results and higher athermal cutting speeds than picosecond pulse widths. Also, shorter wavelengths and the use of assist gas with high thermal conductivity (e.g., helium) result in even wider athermal process windows and increased athermal cutting speeds.
Applying this understanding, we machined stent structures in another polymer material, PLGA, using the femtosecond laser with green output wavelength. We machined a PLGA tube with wall thickness of 180 μm to create stent structures with a strut width of 200 μm (Figure 5). The result was athermal machining with melt-free features and clean, precise edges, demonstrating the benefit of cold machining with femtosecond lasers. Here, athermal ablation carried out by ultrashort-pulse lasers is not just a means of increasing cutting speed or reducing costs. Rather, these lasers fundamentally enable the bioabsorbable stent technology by creating a viable manufacturing solution.
Future directions
So what lies ahead for stents and the broader medical device industry? Current device trends will continue, driving the need to machine smaller parts with finer features and tighter tolerances. Post-processing will become more problematic as devices become smaller and more delicate, particularly as bioabsorbable materials enter the scene.

Figure 5. PLGA tube with wall thickness of 180 μm
and strut width of 200 μm, machined with a Spirit industrial femtosecond
laser by Spectra-Physics.
Laser micromachining will continue to support these trends through athermal ablation processes, delivered by the new generation of femtosecond lasers. New lasers will finally deliver on the long-held promise of ultrashort-pulse laser technology: precise athermal micromachining that is robust, reliable and fast for industrial manufacturing environments.
Meet the authors
Victor Matylitsky is business development manager for ultrafast laser applications at Spectra-Physics, a Newport company. Herman Chui is senior director of product marketing at Spectra-Physics; email: [email protected]. Rajesh Patel is the company’s director of strategic applications.
Acknowledgments
The authors would like to thank Zeus Industrial Products Inc. for providing the PLLA samples.
References
1. G. Giordano (January/February 2013). Exponential growth of medical laser applications in the U.S. LIA Today, Vol. 21, No. 1, p. 8.
2. B. Michaels (September 2011). Shrinking stents strut their stuff. Medical Product Manufacturing News, Vol. 27, No. 7.