From the ubiquity of smartphones to an aging population, the modern world offers the optical sector a wealth of opportunities to innovate for the health care sector.
Optical technologies have a long history of providing a rapid and noninvasive way of diagnosing, imaging and operating that other methods simply cannot match. It’s little wonder then that the health care sector continues to call for fresh ideas from the optics industry.
From novel therapies to adding new functionality to existing devices, in addition to exploiting the huge growth of products in the consumer market, the opportunities for innovation are extensive. But bringing new devices to market can be problematic — it’s sometimes not enough to have a great idea. There are strict regulations to navigate, extensive trial periods to fund, and technological issues associated with product scale up and pilot manufacturing.
But the rewards are there for the tenacious, and with so many factors driving growth in health care, there is no shortage of avenues to explore.
Growth of optics in medicine comes down to two main drivers: The first is related to health care — with an aging population and an increase in lifestyle-related diseases, there’s no doubt that we are all demanding more from the health care sector.
The second driver is technological. Progress in the development of enabling technologies such as photonics, micro- and nanotechnologies, information and communications, innovative materials and manufacturing systems are paving the way for novel health care applications in therapies, diagnostics, surgical interventions and imaging.
Technology drivers
Light Sources:
• Improvements in the brightness, efficiency, size, form factor and cost of LEDs, lasers and OLEDs.
• UV LED development in the UV-B spectrum (280 to 315 nm) is important for light-based therapies. UV-C spectral range (100 to 280 nm) is important for sterilization applications. Hayward, Calif.-based RayVio, a UV LED specialist with technology originally developed at Boston University, recently announced a deep UV LED emitting 45 mW CW with a power density of 30 W/cm2 for example.

An example of OLED lighting samples. Courtesy of CPI.
• Increasing availability and increased power output from mid-infrared (MIR) laser sources is another market driver. Water exhibits strong absorption lines in the MIR region, especially near 3 and 6 μm. This causes strong MIR absorption in human skin, which facilitates biomedical applications in laser surgery, tissue ablation and photo dermatology.
Optical Sensors and Detectors:
• Biomedical sensing using fiber optic sensors incorporated into catheters and endoscopes is also an existing market with large potential to expand.
Smartphones:
• Increasing access to mobile phones with large amounts of computing power equipped with a high-resolution camera.
• A smartphone with a 40-MP camera can be turned into a high-resolution imaging sensor for point-of-care diagnostics.
High-speed Internet:
• Enables access to the Cloud for upload and download of data to medical devices worn or operated by the patient.
Novel materials and manufacturing systems:
• Help deliver these devices and products at lower cost and added functionality.
• Improvements in the technology used to manufacture engineered nanoparticles for image contrast enhancement (e.g. photothermal imaging).
• In laser machining, femtosecond laser systems are becoming more affordable and reliable. Such systems can be used for high-precision manufacturing of medical devices such as stents or for performing surgery.
In order for a new device to achieve commercial acceptance, it needs to be more accurate, more repeatable, of lower total cost, easier to use, or be more effective than those currently used.
This is no easy task, particularly for university startups, early stage companies and small- to medium-sized enterprises (SMEs). Entrepreneurs with limited finances can often struggle to gain access to expensive equipment or fund the extensive trial periods needed to bring new medical devices to market.
In a bid to address the major barriers and help bring new photonic technologies into clinical use, a new National Centre for Healthcare Photonics is being created at NETPark, Sedgefield, County Durham, England. Due to open in early 2017, the center has secured £10 million (about €14 million) from the North East Local Economic Partnership (NE LEP) in principle and will leverage about an additional £8 million (about €11.2 million) from industry and other collaborative R&D projects.
The center is being established and run by, an England-based technology innovation center with a track record of bringing new emerging technologies to market. CPI will work in close partnership with other key stakeholders and organizations to create an ecosystem for innovation in health care photonics.

The cleanroom facilities at CPI could help university startups and SMEs bring their medical devices to market. Courtesy of CPI.
“For U.K. manufacturing to make [the]most of the opportunities in health care photonics, it is essential to reduce the barriers that are preventing innovation from moving beyond the laboratory and into health care devices for patients,” said Dr. Tom Harvey, head of technology for Healthcare Photonics at CPI.
“We are initially looking to identify specific clinical needs-based projects based on the main themes of photonics for therapy, diagnostics, imaging and surgery,” he continued. “In support of these projects, the center can provide facilities to help with prototyping, build and testing of preproduction prototype devices, pilot manufacturing, and photonics modeling and simulation expertise.”

A light blanket for the treatment of a baby born with jaundice. Courtesy of CPI.
One such company that could benefit from the facility is England-based PolyPhotonix, a biophotonic research and development company that has been closely working with CPI to design, develop and manufacture noninvasive photonic-based medical devices.

