A more compact and portable design, achieved by separating the interferometer and light source from the spectrometer, may soon enable clinical uses beyond ophthalmology.
McKenzie Peterson, Lumedica Vision Inc.
Optical coherence tomography (OCT), a noninvasive imaging technology, is a standard diagnostic tool used in the field of ophthalmology. With the advent of new compact form factors for the modality, as well as the assistance of artificial intelligence (AI) and other software innovations, OCT could be put to use in other clinical settings, such as optometry and family medicine. These and other specialties are taking notice of OCT’s capacity to provide high-resolution cross-sectional images without the adverse effects of radiation or surgical incisions for the examination of tissue. Thanks to reconfigured and miniaturized components, as well as user-friendly interfaces, mobile clinics could reap the benefits of utilizing an accessible, easy-to-use OCT system.
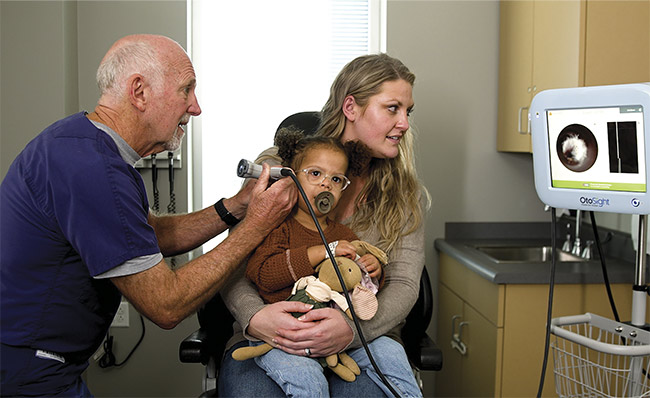
Unlike its OCT predecessors, the OtoSight Middle Ear Scope generates a rolling A-scan in real time to provide a depth-over-time assessment.
The device is housed on a freestanding rolling cart for easy access and mobility within the exam room. Courtesy of PhotonicCare.
The advent of OCT
The first recorded successful application of OCT was the imaging of an in vivo human retina by Eric A. Swanson and colleagues in 1993. The technology was ultimately commercialized in 2005 as a means for ophthalmologists to provide a noninvasive window into the delicate layers of the retina at the resolution required to monitor sight-threatening diseases. The technique has proved to be indispensable to retinal specialists and ophthalmologists, as well as for in vivo cardiovascular imaging. By the 2010s, however, access to OCT was still largely reserved for specialists and well-funded research. Recent innovation has enabled the development of novel point-of-care systems for generalists and practitioners of new medical specialties.
As an inspection tool, OCT has found a role in a variety of nonmedical fields such as food inspection and quality control. Essentially, any transparent or translucent sample with critical features on the micron scale is well suited for fast, nondestructive optical inspection. The human eye, as a natural system made to take in light, has historically been an ideal candidate for OCT inspection. Improvements to ophthalmic OCT systems have occurred in parallel with the development of new medical OCT devices for other parts of the human body. In health care diagnostics, the goal of OCT is to produce images to inform medical decision-making. Cost, however, plays a factor in which end users get access to OCT.
New design
Point-of-care imaging brings the technology to the patient at the moment of need or diagnosis. But bulky, expensive OCT systems, which often require their own room and are largely available only in specialists’ offices, have been inaccessible to many patients worldwide. Many glaucoma cases remain undiagnosed for years and are diagnosed only when a patient visits a specialist who has an OCT system. Unfortunately, any damage done to the eye by glaucoma during this time is irreparable.
The pandemic has added to the backlog of eye diseases not getting diagnosed. As patients emerged from lockdown, health providers saw clinics flooded with overdue appointments and new patients. In many countries — including the U.S., China, and Japan — an aging population also contributes to the rising number of people needing eye care.
With clinic space and clinicians’ time at a premium, providers need to consider the most efficient ways to spend their money. Having a compact OCT diagnostic device in every exam room at a clinic or doctor’s office would decrease the time a patient spends waiting to be examined and would increase the number of patients a provider can see during a scheduled hour. To enable such availability, and to increase the ability for multiple personnel to use the devices, clinical OCT requires a low-cost, compact design with an emphasis on simple functionality.
To achieve these requirements, optical engineers have considered various ways in which they could configure the basic components an OCT device. To make the design more compact, researchers rearranged the Michelson low-coherence interferometer, the basis of OCT, into smaller packages. In the first clinical application of this newly conceived low-cost OCT system, researchers moved the light source, reference arm, and sample arm to the scanner1. In this configuration, only the spectrometer and a computer were housed in the body of the device. 3D printing has been critical to prototyping a redesign because it has enabled the engineers to print overnight and iterate new designs in hours, a process that used to take weeks to accomplish on a shop floor.
