A low-cost, portable, battery-powered microendoscope developed at Rice University could reduce the need for costly biopsies for many patients undergoing screening for esophageal cancer.
That's the conclusion of researchers behind a clinical study involving 147 patients in the U.S. and China at high risk for esophageal squamous-cell neoplasia. The trial explored whether the new fiber-optic imaging system could reduce the need for biopsies when used in combination with a conventional endoscope, the worldwide standard of care for esophageal cancer diagnoses.

Microendoscope images show healthy tissue, top, as compared to cancerous cells with irregularly shaped and enlarged nuclei, bottom. Courtesy of the Richards-Kortum Lab/Rice University.
All 147 patients with suspect lesions were examined with both a traditional endoscope and Rice's microendoscope. Biopsies were obtained based on the results of a traditional endoscopic exam.
A pathology exam revealed that more than half of those receiving biopsies – 58 percent – did not have high-grade precancer or cancer. The researchers found that the microendoscopic exam could have spared unnecessary biopsies for about 90 percent of the patients with benign lesions.
"For patients, biopsies are stressful and sometimes painful," said lead researcher Rebecca Richards-Kortum, a professor of bioengineering and electrical and computer engineering at Rice and director of the Rice 360° Institute for Global Health Technologies.
"In addition, in low-resource settings, pathology costs frequently exceed endoscopy costs," Richards-Kortum said. "So the microendoscope could both improve patient outcomes and provide a significant cost-saving advantage if used in conjunction with a traditional endoscope."
Rice's high-resolution microendoscope uses a 1-mm-wide fiber-optic cable attached to the standard endoscope. The cable transmits images to a high-power fluorescence microscope, and the endoscopist uses a tablet computer to view the microscope's output. The microendoscope provides images with similar resolution to traditional histology and allows endoscopists to see individual cells and cell nuclei in lesions suspected of being cancerous.

Richards-Kortum's lab specializes in the development of low-cost optical imaging and spectroscopy tools to detect cancer and infectious disease at the point of care. Her research group is particularly interested in developing technology for low-resource settings, and the microendoscope was developed as part of that effort.
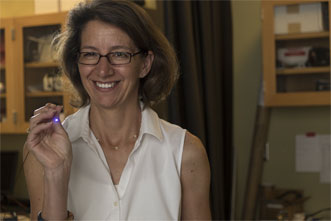
Rice University professor Rebecca Richards-Kortum holds a fiber-optic cable attached to a microendoscope that could reduce the need for costly biopsies for many patients undergoing screening for esophageal cancer. Courtesy of Jeff Fitlow/Rice University.
It is battery-operated, inexpensive and requires very little training to operate. Results from the clinical study verified that both experienced and novice endoscopists could use the microendoscope to make accurate assessments of the need for a biopsy.
Clinical studies of the microendoscope are either planned or underway for a dozen types of cancer including cervical, bladder, oral and colon cancers.
"More than half of cancer deaths today occur in the developing world, often in low-resource areas," Anandasabapathy said. "The World Health Organization and other important international bodies have called for increased global focus on noncommunicable diseases like cancer, and Rice's microendoscope is a great example of what the right kind of technology can do to change health care in low-resource countries."
The clinical trial results were published in Gastroenterology (doi: 10.1053/j.gastro.2015.04.055).
For more information, visit www.rice.edu.