Medical lasers are making rapid progress in numerous new applications including drug delivery, oncology, gene therapy, nerve repair and dentistry.
It started with mouse hairs. In 1967, Dr. Endre Mester of Semmelweis Medical University in Budapest, Hungary, recognized that a low-power ruby laser could stimulate faster hair regrowth in mice. Since then, lasers have increasingly become an important instrument in the physician’s toolbox.
Today, research is advancing toward the use of lasers to diagnose and treat a plethora of conditions. Recent rapid technological developments in lasers have contributed to their safe and effective use in surgical settings, aesthetic treatments, ophthalmology, oncology, cardiology and many other biomedical applications, including veterinary settings. Growth in cosmetic laser treatments is nothing short of booming: Sales of laser-based instrumentation in the medical and aesthetic sector increased 11 percent from 2012 to 2013 to $682 million, and another 10 percent increase is expected in 2014, to $746 million globally, according to The Worldwide Market for Lasers, a report released in January by Strategies Unlimited.
Lasers’ efficiency, safety and precision are the drivers behind this growth. In surgical applications, medical lasers are more precise than conventional surgical scalpels, and therefore cause less damage to surrounding tissue. Although systems are expensive and operators of medical lasers require special training, the advantages of reduced pain, bleeding, swelling and scarring are compelling enough to justify their widespread adoption.
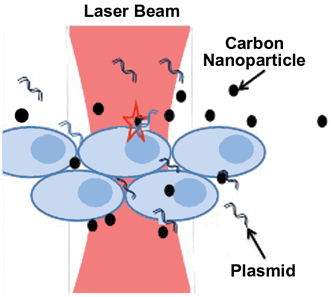
A CW near-IR laser beam directed at diseased cells mediates photothermal delivery of crystalline magnetic carbon nanoparticles with plasmids, drugs or impermeable dyes. Courtesy of S. Mohanty/University of Texas at Arlington.
Much current cutting-edge research is focused on biophysical and physiological studies at the molecular and cellular level, and on lasers’ effects on whole organisms. A group at the University of Texas at Arlington, led by assistant professor of physics Dr. Samarendra Mohanty, has used low-power near-IR lasers and crystalline magnetic carbon nanoparticles (CNPs) to perform photothermal delivery of impermeable dyes and plasmids (self-replicating DNA molecules) into live human prostate cancer (PC3) cells (Scientific Reports, doi: 10.1038/srep05106). The noninvasive technique involves directing a CW Ti:sapphire laser at 800 nm toward the cancer cells in the presence of plasmids and CNPs measuring 5-10 nm. The heat causes the CNPs to stretch the cell membranes and increase fluid flow to allow exogenous substances (plasmids, for example, or an agent that kills the cancer) to be delivered.
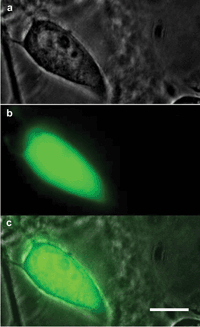
(a) A bright-field image of a live human prostate cancer (PC3) cell, (b) yellow fluorescent protein (YFP) fluorescence in same PC3 cell, and (c) the PC3 cell transfected with ChR2-YFP plasmids using photothermal delivery. Scale bar: 10 μm. Courtesy of S. Mohanty/University of Texas at Arlington.
This technique used a low laser power of <50 mW for up to 20 s of exposure time. In previous work, the group applied higher laser powers (50-100 mW, over time periods of <1-2 s) in the presence of Fe-doped CNPs to actually kill the cancer cells without injury to healthy cells, demonstrating the method’s efficacy (Journal of Biomedical Optics, doi:10.1117/1.JBO.17.1.018003). Compared with pulsed lasers, CW near-IR (diode) lasers are compact, easy to use and less expensive, suggesting that the technique is a promising approach to photothermal therapy of cancer cells.
“This technology is an important development toward controllable in vivo drug, vaccine and gene delivery,” Mohanty said. “It could someday enable label-free diagnostics with therapeutic potential in optogenetics, cancer and many other diseases.”
Laser therapy is one of several emerging medical and veterinary techniques using high-intensity light to stimulate cellular function in tissue, or to shrink and destroy tumors and precancerous growths. Doctors can direct laser therapy on the surface of a body, or use it to reach where conventional surgical techniques can’t, via a flexible fiber optic endoscope inserted through the mouth, nose, colon or vagina.
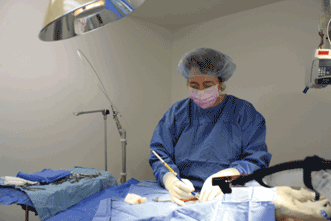
Veterinary surgeon Dr. Laura Remsen uses the Aesculight flexible waveguide CO2 laser system on a canine patient. The Aesculight Class IV laser therapy is a surgery-free, drug-free, noninvasive treatment for pain and inflammation post-surgery, as well as for many chronic and acute conditions such as wounds, infections, sprains, strains, fractures, tooth extraction and arthritis. Courtesy of Animal Care Center in Fernley, Nev.
Photodynamic therapy is another laser therapy approach that activates an applied photosensitive agent that kills only the cancer cells.
The most common types of lasers used to treat cancer are carbon dioxide (CO2), argon and Nd:YAG lasers (Dental Materials, doi:10.1016/j.dental.2014.02.006). Argon and CO2 lasers can cut the skin’s surface to remove superficial cancers of the skin, while Nd:YAG lasers are more commonly applied through an endoscope to reach internal organs, such as the uterus, esophagus or colon. Although laser therapy techniques are FDA approved, researchers are still performing clinical trials and gathering long-term data to determine their role in treating cancers of the brain, breast and prostate.