This newly configured OCT design is almost ready for clinical application. Lumedica Vision Inc.’s OQ EyeScope
1.0 /X, a retinal spectral domain (SD)-OCT imaging system that features the compact and lightweight design, is in+ clinical-stage development, and FDA approval is pending. Excluding the chin rest, the system weighs just under 10 lbs. In the U.S., price is the most significant obstacle to using OCT in optometry, a field in which screening tools would have the most impact on eye disease diagnosis. Screening for glaucoma, age-related macular degeneration (AMD), and retinal disease in optometrists’ offices using a low-cost tool such as the OQ EyeScope could prevent millions of undiagnosed cases of these conditions each year.
A goal of product designers is to make OCT more accessible to health care systems in developing nations, where the $50,000 to $100,000 price tag for traditional OCT machines is often too steep. Blindness attributed to glaucoma occurs more frequently in Africa than in other parts of the world. And in sub-Saharan Africa, most of the population lives in rural areas, while glaucoma specialists and eye care practitioners often practice in faraway cities. A mobile eye clinic equipped with low-cost screening tools could meet an urgent need in this area of the world and others.
OCT devices in the home
Diseases such as glaucoma and AMD progress slowly, so clinicians predict that daily monitoring would improve patient outcome by guiding early intervention and therapy. Because most health care clinics cannot provide this level of care, there is a significant incentive to move OCT into the patient’s home for daily use. An at-home system presents challenges for OCT system designers: Since the device would be operated by the patient, both alignment and scanning would need to become automated tasks. And the system would need to be easy to use by people not familiar with operating medical devices. One 10-year study documenting the utilization of a similar home-monitoring device (though not OCT-based) showed promising results2.
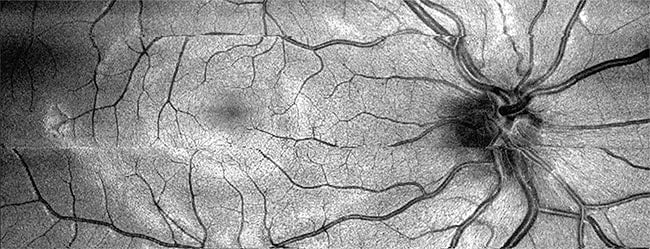
VIS-OCT has the capability to capture a full fundus image. Courtesy of Hao Zhang.
Daily at-home monitoring, however, would produce an abundance of patient image data that would need to be translated appropriately between the patient and doctor. Research shows that AI algorithms may be more efficient than trained physicians at managing large amounts of image data. Even highly qualified retinal specialists do not have the time to set aside to look for irregularities in the images in the database created for each patient. Notal Vision, a digital health company, has set out to marry self-monitoring OCT technology with the wealth of data collected from this approach. The company provides a monitoring center from which physicians can access relevant data, curated by AI-based algorithms, to plan personalized patient care.
OCT for primary care
Research into low-cost OCT has contributed to the creation of hand-held OCT designs, which are ideal for examining hard-to-reach areas such as the human ear. The OtoSight Middle Ear Scope, which was developed by PhotoniCare Inc. and approved by the FDA in 2020, helps physicians to diagnose middle-ear infections and in some cases eliminates the need for exploratory surgery.
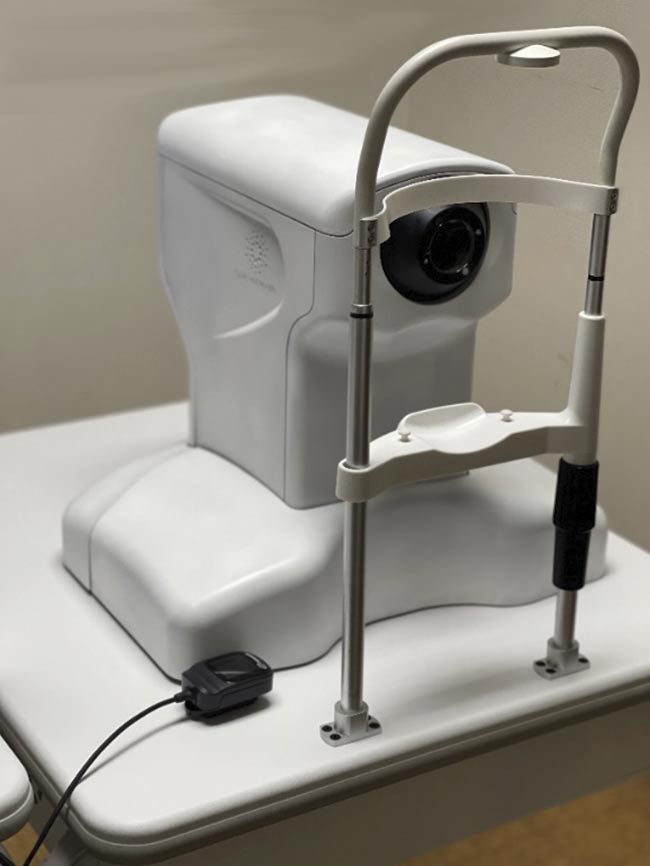
The Aurora X2 is a clinical research system used at universities. Courtesy of Hao Zhang.

The OQ EyeScope 1.0 /X, a tabletop clinical OCT system, is currently awaiting FDA approval for clinical use. Courtesy of Lumedica Vision Inc.
