Rhonda Johnston, a nurse practitioner,
has a simple requirement when it comes to the technology that allows her to serve
patients scattered across southern Colorado: “Our goal is to make sure the
telehealth patient encounter is no different than a traditional encounter.”
If that can be accomplished, she said, “telehealth can be
a very useful tool.”
Also known as telemedicine, the practice of interacting with patients
at a distance is being implemented to serve remote clinics and to teach urban populations
healthy practices. Companies are turning to it instead of sending employees on a
trip halfway around the globe to see a doctor.
In the future, you might be able to see a doctor virtually anywhere
– and that capability won’t be confined to the developed world. In part
that’s because the Seattle-based Bill & Melinda Gates Foundation is funding
the creation of low-cost cell phone-based telehealth applications.
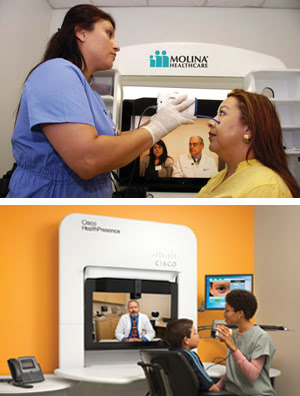
In telehealth, the doctor need not be present, but a nurse or other skilled person
must be. Continued instrumentation advances may someday make it possible for patients
to do their own exams. Courtesy of Cisco Systems and Molina Healthcare.
Powering these actual and possible uses are advances in photonics-based
imaging, displays and instrumentation. However, the field still faces technical,
regulatory and economic hurdles.
A whole host of issues have already been successfully addressed.
For example, Johnston – a director of education and training for clinical
video telehealth in the Washington-based Department of Veterans Affairs (VA) Office
of Telehealth Services – has seen enormous strides made since she started
using the technology in 1995. In particular, she cited the advent of high-definition
cameras and displays.
“It’s better than I can see face-to-face,” she
said.
There have also been instrumentation advances. On the horizon
are ultrasound imaging wands, which could largely replace the need for touch.
At present, there must still be a skilled operator on the patient
end to work the equipment. In Johnston’s case, this is done with a registered
nurse trained in advanced assessment.
Making the distance between patient and provider disappear can
require a mix of approaches, said Jeffrey R. Lowe, care coordination and telehealth
manager for the Veterans Integrated Service Network 19 (VISN 19). Spanning Colorado,
Utah, Wyoming, Montana and parts of surrounding states, the Glendale, Colo.-headquartered
VISN 19 was the first in the VA network to launch telehealth primary care.
Lowe said that telehealth falls into three broad categories. There
are low-bandwidth applications running over standard telephone lines, with data
rates in the tens of kilobits per second. One use might be in-home monitoring. An
example of the second category might be telehealth video conferencing, requiring
about a megabit-per-second bandwidth. Finally, there is store-and-forward telehealth,
where images are captured and transmitted for later review.

Using store-and-forward technology, at-a-distance medical consultations can be done over
slower channels and efficiently at a time more convenient for both provider and
patient. Courtesy of Peter Yellowlees, UC Davis.
These approaches save hours of travel many times a year for just
fewer than 18,000 VISN 19 patients. The goal is to grow that number by 30 percent
in the coming year.
In the future, Lowe expects to see higher-quality imaging but
not exotic hardware. “What we historically have done is use a commercially
available off-the-shelf camera with a high number of pixels,” he said.
One new hardware twist that VISN 19 is deploying in 60 sites is
a patient telehealth cart. These mobile setups allow video conferencing and the
capture of still images.
Scottsdale, Ariz.-based GlobalMedia, a private firm, supplies
some of these carts. Communications manager Roger Downey said that the company makes
a variety of carts for different medical disciplines. Typically they have two cameras,
one for the big picture and the other for fine work. They also may have a mix of
visible and ultraviolet lights.
Downey said that GlobalMedia’s products offer a unique one-button
approach for visible still images sent to a patient’s electronic medical records.
The difference isn’t in the imaging but in what happens to the local copy
of the transmitted data, a process that is compatible with the privacy provisions
of HIPAA, the Health Insurance Portability and Accountability Act of 1996.
“That one-button click would also remove every image remnant
from the original computer, which makes it very HIPAA-compliant,” Downey explained.
Other players in the telemedicine market include large companies
like Cisco Systems of San Jose, Calif., and a host of smaller ones, like startup
NuPhysicia of Houston and Boston-based American Well.
What they all hope to do is to tap into what the London-based
consultancy Ovum, a Datamonitor company, predicts will be a $6.7 billion North American
telehealth market in 2012. That figure includes equipment, software and services.
The total is up nearly tenfold from the $693 million spent in 2006.
