Capable of providing streamlined access to medical data in real time, and with the ability to perform diagnostics in remote areas, portable imaging technologies for medical applications are of increasingly significant interest to medical practitioners and technology companies alike.
It takes some clever thinking to shrink many of the cumbersome biological imaging tools in use today to a size where they can be taken directly to the bedside. For some patients, point-of-care imaging is the only option.
Portable imaging devices have grown in importance due to the numerous benefits they offer. They simplify hospital workflows, can easily be shared between care centers (which helps relieve the strain on hospital budgets), and offer medical accessibility to patients who cannot be seen in an office, such as those under home care or in remote or underdeveloped areas.
Stripping down a device to its essential components without compromising image quality, performance or reliability can be challenging. Moreover, it’s an expensive endeavor.
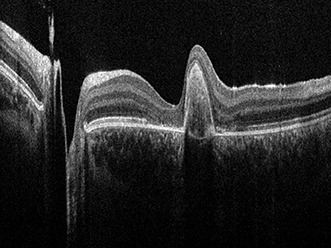
An OCT image of a human retina acquired with the Envisu C2300 SD-OCT system. Courtesy of Leica.
Handheld OCT instruments
Optical coherence tomography (OCT) is a noninvasive, noncontact optical imaging technique that has become a standard modality for diagnosing and monitoring retinal diseases in ophthalmology. However, most commercial OCT systems are bulky and table-mounted, thereby limiting their accessibility for use in screening applications.
Eye-care specialists long have recognized the importance of screening for the early detection of many sight-limiting conditions like age-related macular degeneration and diabetic macular edema, as well as neuro-degenerative diseases such as Parkinson’s and Alzheimer’s.
Handheld OCT devices, such as those developed by Optovue Inc., Thorlabs Inc. and Bioptigen Inc. (the latter of which was recently acquired by Leica Microsystems GmbH and is referred to herein as Leica). These devices help ophthalmologists monitor patients with sufficient sensitivity while remaining easy-to-use and portable tools. As a result, screenings can be performed outside of standard optometry settings.

A handheld photoacoustic (PA) probe uses compact diode lasers to image several centimeters deep into tissue without contrast agents. The combined PA-and-ultrasound system is in the process of being commercialized by Esaote. Courtesy of Pim van den Berg and Khalid Daoudi.
The offerings from Leica and Optovue are based on spectral domain OCT (SD-OCT), which delivers a high signal-to-noise ratio, excellent axial resolution and deep imaging depths into human tissue. In the approach, interferometry is used to create cross-sectional views of different tissue types.
Leica’s Envisu C2300 SD-OCT system uses low-power, near-infrared light to generate high-resolution, volumetric images of the eye. It includes a 160-nm spectrometer that employs a 2048-pixel line-scan camera coupled to a broadband superluminescent diode light source centered at 880 nm.
“The Envisu C2300 SD-OCT system includes a handheld optical scan head fed by a 2-meter-long fiber optic tether cable,” said Sebastian Tille, director of business development at Leica. “The optical signal is scanned across the ocular target via a set of galvo-driven mirrors, enabling 32,000 scans/second with very high sensitivity. A single scan already delivers high-quality OCT images, which eliminates the need for averaging and thus increases productivity even if patient[s’] eyes are moving.”

The iScan machine is a portable, tabletop OCT system weighing just 43 lbs. Patients can be scanned in a variety of settings. Courtesy of Optovue.
The FDA-approved system is already used in several health care facilities, enabling treatment for patients who cannot easily come to or sit at a standard desktop device. So, for the elderly, children and patients suffering from certain types of wounds, portable OCT devices may be the only means of getting the treatment they need.
“Another important application is for OCT images in the operating room,” Tille said. “The Envisu C2300 OCT mobile cart can be moved into an operating room, where imaging can be conducted on anesthetized patients by an MD or ophthalmic photographer either handheld or with the scan head affixed directly to the side of a microscope.”
Optovue’s SD-OCT solution uses an 840-nm-wavelength scan beam that is projected into the eye. The resulting backscatter is collected, processed through a spectrometer and then recorded by a sensor. By scanning millions of reflected profiles, it forms a 3D representation of the tissue.
“Many eye-care professionals have multiple offices, yet can’t justify purchasing an OCT for every location,” said Paul Kealey, Optovue’s senior vice president of product strategy. “The iScan system is a lightweight, compact design with plug-and-play installation, so clinicians can easily move the OCT from location to location.”
Researchers at the Massachusetts Institute of Technology (MIT) have taken a slightly different approach by developing an ultrahigh-speed, handheld swept-source OCT (SS-OCT) system. Using Thorlabs’ high-speed MEMS-VCSEL swept laser source technology, the team worked to build a compact and lightweight device that uses a 2D microelectromechanical systems (MEMS) scanning mirror (as opposed to a galvanometer mirror pair) for beam scanning. It was presented in the team’s publication in Biomedical Optics Express (doi: 10.1364/BOE.5.000293).
The device employs an optically pumped vertical-cavity surface-emitting laser (VCSEL) operating at a 1060-nm center wavelength, yielding a 350-kHz axial scan rate and 10-μm axial resolution in tissue. Two orthogonally scanned volumes can be processed to generate a motion-corrected merged volume; this successfully tackles any adverse issue regarding a patient’s eye movement.
The device’s cost, however, is an issue. Currently, it’s too expensive for nonspecialist screening applications. With the majority of the cost due to the VCSEL and data acquisition electronics, Thorlabs has several active projects targeting custom-designed electronics and a more simplified, electrically pumped VCSEL that will help to significantly reduce this cost.
Portable microscopes
In a bid to encourage pioneering solutions for some of the world’s biggest health care issues, the Foundation for Innovative New Diagnostics (FIND), which is sponsored by the Bill & Melinda Gates Foundation, approached microscopy specialist Zeiss with a challenge.

