Spectroscopy advances are steadily reducing disease-detection time frames. These new methods also hone the accuracy of disease identification and provide for more timely treatment protocols. As with anything groundbreaking, though, roadblocks inevitably arise. As with the diseases themselves, time is precious when resolving these hurdles. Sometimes, though, there’s just no time to spare.
Curing a disease is no easy task. Virtually every disease requires its own unique treatment. However, many diseases have no existing panacea despite the time, money and manpower invested in researching them. And, for those that do have treatment options available either to destroy or to curb the disease, success may come down to timing. How long has the disease been advancing, at what stage does it exist when it’s first detected and identified by medical experts, and in what stage of approval are the possible treatment protocols?
Spectroscopy advances – most notably those that have come to light in the last few years – are helping to reduce the amount of time needed to detect diseases and thereby allow for more timely and viable treatment options. Additionally, these new methods are increasing the accuracy of disease identification.
As with anything new, growing pains exist as novel developments inch their respective ways into new applications and procedures. In some cases, they’re halted from accessing a clinical setting altogether due to stringent FDA regulations and “big business” concerns.
Some lifesaving technologies – and those who invented them – are still awaiting FDA approval and the financial investments needed to transition to clinical use. Others, though, are being used in clinical settings right now.
Ahead of the curve; hampered by corporate concerns
In November 2014, BioPhotonics contributing editor Gary Boas checked in with Boston University’s Dr. Irving Bigio, who has been developing a technique called elastic scattering spectroscopy (ESS) since the 1990s (“UV-VIS Spectroscopy in the Clinic – What’s Stopping It?” www.photonics.com/A56917). ESS provides real-time, semiquantitative point-source measurements of microstructural changes and, because it can be miniaturized, can be easily incorporated within endoscopic biopsy tools.

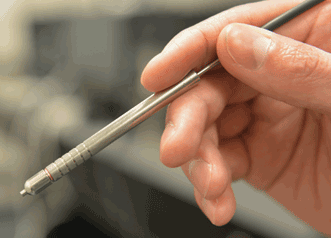
To facilitate clinical adoption of the technology, Bigio’s team developed elastic scattering spectroscopy (ESS) devices that easily integrate into endoscopic tools. An example is the incorporation of optical fibers into the biopsy forceps that doctors use to remove growths. Courtesy of Irving Bigio, Boston University.
Bigio and his colleagues already have successfully demonstrated ESS for use in a range of applications suitable to the upper gastrointestinal (GI) tract and the colon. Examples include determining the presence of dysplasia in Barrett’s esophagus, distinguishing benign from adenomatous polyps in the colon, and helping to differentiate Crohn’s disease from ulcerative colitis. ESS also showed its potential for detecting cancer in thyroid nodules and for real-time pathology to guide breast surgery.
In the June 2014 issue of Inflammatory Bowel Diseases, Bigio’s team reported a study demonstrating the use of ESS as an optical marker of inflammatory bowel disease activity. This established its potential ability to discriminate between ulcerative colitis and Crohn’s
disease.
As part of the study, they devised a diagnostic algorithm based on a pattern recognition scheme to classify measured spectra. The algorithm allowed them to determine whether any specific diagnosis obtained from an optical biopsy has a high probability of being correct. This increases the reliability of those measurements that the instrument does not deter-mine. And, for the 10 to 15 percent of cases where the algorithm indicates that some uncertainty still exists, the doctor can collect additional measurements or perform a physical biopsy.
As it stands right now, this technology has been fully mature for more than half a year. Certainly, it could benefit a range of clinical applications. To date, though, it has yet to be brought into the clinic.
One of the two primary obstacles originally faced by Bigio and his team was the reticence of clinicians, many of whom are wary of adopting new technologies – especially those that might present a steep learning curve. To address this, Bigio and colleagues designed devices that integrated seamlessly into the clinicians’ work flows. One example was incorporating optical fibers into the biopsy forceps used to remove polyps during endoscopies. Clinicians tested the new design and were very enthusiastic about it.
Problem solved? Not quite. The team now faced a more formidable obstacle: Attracting funding from an investment community that is increasingly averse to risk.