It’s all about fusion
For industry giants such as Carl Zeiss AG and Leica Microsystems GmbH that have a long tradition in bringing optical innovations to medical health care, it’s all about combining different technologies to create the best possible device to enable doctors to improve workflows and treatments. Both companies have recently included optical coherence tomography (OCT) imaging capabilities in their surgical offerings. This added functionality enables eye surgeons to identify structures during operations that were previously hidden from sight.
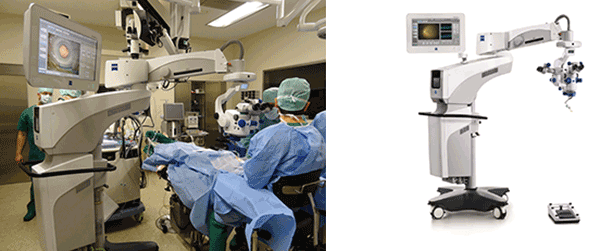
The Zeiss Opmi Lumera 700 surgical microscope and Zeiss Rescan 700 OCT
device superimposes high-resolution OCT images on the view through the
surgical microscope, providing ophthalmologists with a view beneath the
surface of the tissue. Images courtesy of Zeiss.
“The first surgical microscope was developed by Zeiss more than 50 years ago and OCT was also first brought to ophthalmology by Zeiss,” said Jann Gerrit Ohlendorf, director of communications at the medical device business of Zeiss. “Thanks to this smart combination of two trusted technologies, doctors can now adjust their method of operation during surgeries. Other solutions on the market do not allow for these insights into the transparent structures of the eye.”
With the Zeiss Opmi Lumera 700 surgical microscope and Zeiss Rescan 700 OCT device, high-resolution OCT images appear in the eyepiece as real-time images superimposed on the view through the surgical microscope.
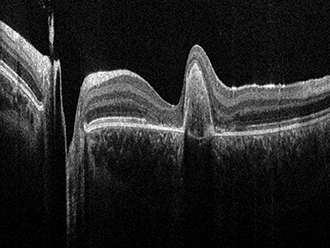
An OCT image of a human retina acquired with the Bioptigen Envisu C2300. Courtesy of Leica Microsystems.
A good example of what that means for ophthalmology is the phenomenon known as epiretinal gliosis. This is a macular disorder in which cells grow over the retina to form a membrane that must be surgically removed to avoid impaired vision. The problem is that the membrane is extremely thin and transparent. But thanks to the combined imaging system, surgeons can now see this membrane more clearly and can adjust their technique as they work, for example, by switching surgical instruments to avoid putting too much pressure on the retina.
“Intraoperative OCT and multimodal imaging are rapidly evolving fields within ophthalmic surgery and offer excellent development opportunities for young professionals to shape future Zeiss products and tangibly help doctors reach even better outcomes for their patients,” said Christoph Hauger, director of advanced development at the medical device business of Zeiss.
Health care drivers
In developed nations, life expectancy is on the rise and so, too, are many age-related maladies such as cancers and neurodegenerative diseases including Alzheimer’s and Parkinson’s. Adding further pressure to the health care sector is the increase in lifestyle-related diseases such as Type 2 diabetes and heart disease.
We are also expecting more from our health care providers. Patients are calling for the introduction of personalized and stratified medicine, early diagnosis of disease, prevention rather than cure, care closer to the home and continuous health monitoring rather than periodic sampling, among others.
“Optical technology provides the means for contact-free imaging and analysis, and hence is superior to other methods that need to extract sample parts for physical and/or chemical processing and analysis,” said Sebastian Tille, director of business development at Leica Microsystems. “Furthermore, optical imaging methods provide a way of correlating structural and functional information about the sample — even highly localized down to tens of nanometer precision (using superresolution microscopy) or penetrating several millimeters into tissue [using OCT].”
Having recently acquired Bioptigen Inc., a technology leader in the field of OCT, Leica Microsystems is extending its reach into the medical domain. An example is the U.S. FDA-cleared and EU CE-marked Envisu C2300 OCT for handheld, pediatric and perioperative applications. Other advanced ophthalmic OCT imaging systems are used in preclinical research.
“Thanks to the know-how of our engineers, specifically around design of the spectrometers — the heart of OCT devices — the Bioptigen Envisu OCT systems excel through a set of performance
parameters,” Tille said. “We will further push the performance parameters like speed, resolution and sensitivity, as well as find suited combinations with other imaging modalities to push utility and generate more insights, similar to developments in fluorescence microscope[s], which also is a nice complement.”
While first-world countries can enjoy access to the latest cutting-edge technologies, third-world countries pose another set of problems. In rural destinations, the need for remote diagnostics becomes crucial: There often is no reference laboratory or qualified personnel available, so a patient must be diagnosed from a distance by sending information either through wire or wirelessly.
“We [Zeiss] are facing the challenge of poor infrastructure and a lack of awareness for the importance of high-quality instruments in diagnosis,” said Peter Kraemer, who is responsible for education and routine microscopy at Zeiss. “It is often hard to convince doctors and medical staff in heavily burdened countries to invest the existing budget in long-term solutions, meaning high-quality microscopes and reliable equipment.”
A potential solution is the Zeiss imaging app Labscope, plus iPad and the Zeiss Axiocam ERc 5s microscope camera, which both support remote diagnostics. The camera provides 5-MP color images that can be used with a PC to capture images or video for observation of dynamic processes. Users can then store microscope images directly on an SD card and transfer them to a computer to share with colleagues or experts via the Internet.