Raman spectroscopy, chip-based technology, and AI together enable label-free detection of disease characteristics, tracking of immune response, and identification of a disease’s antibiotic resistance.
KARINA WEBER AND JÜRGEN POPP, LEIBNIZ INSTITUTE OF PHOTONIC TECHNOLOGY
Millions of people worldwide die from infectious diseases each year, and the spread of these diseases poses a real threat to the survival of public health systems. How quickly health care institutions can be overburdened when an infection rapidly spreads was once again made clear during the current pandemic triggered by the SARS-CoV-2 virus. In addition, the sharp increase in the number of multidrug-resistant pathogens often makes it difficult to effectively treat patients with pharmaceuticals. Noninvasive optical technologies such as Raman spectroscopy could hold the key to quick diagnoses and tailored patient treatment, helping to stop the spread of contagious diseases.

A demonstrator of a RamanBioAssay chip with 20 reaction chambers that enables the measurement of four types of antibiotics, each with a different concentration. Courtesy of Leibniz Institute of Photonic Technology.
In a world facing pandemics, a growing need exists for inexpensive, fast, sustainably produced, and easy-to-adjust point-of-care diagnostic devices. The integration of noninvasive photonic methods into bioanalytical chip-based instrumentation offers great potential to fulfill the aforementioned needs. To enable the timely transfer of ideas from the research laboratory to commercialized medical products, open user platforms are needed that bring together the expertise of renowned players from science and industry to create an efficient flow of information. For the sake of further innovation, it is important to follow the road from the creation of a research idea — in this case, utilizing molecular spectroscopy as a powerful approach for point-of-care infection diagnosis — to its practical application in a medical device.
The potential of Raman
Recent research has shown that optical technologies in general, and molecular spectroscopic methods in particular, offer enormous potential as fast, nondestructive, and label-free approaches for biomedical analysis. Rapid advancements in the development of instrumentation built around these techniques, the use of artificial intelligence (AI) to gather and interpret data, and increased dialogue among technologists, spectroscopists, and end users have triggered the growing use of molecular spectroscopy. This is particularly true in medical diagnostics and the development of assays for point-of-care or point-of-need applications.
In the life sciences and medicine, Raman-based technologies increasingly complement the use of established methods such as fluorescence spectroscopy and microscopy. Raman spectroscopy enables the label-free detection of the molecular composition and morphology of complex samples such as biological cells and tissues, while requiring little or no sample preparation. The Raman spectrum consists of many dozens of independent parameters ranging from concentration measurement to the three-dimensional arrangement of macromolecules and biopolymers in biological samples, providing a map of all of the chemical information in these samples.
The Raman effect was discovered 94 years ago, when C.V. Raman showed that when matter interacts with light, photons are inelastically scattered. Raman spectroscopy has only been able to fully develop its great potential in the last 10 to 20 years, however, thanks to technical innovations. This renaissance of Raman spectroscopy has been triggered primarily by major advancements in laser technology, such as the miniaturization of lasers and various other light sources, the design of efficient filters that block out elastically scattered Rayleigh light, and the development of extremely sensitive detectors. In addition to these advancements, the success of Raman spectroscopy is also intrinsically linked to achievements in the field of AI.
As Raman spectroscopy has moved forward, the interdisciplinary dialogue between spectroscopists and the end users of their systems, such as clinicians, has also increased. This has accelerated the application of Raman spectroscopy and its variants in new biomedical realms. For example, the data that the technique reveals enables the noninvasive morphochemical characterization of a wide range of biological samples, from prokaryotic and eukaryotic cells, fungi, and biofilms to tissue sections and whole organs. In this way, Raman studies have provided insights about disease mechanisms for the early diagnosis of illnesses.
For the purposes of this article, the focus will be placed on the application
of Raman spectroscopy for infectious-disease diagnostics.
Reality in the clinic
The following is a typical situation that occurs in a doctor’s office: A patient with a fever or other typical symptoms of infection comes into the office. After a short anamnesis (medical history) is obtained and an exam is given, the physician decides that the patient’s infection is likely caused by bacteria and prescribes an antibiotic.