In general, said Ovum senior health care technology analyst Cornelia
Wels-Maug, telehealth is well suited to cases where the distances between provider
and patient are great. Thus, Canada, the western US, Scandinavia and Australia are
prime potential targets.
However, the practice extends well beyond those initial markets,
in part because doing so pays dividends. “Research indicates there is a cost
benefit,” Wels-Maug said.
She cautioned that these studies are limited. Thus, the savings
may not materialize.
There is some evidence, though, that payoff may be real. Take
the case of Cisco, a provider and consumer of telemedicine technology. In March,
the company launched its own care-at-a-distance platform. It combines high-definition
cameras; an otoscope to image the inside of the eyes, ears and nose; and devices
to capture vital signs.
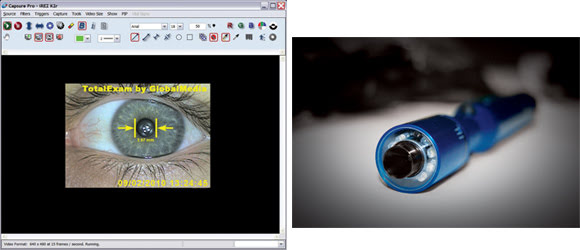
High-definition video devices (right) and other imaging innovations
allow doctors to see and treat distant patients as if they were physically present
(left). Courtesy of GlobalMedia.
The company runs a health and wellness clinic at its California
headquarters to serve the thousands of employees there. The same approach, though,
won’t work for other company locations, said Nick Augustinos, leader of Cisco’s
global health care solutions group. Those sites don’t have enough people.
So Cisco is using its own technology to make its California primary
care clinic available to workers in North Carolina and elsewhere. Telemedicine technology,
Augustinos said, offers “… the ability to establish a medical practice
and deliver care in a very cost effective way and do it in areas that otherwise
you wouldn’t have been able to.”
This model could be used elsewhere. Cisco, for example, is working
to deploy its technology in retail chains, potentially offering health care at more
convenient times and in nontraditional places.
The company’s platform is being used by Molina Healthcare
of Long Beach, Calif. Molina provides Medicaid-related solutions to meet the needs
of low-income families and individuals. It also assists state agencies in the administration
of Medicaid. About 1.5 million members in nine states are in its licensed health
plans.
Dr. Rafael Amaro, the company’s medical director, said Molina
is using the donated telehealth technology at three sites for health care education,
such as teaching diabetics how to check blood sugar and maintain it at a proper
level. Doing so will avoid problems – and costs – down the road.
Molina might eventually seek to improve the efficiency of its
health care delivery. One telemedicine application might be a remote retinal exam
for diabetics, an area known to need improvement. Patients would have their eyes
scanned, with the collected data reviewed elsewhere.
“It’s transmitted to an ophthalmologist who’s
at a desk with a nice big screen and looking at the backs of the eyes, maybe doing
30, 40, 50 patients, one right after the other,” Amaro said.
Physicals, diagnosis of ailments such as pains in the lower back,
blood chemistry tests and other remote ambulatory care are offered by NuPhysicia,
said company president Glenn Hammack. Clients include firms operating oil rigs around
the world.
Some of the nontechnical issues confronting telemedicine providers
involve reimbursement and regulation. With regard to the former, telemedicine expenses
often are reimbursed by insurance companies only if the patient lives in an underserved
area. As for regulation, NuPhysicia has subsidiaries in Brazil and Malaysia because
their governments mandate that oil rigs in their jurisdictions be served by local
providers.
On the technology side, Hammack noted that his company’s
offerings make use of one- or three-chip CCD cameras. One of the keys to further
expansion of telemedicine lies in sensor improvements, including such photonics-based
instruments as microspectrophotometers.
These can be particularly useful for small-sample on-site blood
analysis, Hammack said. “Instead of having to transit that sample to a central
facility and then wait one or two days for the results, the continued progress of
point-of-care testing provides equivalent results in minutes.”
Further improvements in such sensors are vital. Also important
is the development of systems that are easier for unskilled people to use, Hammack
noted.
The need for technology that is easier to operate was something
mentioned also by Peter Yellowlees, a professor of psychiatry and director of health
informatics at the University of California, Davis, a telehealth research leader.
Yellowlees himself has been doing video consultations as part
of his psychiatric practice for nearly 20 years. He said that providers sometimes
struggle with complex systems, particularly if the separate parts are not well integrated.
As for the future, he sees mobile devices as playing a big role. There already are smartphone applications that monitor women in pregnancy. Two-way
mobile video conferencing is now possible. Ongoing improvements could put medical
care in the palm of one’s hand, provided that security and privacy issues
are dealt with.
“At the moment, most are not HIPAA-compliant,” Yellowlees
said of Internet and cell phone two-way video communications. “It’s
not secure enough, in other words, for health care.”