Low-level laser therapy (LLLT) is one technique in development that uses low-intensity lasers to treat cancer, degeneration, stroke and other conditions. Most LLLT in animals and patients is limited to red and near-IR light at 600-1100 nm; live tissue scatters light at shorter wavelengths and water absorbs too much at wavelengths beyond 1100 nm. Many LLLT devices are Class 3B lasers or LEDs, though some are defocused Class 4 lasers. In most cases, the devices emit divergent beams (uncollimated), delivered with typical irradiance of 5 mW/cm2 to 5 W/cm2 and low power range of 1 mW to 10 W. Delivery can be pulsed or sometimes continuous, with typical treatment time of 30 to 60 s per treatment point.
Recent medical research theorizes that the mechanism of low-level laser therapy is primarily via the absorption of light within mitochondria, the numerous “power plants” within cells that convert the oxygen and pyruvate from food into cellular energy via adenosine triphosphate (ATP). As it happens, cytochrome C oxidase, a critical protein involved in the regulation of mitochondrial activity, is a photoacceptor of light in the near- to far-IR. At the cellular level, LLLT displaces nitric oxide from the respiratory chain to increase levels of ATP and reactive oxygen species. The deep-tissue application of laser or LED devices in LLLT techniques may work via this mitochondrial mechanism to promote tissue repair, reduce inflammation and induce analgesia, according to James Carroll, medical researcher, and founder and CEO of Thor Photomedicine in Chesham, England.
Nerve treatment and tooth regeneration in dental and veterinary contexts is a focus of interest in current LLLT research. In February 2014, Carroll and colleagues at the University of Birmingham in England reviewed related dental/orofacial research and found that of 153 papers and studies, 130 of them reported a positive effect in terms of pain relief, healing time or other symptom improvements; 23 reported inconclusive or negative results. The team concluded that direct application of low-power therapeutic light in the oral cavity (as opposed to photodynamic therapies) should be safe and reliable for pain relief in dentistry, as it has been found to be in other health care fields.
Clinical investigator Dr. Praveen Arany and colleagues at Harvard University’s School of Engineering and Applied Sciences have found supporting evidence for this conclusion. The group applied low-power, continuous-wave near-IR laser light (an 810-nm GaAlAs diode with varied power, spot size and distance) to the tooth pulp of treated rats’ teeth and found that this stimulated new growth of dentin, the bonelike substance in teeth (Science Translational Medicine, doi: 10.1126/scitranslmed.3008234).
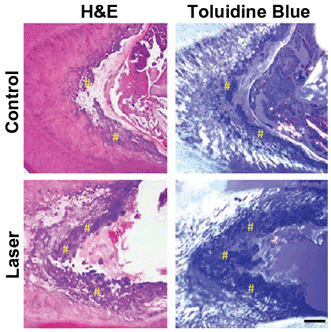
Low-power laser treatment of the exposed pulp in the molar of a rat induces tertiary dentin in a rodent model. H&E = hematoxylin and eosin, used for histological analysis of decalcified teeth. Courtesy of Harvard’s Wyss Institute and SEAS.
The mechanism, the researchers said, is the inducement of reactive oxygen species to activate latent transforming growth factor β1 (TGF-β1), which is capable of differentiating human dental stem cells in vitro. They concluded that the laser light already used in dental procedures may encourage tooth regeneration. In fact, researchers agree that LLLT is a safe, effective treatment to enhance healing and tissue remodeling while reducing inflammation and analgesia in a wide range of oral pathologies. Furthermore, the drug-free technique appears to be efficacious where many current pharmaceuticals are not.
Progress is visible on the clinical side as promising devices near commercial practicality. In August 2013, the FDA cleared the first CO2 laser system for use in “pain free” hard and soft tissue ablation for dentistry. Built by system developer Convergent Dental of Natick, Mass., the Solea laser system operates noiselessly without the vibration of a dental drill and eliminates 95 percent of anesthesia and needles. Unlike conventional CO2 lasers centered at 10.6 µm, the Solea laser source is based on an oxygen 18 isotope that lases at 9.3 µm, matching the peak absorption of hydroxyapatite, a mineral found in teeth and used in dental implants. In May, Convergent Dental appointed Cogmedix of Worcester, Mass., to be its contract manufacturer.
Pilot studies using LumiThera’s prototype laser system will investigate a multiwavelength LLLT approach to slow the progression of dry age-related macular degeneration. Courtesy of LumiThera.
In 2012, researchers at the Institute of Ophthalmology at University College London applied LLLT to eye disease. Researcher Dr. Rana Begum and colleagues found that when the retinas of aged mice were exposed to five 90-s exposures of 670-nm light over 35 hours, key inflammatory markers in the mitochondrial membrane were significantly reduced (Neurobiology of Aging, doi:10.1016/j.neurobiolaging.2012.04.014).
Development-stage medical device company LumiThera (Poulsbo, Wash.) cites the article on its website, along with many others that provide evidence that light can be used to treat eye conditions such as age-related macular degeneration, retinitis pigmentosa, diabetic macular edema and others. In April, LumiThera was awarded a $250,000 Washington State Life Sciences Discovery grant to develop a proof-of-concept LED system for treatment for ocular disorders and disease. The company will use the grant to build the unique multiwavelength device and pursue pilot studies of light-scatter profiling in the eye. The hope is that, someday, the noninvasive approach may help to slow the progression of dry age-related macular degeneration, according to founder and CEO Clark Tedford.