The current gold standard for diagnosing middle-ear infections, a pneumatic otoscopy exam, is correct only 50% of the time3. PhotoniCare advertises a 90.6% accuracy rate for detecting fluid buildup, the cause of middle-ear infections. When designers created the OtoSight, they determined that some capabilities were more important than others for its effective use. For example, to detect middle ear infection, primary care providers do not need to see the shape of the fluid buildup in the middle ear, but they do need to establish the existence of fluid and its turbidity. Therefore, instead of providing a complete B-scan, which is the depth profile of a sample over space, the OtoSight was designed to provide a rolling A-scan, or the depth profile over time, to supply the needed information. A simple point-and-shoot scanner enables the system to provide data on a single point as a series of images. This strategy reduces the size and cost of the design while making it easy for new users to interpret the system’s images when making diagnoses. Researchers predict that the next area of expansion for OCT in otology will be the creation of an endoscopic device for use in the ear4.
Even the use of near-infrared light, a fundamental element of traditional OCT, might be changed in future uses of the technology. This is because visible-light OCT (VIS-OCT) is showing promise as a retinal oximetry technique. The advantages of VIS-OCT include a higher axial resolution (<2 µm as compared to 6 to
7 µm in a typical OCT system) and higher image contrast. VIS-OCT systems are currently in early-phase clinical trials at leading ophthalmology clinics, including those affiliated with Hao F. Zhang at Northwestern University and others at New York University, Stanford University, the University of Virginia, and the University of Pennsylvania. Instead of the low-cost superluminescent diodes used in traditional OCT designs, however, most VIS-OCT designs depend on costly spatially coherent light sources, which is preventing the widespread adoption of VIS-OCT.
Open-source databases
Artificial intelligence is increasingly important in image analysis. Early data suggests computer vision will be able to identify retinal layer morphology and pathology. This work requires access to large databases of autonomous OCT retinal images. Several open-access OCT retinal image databases exist, including OCTID, published by Peyman Gholami and colleagues5, and an annotated image database complied by researchers from the University Hospital Center of Zagreb6. Studies of deep learning models indicate that the identification of systemic retinal biomarkers could provide early warning for diseases found outside the eye, such as cardiovascular, kidney, and neurodegenerative diseases7. The increased availability of low-cost and hand-held OCT will lead to the expansion of image databases such as these.
As with any new medical device that is trying to improve upon a previous model, innovators must demonstrate that their solution is more effective than that of the predicate device. In most cases, OCT provides improved resolution and therefore improved clarity for diagnosis, but implementing the technology in new fields may require providing continuing education to interpret the data provided in images. The glaucoma study conducted in sub-Saharan Africa did not inquire about the potential for OCT use. In the U.S., most optometrists are familiar with OCT images; however, continuing education may be necessary enable complete glaucoma management. Workflows within OCT software should be optimized for use in all settings, including continuing education, research studies, and busy clinics.
Next-generation system design and software development will go hand in hand to build the OCT system for the clinical environment in which it is used. The emergence of compact, user-friendly, lower-cost OCT devices will help to establish the technology as a standard method for point-of-care imaging in many settings, inside the clinic and at home.
Meet the author
McKenzie Peterson is sales and marketing associate at Lumedica Vision Inc. She is a writer by training, with a degree from the University of Georgia. She has a special interest in health care and topics concerning medical devices and their usability; email: [email protected].
References
1. G. Song et al. (2019). First clinical application of low-cost OCT. Trans Vis Sci Tech, Vol. 8, No. 3, p. 61, www.doi.org/10.1167/tvst.8.3.61.
2. M. Mathai et al. (2022). Analysis of the long-term visual outcomes of ForeseeHome remote telemonitoring: the ALOFT study. Ophthalmol Retina, www.doi.org/10.1016/j.oret.2022.04.016.
3. M. Pichichero and M. Poole (2001). Assessing diagnostic accuracy and tympanocentesis skills in the management of otitis media. Arch Pediatr Adolesc Med, Vol. 155, No. 10, pp. 1137-1142, www.doi.org/10.1001/archpedi.155.10.1137.
4. H.E.I. Tan et al. (2018). Optical coherence tomography of the tympanic membrane and middle ear: a review. Otolaryngol Head Neck Surg, Vol. 159, No. 3, pp. 424-438, www.doi.org/10.1177/0194599818775711.
5. P. Gholami et al. (2020). OCTID: Optical coherence tomography image database. Comp Electr Eng, Vol. 81, No. 106532, www.doi.org/10.1016/j.compeleceng.2019.106532.
6. M. Melinšcak et al. (September 2021). AROI: annotated retinal OCT images database. Proc. International Convention on Information, Communication and Electronic Technology (MIPRO), pp. 400-405.
7. T.M. Ramchod (2021). Systemic retinal biomarkers. Curr Opin Ophthalmol, Vol. 32, No. 5, pp. 439-444, www.doi.org/10.1097/icu.0000000000000784.