It may be asked why — that is, on what basis — did the physician identify the illness as a bacterial infection? Could it instead be a viral or fungal infection? Furthermore, it is unknown whether the prescribed antibiotic will be effective in fighting the supposed infection-causing bacterial pathogen or whether the pathogen will be resistant to it.
Nowadays, the global, rapid, and, in some cases, uncontrolled spread of novel pathogens, along with a steady increase in antibiotic resistance, poses major challenges for health care systems worldwide. To cope with these threats, fast and innovative diagnostic solutions that enable speedy and targeted treatment must be developed.
Researchers in the field of Raman spectroscopy have shown in recent years that the modality offers the potential to successfully address unmet needs in infectiology. These needs include rapidly determining the host response, quickly detecting pathogens without needing to perform time-consuming cultivation steps, and detecting antibiotic resistances using a point-of-care approach (Figure 1).
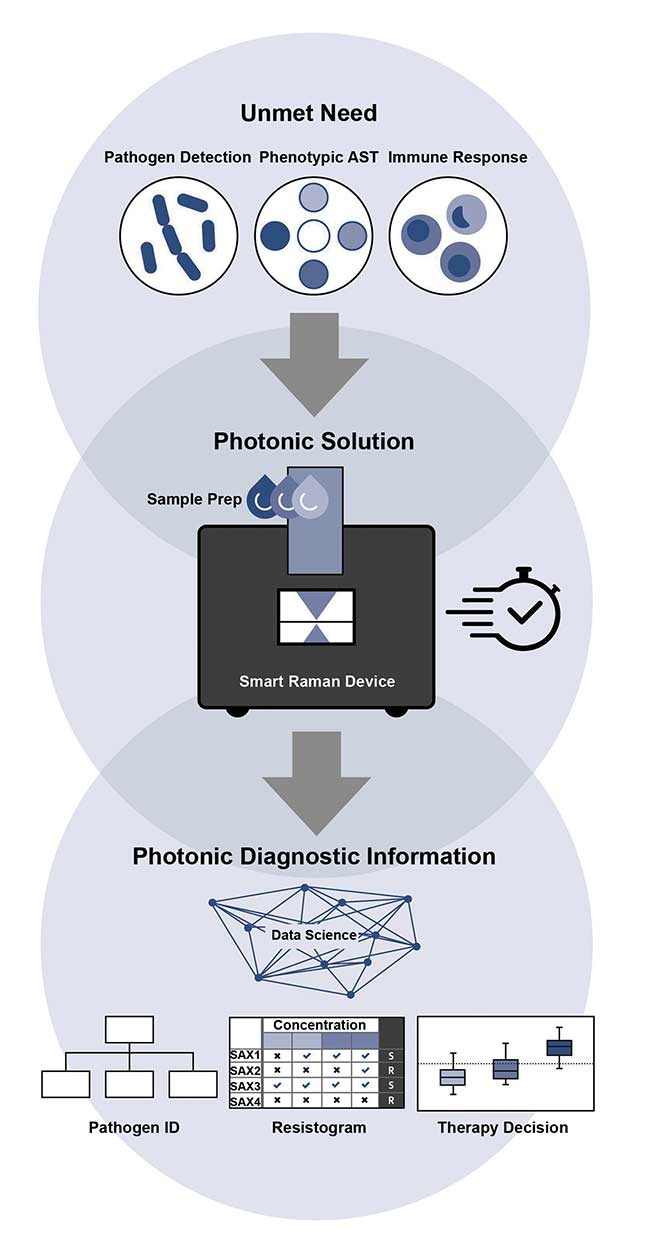
Figure 1. A schematic representation of cell-based Raman assays for infection diagnostics.
AST: antimicrobial susceptibility testing. Courtesy of Leibniz Institute of Photonic Technology.
