Lasers cut the time wounds take to heal, but costs still need to be sliced and systems need to be smaller and less complicated.
In surgery, the best cut is often the smallest. Because they enable precision targeting and can minimize tissue trauma, lasers offer an advantage in surgery. What’s more, they can deliver healing light, thereby widening treatment possibilities. But to win wider acceptance and greater use, laser surgery systems need to cost less while being more versatile and user-friendly. Progress is being made in these areas but more must be done.
As for the smallest cut being best, that’s the idea behind minimally invasive surgery, where incisions may be half or less the length of the traditional approach. As a result, patient recovery time can be reduced from months to weeks or days, depending on the type of surgery.
A patient undergoes dental treatment with a laser. Courtesy of Biolase.
Lasers offer advantages in minimally invasive procedures, said Dr. Samuel B. Low, a professor emeritus of periodontics at the University of Florida in Gainesville. A practicing periodontist, Low noted that laser surgery often means no knife, blade or suturing, resulting in faster healing and higher patient-reported comfort.
What’s more, a laser can confer an added benefit, Low said. “It centers around the area of biostimulation and accelerated wound healing.”
For periodontists, who deal with gums and other supporting tooth structures, this means that as a result of laser treatment it may be possible someday to regrow a patient’s own tissue. Surgery would then be additive without the need to resort to grafts or the like.
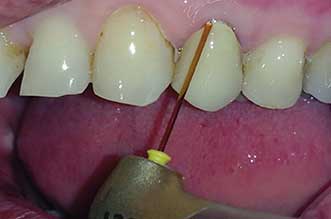
Lasers can eliminate the use of needle and drill for tooth and gum surgery. Courtesy of Dr. Samuel B. Low.
Importantly, the use of a laser may remove the need for a numbing injection. One of the chief reasons why people, particularly children, dread seeing a dentist and put off visits is fear of the needle, according to Low. With a laser, both needle and drill can be largely eliminated.
Low is a consultant for Biolase of Irvine, Calif. The company supplies laser systems for dental surgery and related applications. Diode lasers in the 810-980 nm range are used for soft tissue because the wavelengths target hemoglobin and water. For tooth enamel, the hardest substance in the body, the company turns to erbium, chromium doped yttrium scandium gallium garnet (Er,Cr:YSGG) lasers operating at 2780 nm. That wavelength is absorbed well by water and the hydroxyapatite that makes up most of the enamel.
Biolase President and CEO Harold C. Flynn Jr. noted that traditionally treatment of disease under the gums has required cutting into large sections of tissue. Doing the same with a laser involves minimal cutting and pain, thanks in part to active cooling of the site using water and air.
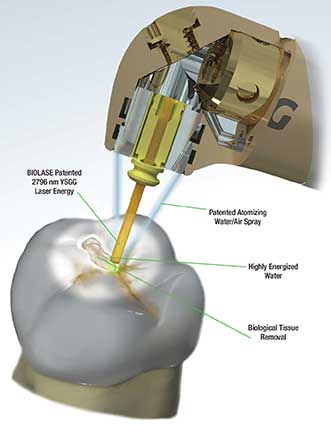
How a laser is used in dental treatment. Courtesy of Biolase.
There also is another benefit to surgery done with a laser, Flynn said. “You get less infection because the laser actually disinfects at the same time and gets rid of pathogens. Researchers report that our wavelengths will break down endotoxins and biofilms that create complications.”
Flynn predicted that lasers for the treatment of cavities, gum disease and other oral health conditions are about to take off. In part, this is due to advances in laser technology, such as the refinement of flash lamp systems that offer hundreds of kilowatts of peak power in microsecond-long pulses. Such power is needed because enamel is very hard, Flynn noted.
Another reason for the predicted growth of these laser surgery applications is the development of systems that can be better integrated into a dental chair. This is important, because as illustrated by the Biolase products, multiple systems operating at different wavelengths may be needed. Consequently, making systems compact and inexpensive is critical. That may be even more important if biostimulation is added to the mix.
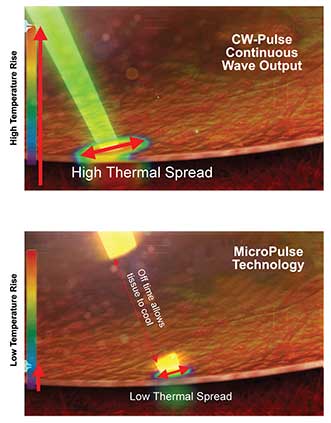
The best results occur when wavelength, pulse width, power and other parameters of surgical lasers are optimized. Courtesy of Iridex.
The need to cut the cost and size of laser-based surgery systems was also mentioned by Amir Lichter, vice president of global R&D at Yokneam, Israel-based Lumenis. Among other things, the company makes CO2 laser systems of 10.6 micron operating wavelength for ear, nose and throat surgery, as well as for treating fertility-related disorders. Lumenis also makes 2.1 µm-operating wavelength holmium lasers for men’s health issues and a Nd:YAG holmium combination product for other applications.
