A research team led by engineers at the University of California, Berkeley has developed a new mobile phone microscope capable of analyzing blood. Its primary purpose is to automatically detect and quantify bodily infection caused by parasitic worms.
The next generation of UC Berkeley's CellScope technology, its abilities to provide critical information to health providers in the field could help revive efforts to eradicate debilitating diseases in Africa.
"We previously showed that mobile phones can be used for microscopy, but this is the first device that combines the imaging technology with hardware and software automation to create a complete diagnostic solution," said Daniel Fletcher, an associate chairman and professor of bioengineering at UC Berkeley whose lab pioneered the CellScope.
Having teamed up with Dr. Thomas Nutman of the National Institute of Allergy and Infectious Diseases, as well as with collaborators from Cameroon and France, the UC Berkeley team conducted a pilot study in Cameroon, where health officials have been battling the onchocerciasis (river blindness) and lymphatic filariasis, both of which are caused by parasitic worms.
Using motion instead of molecular markers or fluorescent stains to detect the movement of worms, the researchers found that the video CellScope was as accurate as conventional screening methods.
River blindness is transmitted through the bite of blackflies and is the second leading cause of infectious blindness worldwide. Lymphatic filariasis, which is spread by mosquitoes, leads to elephantiasis, a condition marked by painful, disfiguring swelling in parts of the body. It is the second leading cause of disability worldwide and, like river blindness, highly endemic in certain regions in Africa.
Although the antiparasitic drug ivermectin, or IVM, can be used to treat these diseases, mass public health campaigns to administer the medication have been stalled due to the potentially lethal side effects for patients also infected with Loa loa, or African eye worm, which causes loiasis. When there are high circulating levels of microscopic Loa loa worms in a patient, treatment with IVM can lead to brain damage or other severe or fatal neurologic issues.
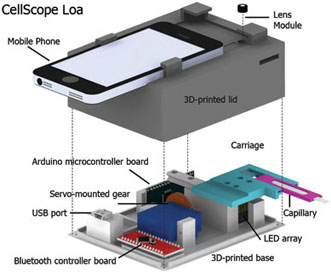
A schematic of the CellScope Loa device, a smartphone-based video microscope. It includes a 3D-printed case housing simple optics, circuitry and controllers to help process the sample of blood. CellScope Loa can quantify levels of the Loa loa parasitic worm directly from whole blood in less than 3 minutes. Courtesy of Mike D'Ambrosio and Matt Bakalar, Fletcher Lab, UC Berkeley.
For this latest generation of the mobile phone microscope, fittingly named CellScope Loa, the researchers paired a smartphone with a 3D-printed plastic base, where the sample of blood is positioned. The base includes LEDs, microcontrollers, gears, circuitry and a USB port.
Control of the device is automated through a proprietary, purpose-specific app developed by the researchers. The phone communicates wirelessly to controllers in the base to process and analyze the blood sample. Gears move the sample in front of the camera, and an algorithm automatically analyzes the telltale “wriggling” motion of the worms from the phone's captured video. The worm count is then displayed on the screen.
The procedure takes approximately two minutes or less, starting from the time the sample is inserted to the display of the results.
"This research is addressing neglected tropical diseases," Fletcher said. "It demonstrates what technology can do to help fill a void for populations that are suffering from terrible but treatable diseases."
The standard method of screening for levels of Loa loa involves trained technicians manually counting the worms in a blood smear using conventional laboratory microscopes, making the process impractical for use in field settings and in mass campaigns to administer IVM.
Fletcher said previous field tests revealed that automation helped reduce the rate of human error. The short processing time allows health workers to quickly determine on site whether it is safe to administer IVM.
The researchers are now expanding the study of CellScope Loa to about 40,000 people in Cameroon.
The results of the pilot study were published Science Translational Medicine (doi: 10.1126/scitranslmed.aaa3480).
For more information, visit www.berkeley.edu.