The Zeiss portable microscope offers both bright-field excitation and fluorescence illumination for the reliable diagnosis of TB, and is small enough to be transported in a case. Courtesy of Zeiss.
FIND and Zeiss jointly developed a portable microscope that offers both bright-field excitation — the gold standard for tuberculosis (TB) detection — and fluorescence illumination to enable the reliable diagnosis of TB. It can even be used in areas without a power supply.
“At remote rural destinations, especially in Third World countries, there often is no reference lab or qualified personnel available. Therefore, it is an advantage to be able to separate place of examination from place of diagnosis,” said Dr. Silvia Zenner-Gellrich, manager of market segment Education and Routine at Zeiss. “Time to result becomes shorter and treatment much more efficient and faster. This is called remote diagnostics.”
The company’s Primo Star iLED system has been adapted to detect TB even under challenging rural conditions like moisture, unstable power conditions and poor infrastructure. When used with Zeiss’ iPad imaging app, Labscope, users can store microscope images directly onto an SD card and transfer them later to a computer or share them with colleagues and experts via the Internet.

The Primo Star iLED is small and portable, and can be operated with a battery pack in locations with no electricity or an unreliable power supply. Courtesy of Zeiss.
“It is small, portable and reduced to its essentials,” Zenner-Gellrich said. “Fluorescence is excited with an energy-saving LED. In remote areas with fluctuating or no electricity, the battery pack can be used. If the electricity supply is unstable or fails, the microscope can be operated for a few hours using batteries.”
Although many instruments have already been sold in Ethiopia and to Doctors Without Borders/Médecins Sans Frontières (MSF), Zenner-Gellrich points out that they are facing the challenge of poor infrastructure and a lack of awareness for the importance of high-quality instruments in diagnosis.
“It is often hard to convince doctors and medical staff in heavily burdened countries to invest the existing budget in long-term solutions, meaning high-quality microscopes and reliable equipment.”
Combining technologies — the future of imaging
According to Leica’s Tille, portable imaging systems inside hospital and clinical settings will evolve to include multiple imaging modalities in a single device. In fact, evidence of this already is being demonstrated in some of the latest innovations, which currently are at proof-of-concept stages.
The company Royal Philips launched its Digital Accelerator Lab in late 2012 and has centers in the Netherlands and India. Using this lab, scientists have collaborated with researchers from Accenture Technology Labs to explore the potential use of Google Glass in clinical settings. The result is a proof-of-concept, head-wearable display that allows any doctor performing a surgery to simultaneously monitor a patient’s vital signs without ever having to take his or her eyes off the procedure or the patient.
Combining technologies from Google and from Philips’ IntelliVue product line enables a patient’s vital signs to be transferred into Google Glass, giving doctors hands-free, voice-controlled access to critical data while in the operating room or even on the go in the hospital.

The iStand expands the clinical utility of the iVue OCT system by allowing patients to be scanned in supine and various other conditions. The iStand also makes it possible to roll the iVue OCT system between exam lanes, procedure rooms and satellite offices. Courtesy of Optovue.
“Better access to the right information at the right time allows a clinician to increase focus on better patient care,” said Hans Notenboom, global head of digital at Philips’ Healthcare Informatics Solutions and Services. “Philips foresees an increase in wearable technology across the entire health continuum.”
“Delivering pertinent clinical data to where clinicians need it most to help improve outcomes across the health continuum from healthy living, prevention
and diagnosis, to treatment and home care, is a key area of focus for Philips,” added Notenboom.
In another example of combining modalities, researchers at French-based Silios Technologies and Quantel Laser, as well as from the Netherlands-based Esaote Europe BV and the University of Twente, have integrated a photoacoustic (PA) imaging device into an ultrasound system. The team’s paper was published in Optics Express.
In it, the team presented a handheld PA probe that uses compact and cost-effective pulsed diode lasers to allow for real-time imaging. “Photoacoustics is capable of imaging the blood vessel network with submillimeter resolution at several centimeters deep in tissue without use of contrast agents,” said Professor Wiendelt Steenbergen and Dr. Khalid Daoudi, both of the University of Twente.
For a good-quality signal, very short pulses at sufficiently high energy levels are needed. Quantel and the company BrightLoop contributed the laser diode stacks and drivers, which delivered pulses in the range of 100 to 150 ns at up to 1 mJ. The beam-shaping expertise was provided by Silios.
“The beam is homogenized and sized to avoid any damage on the skin. We develop[ed] an optical system combining diffractive optical elements (DOEs) and refractive components,” said Dr. Stéphane Tisserand, CEO at Silios. “The manufacturing cost of our optical system has to be low enough to keep the photoacoustic hand piece price in the range of [a] commercial acoustic hand piece. This can be achieved as the DOEs are manufactured in a [collective] manner onto silica wafers, like in the semiconductor industry. Moreover, the refractive part of the system has been designed using off-the-shelf components to optimize the costs.”
The work is part of the FULLPHASE project supported by the European Commission and tp21, a Berlin-based project management consultancy. The project’s overarching goal is to transform PA imaging from a lab-based technique to a low-cost, portable multiwavelength combined PA-and-ultrasound system that will be commercialized by Esaote.
While PA currently lacks clinical data, the team is currently investigating clinical applications, such as rheumatoid arthritis in finger joints, cardiovascular disease, diabetes and burn wounds. The outcome will play a crucial role in the further development and commercialization of this combined PA-and-ultrasound system.
“The aim in these programs is to develop a product and to market it very soon after the end of the project [i.e., September 2016],” added Tisserand.