Bigio’s group already had performed large-scale clinical studies with ESS. Furthermore, these studies met performance standards established by the American Gastroenterological Association for optical biopsy tools for colonoscopy or upper GI endoscopy: 90 percent sensitivity and 90 percent negative predictive value.
Regardless, investors were (and still are) reluctant to embrace it. “There’s no venture in venture capital anymore,” Bigio said. He indicated that groups will say they are interested in a new technology but only after it has received FDA approval. Simply put, they don’t want to be involved in funding FDA trials.
Bigio confirmed that the latter imped-iment still exits. “The one (and only) obstacle that is impeding commercial development of our technology is the lack of investors willing to risk investing in a medical technology that may take a couple of years to generate profits. They seem to want technologies that are already FDA-approved,” he stated. Bigio went on to say that some potential investors currently are studying the business opportunity, but, as of this point in time, no decisions have yet been made.
Investor restraint has become a problem throughout the medical instrumentation field. The current trend is that when larger companies want new products, they simply buy existing companies. But, as Bigio indicated in June 2014, this sort of development strategy is shortsighted. Companies will buy other, smaller companies for hundreds of millions of dollars, “but they won’t spend $5 million to fund a new idea that will open a whole new product area.”
In short, more than half a year later, Bigio, his research colleagues and the technology he helped spearhead all are in the same anticipatory situation. The technology exists. In fact, it performs to standards set by the American Gastroenterological Association. However, in the clinical world – where it’s needed – the device is only as real as its existence in each respective place of treatment: It does not exist.
Cancer detection so good, biopsies are less prevalent
Not all lifesaving technologies face the quandary detailed above. One noninvasive skin cancer detection device is a prime example.
Skin cancer is the most common form of cancer and, according to the American Cancer Society (ACS), it accounts for almost 50 percent of all cancers in the U.S. In fact, the most recent ACS data indicates that 3.5 million cases of basal and squamous cell skin cancer are diagnosed yearly in this country, with melanoma expected to account for more than 73,000 cases of skin cancer this year alone.
About eight months ago, a new device hit the medical world that offers doctors the potential to see a clearer picture of cancerous skin lesions and thereby reduce unnecessary biopsies. A team at the University of Texas at Austin developed a probe that combines three distinct spectroscopy methods to measure the properties of skin tissue: Raman spectroscopy, diffuse reflectance spectroscopy and laser-induced fluorescence spectroscopy. The 3-in-1 device offers a fast, comprehensive and noninvasive examination of melanoma and other skin cancer lesions.
The 3-in-1 spectroscopy probe. Courtesy of James Tunnell and Austin May, University of Texas at Austin.
According to the researchers, the probe reveals information invisible to the human eye, offering a better screening tool for cancer that can eliminate many negative biopsies. They noted that as normal skin becomes cancerous, cell nuclei enlarge, top layers of skin thicken, and skin cells increase their consumption of oxygen and become disorganized. These changes alter the way light interacts with the tissue.
Diffuse optical spectroscopy can be sensitive to absorption by proteins such as hemoglobin, while Raman spectroscopy is sensitive to vibrational modes of chemical bonds, including those found in connective tissues, lipids and cell nuclei.
Currently, as per the researchers, the only definitive way to diagnose skin cancer is to perform a biopsy. However, determining which lesions to biopsy can be an imprecise process. For every case of skin cancer detected, approximately 25 negative biopsies are performed. The researchers noted that this can be expensive and sometimes unnecessarily time-consuming.
“Skin is a natural organ to apply imaging and spectroscopy devices to because of its easy access,” said Dr. James Tunnell, an associate professor of biomedical engineering at the University of Texas at Austin. He went on to say, “This probe that is able to combine all three spectral modalities is the next critical step to translating spectroscopic technology.”
Dr. Tunnell told BioPhotonics about progress updates, stating, “We are planning clinical studies starting this summer.” It should also be noted that this device took to the winner’s podium at the annual South by Southwest Interactive Innovation Awards, claiming victory in the “SciFi No Longer” category. The event took place in Austin, Texas, on March 17, 2015.
Meet the author
Rodd M. Pedrotti is editor of BioPhotonics; email: [email protected]