Determining the host response
The presence of immune cells helps to determine whether the patient is suffering from an infection. Leukocytes, for example, are an important part of the immune system’s defense against pathogens such as bacteria or viruses. In this context, the activation state of leukocytes (the release of inflammatory molecules) can reveal information about both the pathogen and the patient’s specific immune response to it, in order to quickly detect possible dysregulation. Therefore, research is ongoing to ascertain whether leukocytes are the key to fast and efficient monitoring of infections.
Raman spectroscopy offers great potential for quick immune cell characterization in terms of monitoring the activation state of leukocytes, which can enable rapid diagnoses and differentiation of infections, as well as indicate the prognosis of patients with infections. Studies have shown that Raman spectroscopy can be used to identify the major leukocyte subtypes — that is, to differentiate among neutrophils, lymphocytes, and monocytes1. These studies confirm that pathogen-specific activation can be detected by the Raman technique2. In one study, the Raman spectroscopic analysis of an in vitro model of isolated neutrophils from human peripheral blood allowed for discrimination between infected and noninfected neutrophiles with 92% accuracy. The model was stimulated with heat-inactivated gram-positive (lacking an outer membrane) and gram-negative (surrounded by an outer membrane) bacteria.
Studies of neutrophils that have been activated due to infection have revealed that it is possible to distinguish the immune system’s response to fungal infection (simulated with Candida albicans) from a bacterial infection with 92% accuracy. In addition, neutrophils stimulated by gram-positive bacteria (Staphylococcus aureus) could be separated from those stimulated by gram-negative bacteria (Escherichia coli) with an accuracy of 84%3.
In a recently published clinical study — involving both the University Hospital Jena in Germany and the University Hospital Attikon in Athens, Greece — it was shown that the analysis of the Raman spectroscopic fingerprints of leukocytes from patients’ blood successfully distinguished between inflammation, infection, and sepsis. This study, which showed the potential of the technique to generate a label-free hemogram, is part of the European project titled HemoSpec (Figure 2)3. The project combines three technologies: automated microfluidic sample handling with integrated holographic blood count, simultaneous multiplex fluorescence biomarker sensing, and detailed Raman spectroscopic leukocyte characterization.
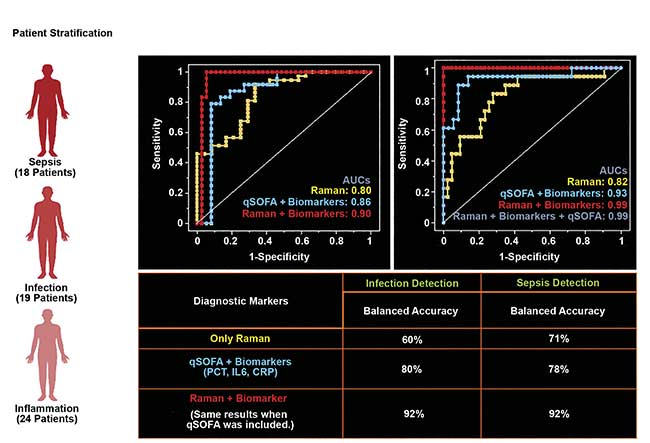
Figure 2. A receiver operating characteristic curve showing diagnostic efficiency. Raman spectroscopic characterization of the host response was demonstrated in the Phase II clinical trial of the HemoSpec project, which enabled discrimination between inflammation, infection, and sepsis in hospitalized patients based on the molecular signatures of leukocytes from blood. Courtesy of Leibniz Institute of Photonic Technology.
By fully automating the process chain — cell detection, Raman spectra acquisition, and chemometric analysis — it is possible to analyze a large number of cells (as many as 1000) in a timescale of 30 min with only minimal sample preparation. The combination of such a high-throughput Raman cell platform and the knowledge gathered from the aforementioned Raman host response studies presents the opportunity for new avenues to be opened for clinical diagnostic applications in terms of timely personalized therapy.
Tailored therapy
Once laboratory tests determine that a patient is suffering from a bacterial infection, to treat it successfully, the physician must find out as quickly as possible the type of bacteria that caused the infection, as well as the antibiotics that are resistant to that particular bacteria. Medical diagnostics labs that economically cover the testing of the entire range of pathogens and resistances currently often use culture-based methods. Thus, the results for pathogen identification and resistance profiles are often not available for at least 24 h, but more typically take three days, which doesn’t allow for timely treatment.
