
Treating cancer lightly
Photodynamic therapy, which uses light-activated drugs to kill cells, is being investigated as a cancer treatment that is less damaging to the patient’s overall health than chemotherapy or radiation treatments. The drugs currently used in photodynamic therapy, called photosensitizers, produce singlet oxygen to kill the targeted cells. Unfortunately, the damage done by this gas can cause nearby cells to swell, leading to inflammation and pain at the site.
To reduce these side effects, researchers at the University of California have synthesized compounds that release nitric oxide (NO), rather than singlet oxygen, when they are stimulated by light. NO has been demonstrated to kill cancer cells effectively, but by means of a mechanism that does not cause swelling.
Inspired by their own work on an enzyme that is photoregulated by NO, the scientists determined that a metal-NO complex design that mimics the active enzyme site could be used to deliver the compound to cancer cells. The typical systemic NO donors, such as nitroglycerin, could not be used for this purpose, though. Once the donors are introduced into the body, they rapidly spread and begin to release the NO. To kill the cancer cells, massive doses of the compound would have to be administered and, because NO lowers blood pressure, the patient would be in danger long before a therapeutic amount could be introduced.
To render their concept feasible, the investigators had to develop a novel compound that would release the NO on command, in a limited area. They created dye-sensitized ruthenium nitrosyls (NO complexes of ruthenium) to deliver the treatment. These compounds are absorbed into cancer cells, limiting their interaction with healthy tissue, and respond to specific wavelengths of light by releasing their nitric oxide.
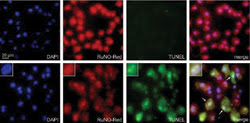
Fluorescence microscopy of breast cancer cells treated with 200 μm of a ruthenium nitrosyl compound shows the difference between cells kept in the dark (top row) and those exposed to 1 min of visible light (bottom row). DAPI, a stain used in multicolor fluorescence, shows the cell location in blue. The compound fluoresces red, while the green TUNEL staining highlights the damaged cells. The insets are a magnified view of a treated cell undergoing apoptosis. Image courtesy of Pradip Mascharak.
Before they are activated, the compounds are fluorescent, which enabled the investigators to track their uptake into breast cancer cells in a laboratory setting. After the NO is released, the fluorescence is quenched. The cells began to show signs of apoptosis within four to eight hours after exposure to light.
“We are planning to go all the way,” said Pradip Mascharak, the principal investigator of the study. The team intends to design patches containing the ruthenium nitrosyls that could be placed on skin malignancies or near the site of breast and prostate cancers. The patches would then be activated by specific wavelengths of light, and high doses of NO would be delivered to the tumor site.
Published: September 2009