Lichter also cited the need to combine lasers with radio frequency and other energy sources. Doing so will allow each energy source to offer its own unique capabilities. For instance, lasers can cauterize a blood vessel opened up during a procedure and physicians particularly appreciate that capability, according to Lichter.
He added that a final important trend for the future involves integrating a laser into the operating room and connecting it with the patient database. A surgeon might then have ready access to diagnostic information, such as from an x-ray.
“Just imagine if a doctor can see an image of an internal organ with extreme magnification and target his laser device exactly to the point he wishes to hit. Not only this — a doctor may even be able to see the results in real time and change the parameters of the treatment accordingly,” Lichter said.
A different focus is being taken by Iridex of Mountain View, Calif. Its laser systems are used to treat retina diseases and glaucoma. In the past, laser surgery in these areas was in the form of microdissection, said Timothy D. Buckley, vice present of global sales and marketing. In essence, lasers were used to make controlled burns, destroying tissue while cauterizing surrounding blood vessels.
Today Iridex aims to get the same therapeutic response with no damage, Buckley said. This is possible because diagnostic tools exist that allow the cellular response to be measured, which means that the response can be optimized by tuning beam wavelength, pulse width, power and other parameters. This can reduce the ongoing cost of treatment by as much as tenfold, as compared to the pharmaceutical route, according to Buckley.
He added that key to gaining broad acceptance of such an approach is improving the portability and lowering the cost of systems. That’s especially important for the emerging economies found in Africa and elsewhere.
There are still laser-based systems that do eye surgery of the subtractive type. For instance, cataract treatment procedures make use of very short pulse width lasers because these enable precision cuts. “Right now femtosecond lasers, where it’s commercial, are in microdissection, very controlled surgical steps to minimize collateral damage,” Buckley said.
In a final example, Elesta of Florence, Italy, makes 1064-nm wavelength Nd:YAG laser systems for the ablation
of malignant liver tumors or benign thyroid nodules, with ultrasound imaging the tissue. Once the target is located, a thin flexible fiber, measuring perhaps only 0.3 mm, is inserted and guided to the proper spot. Within 15 minutes of lasing, the target is destroyed, said Luca Breschi, R&D manager.
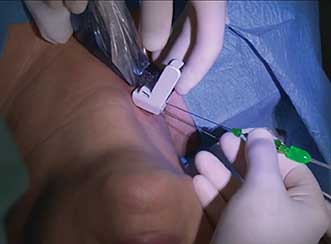
With ultrasound guiding the placement of fiber optic bearing needles, surgeons use a laser to destroy thyroid nodules. This prevents the thyroid from having to be removed and the patient then having to take thyroid replacement hormone for life. Courtesy of Dr. Teresa Rago, Cisanello Hospital.
Minimally invasive surgical techniques are becoming more and more important due to the need to reduce cost and improve patient quality of life, he said. For example, laser elimination of thyroid nodules can keep a patient from having to undergo surgery to remove the thyroid and ending up on thyroid replacement therapy for the rest of his or her life.
“The laser has a key role due to the very thin and flexible fiber optics that can deliver laser energy in every part or organ, opening the way to treat a very big number of pathologies of the human body,” Breschi said of this future trend.
In surgery applications, the laser is often not the most expensive or time-consuming aspect of the system. Instead, that distinction may belong to securing regulatory approval, which requires extensive documentation, said Richard Jollay, a senior product manager at B&W Tek of Newark, Del. The company supplies medical-device-capable diode lasers and systems.
The extensive paperwork impacts laser surgery systems in various ways. One is that vendors are reluctant to make changes that would trigger the need for a recertification. Another involves the nature of the equipment itself.
“We don’t typically try to use the very latest state-of-the-art electronics or things like that because we have to buy components that have been certified,” Jollay said.
As for future trends, aside from the need to cut costs and shrink the size of systems, another likely requirement is increased flexibility and greater user-friendliness. Both arise because users are not laser experts, and that fact impacts everything from system setup to safety. Also, no single combination of wavelength, pulse width, power and other laser parameters works best for all tissue. In the case of dental surgery, for instance, one wavelength of choice is in the near infrared range below 1000 nm while the other is in the mid-IR at about 3000 nm.
Having two or more systems is a solution to this problem, but that can present difficulties due to the cost and the space needed for multiple systems. Eventually the latter problem, and perhaps the former as well, may be solved with the development of a single handheld piece capable of switching between multiple wavelengths.
The requirement for multiple sources will not be going away due to the varied tissues in the body, noted the University of Florida’s Low. “A laser is not a laser is not a laser. It’s all dependent upon the wavelength, because that is related to the target,” he said.