Clinicians often initially treat patients empirically (based on experience), prescribing a broad-spectrum antibiotic. They sometimes even prescribe reserve antibiotics, which are restricted for use with specific conditions. Because of increasing antibiotic resistance, however, it is essential to strive for an effective targeted treatment that relies on a rapid and accurate characterization of a specific pathogen and its resistance profile before therapy begins.
To address this need, the Leibniz Institute of Photonic Technology (Leibniz-IPHT), in close cooperation with the University Hospital Jena, developed the RamanBioAssay — an approach that enables quick identification of pathogenic agents and their antibiotic resistance, as well as determination of the minimum inhibitory concentration of an antibiotic (Figure 3). This approach drastically re- duces the time to diagnosis to 2 to 3.5 h. It requires only a small number of microbial pathogens because a very small sample size of only a few hundred bacteria is sufficient, as opposed to the larger sample size required in other forms of analysis. This method can clearly identify pathogens and determine their antibiotic resistance, without the need to perform a prior cultivation step4.

Figure 3. The high-throughput Raman setup at the University Hospital Jena. Courtesy of Leibniz Institute of Photonic Technology.
Based on the information that the method provides, physicians can specifically tailor a therapeutic antibiotic treatment to the identified pathogen. The RamanBioAssay uses a combination of chip-based Raman microspectroscopy and classical imaging. An example of a chip surface on which an assay is performed is shown in the first image. The intelligent use of laser light in a Raman setup, in combination with a light microscope, enables the label-free, nondestructive, and culture-independent optical and spectroscopic characterization and identification of bacteria down to the level of individual cells. Statistical evaluation algorithms, as well as the use of AI methods, enable the automatic classification and identification of bacteria and their antibiotic resistance. And with the integration of chip-based methods in miniaturized Raman setups, the entire process chain is covered5.
Customized AI
The success of the approach is inextricably linked to the development of customized algorithms and machine learning methods for translating Raman measurement data into information that is qualitatively and quantitatively usable by the end user — in this case, medical doctors6. Data analysis software needs to provide reliable analysis of the Raman data in a form that can be easily understood by anyone seeking diagnostic information. One example that has been created is called RAMANMETRIX, based on customized AI. For optimal use, the software system must combine chemometric and machine learning techniques to provide a complete and detailed overview of Raman data.
When machine learning is applied in the process of extracting this data, it must take all aspects of the Raman analysis into account, including pretreatment and preprocessing protocols, spike correction and calibration, baseline correction, and normalization tools. And the interface must be understandable and usable for anyone in a corporate or research setting (Figure 4).
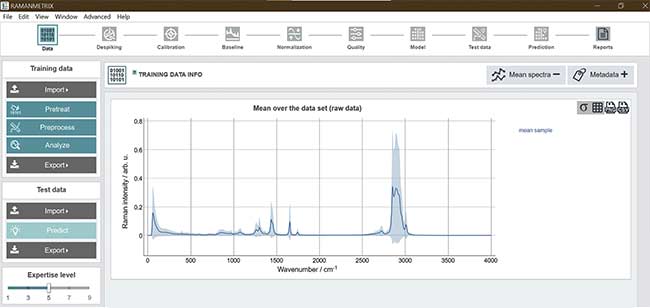
Figure 4. A screenshot of the RAMANMETRIX software solution, which provides a complete data processing pipeline within a user-friendly graphical interface. Courtesy of Leibniz Institute of Photonic Technology.
Innovative photonic tools, such as a point-of-care device for infectiology, could be very valuable in medical applications. A current major hurdle, however, is the ability to realize the rapid translation of such promising methods into clinical and medical practice applications. How can academia and industry help good ideas evolve from proof of concept into products, rather than have such ideas end up in the limbo of incomplete clinical translation?
Photonics brought to life
To bring these recent advancements to the patient more quickly, novel infrastructures that are open to a variety of users are needed. One such form of infrastructure currently being built up is the Leibniz Centre for Photonics in Infection Research, which is designed to open up new ways to develop market-ready light-based diagnostic technologies and novel therapeutic approaches for treating infectious diseases. As a translational center, it is financially supported by the German Federal Ministry of Education and Research and will be grounded in a systemic approach that allows ideas for the light-based diagnosis and therapy of infectious diseases to be further developed, tested, and rapidly brought to market maturity. As a globally unique infrastructure, the center thus bridges the gap between research results and the market launch of solutions for physicians and patients.
The center is being built by Leibniz-IPHT, Leibniz Institute for Natural Product Research and Infection Biology Hans Knöll Institute, Friedrich Schiller University Jena, and the University Hospital Jena.
The infrastructure provided by the collaboration will include all the steps necessary for product development — from validation via analysis of real patient samples to professional support in product design and small series production. Resources to help with implementing standard procedures and understanding the relevant legal regulations will be available. Industry and authorities must be involved from the beginning to ensure smooth market entry of new diagnostic procedures and therapeutic approaches.
Acknowledgments
The authors gratefully acknowledge the financial support of the European Union, the Thüringer Ministerium für Wirtschaft, Wissenschaft und Digitale Gesellschaft, the Thüringer Aufbaubank, Germany’s Federal Ministry of Education and Research, the German Science Foundation, the Fonds der Chemischen Industrie, and the Carl Zeiss Foundation.
Meet the authors
Karina Weber studied biotechnology at the University of Applied Sciences Jena, followed by postgraduate study in chemical and process engineering at the Clausthal University of Technology. In 2007, she became a postdoctoral student in professor Jürgen Popp’s group at the Institute of Physical Chemistry at the University of Jena and Leibniz-IPHT. Since 2018 she has been deputy head of Popp’s Spectroscopy and Imaging department and also consultant of the executive board at Leibniz-IPHT. Her research focuses on smart molecular biological tools, as well as on spectroscopic analytical tools that cover the entire analysis chain for on-site and point-of-care testing for medical and life science applications; email: [email protected].
Jürgen Popp studied chemistry at the University of Erlangen-Nuremberg and the University of Würzburg. Since 2002, he has been a chair of physical chemistry at the Friedrich-Schiller University Jena, and in 2006 he became scientific director of Leibniz-IPHT. His core research focus is biophotonics — in particular, the development and application of frequency-, time-, and spatially resolved innovative laser microspectroscopical methods and techniques for biomedical diagnostics, as well as environmental and food analysis; email: [email protected].
References
1. I.W. Schie et al. (2018). High-throughput screening Raman spectroscopy platform for label-free cellomics. Anal Chem, Vol. 90, pp. 2023-2030.
2. N. Arend et al. (2020). Detection and differentiation of bacterial and fungal infection of neutrophils from peripheral blood using Raman spectroscopy. Anal Chem, Vol. 92, pp. 10560-10568.
3. A. Ramoji et al. (2021). Leukocyte activation profile assessed by Raman spectroscopy helps diagnosing infection and sepsis. Crit Care Explor, Vol. 3, No. 5, p. e0394, www.doi.org/10.1097/cce.0000000000000394.
4. J. Kirchhoff et al. (2018). Simple ciprofloxacin resistance test and of minimal inhibitory concentration within 2 h using Raman spectroscopy. Anal Chem, Vol. 90, No. 3, pp. 1811-1818, www.doi.org/10.1021/acs.analchem.7b03800.
5. A. Tannert et al. (2019). Phenotypic antibiotic susceptibility testing of pathogenic bacteria using photonic readout methods: recent achievements and impact. Appl Microbiol Biotechnol, Vol. 103, No. 2, pp. 549-566, www.doi.org/10.1007/s00253-018-9505-4.
6. S. Guo et al. (2021). Chemometric analysis in Raman spectroscopy from experimental design to machine learning-based modeling. Nat Protoc, Vol. 16, No. 12, pp. 5426-5459, www.doi.org/10.1038/s41596-021-00620-3.