The new generation of devices can heighten resolution, integrate patient data with intraoperative images and allow for more exact localization of surgical targets.
By integrating intelligence, video, intraoperative-imaging and navigation technologies, today’s surgical microscopes provide surgeons with insights to improve their decision-making at the point of care and provide patients with the best possible outcomes.
Surgical microscopes enable physicians to perform delicate surgery through tiny incisions. With a microscope, a surgeon can visualize anatomy within small cavities not perceptible by the human eye alone. They have long been used for ophthalmology.
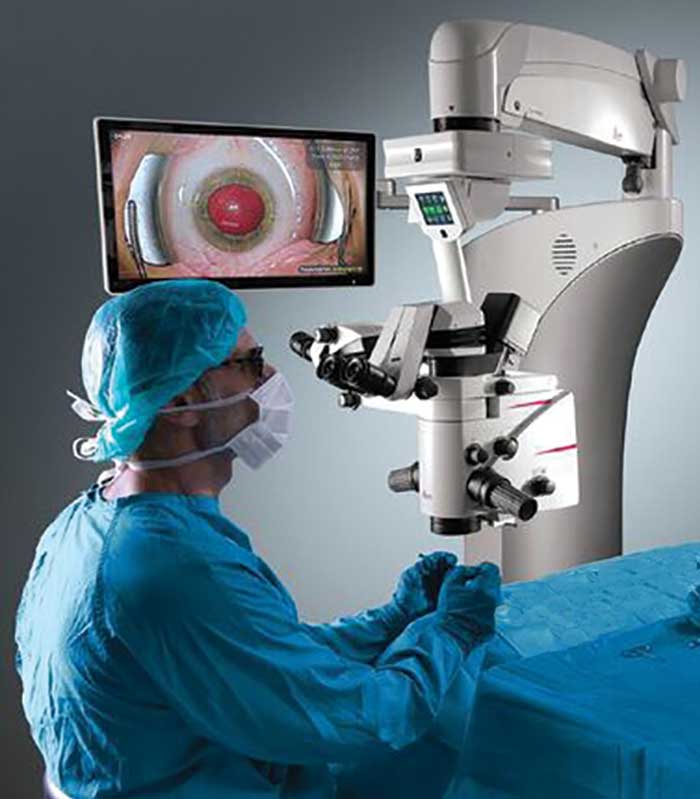
This ophthalmic cataract surgery makes use of the Prove 8 ophthalmic microscope and IOL guidance software from Leica. Courtesy of Leica Microsystems.
“Currently, cataract surgery is performed through the smallest incision
of any surgery on a major organ system in the human body,” said Jim
Mazzo, global president of ophthalmology at Carl Zeiss Meditec in
Dublin, Calif. “By making smaller incisions of up to1.8 mm,
ophthalmologists can improve the visual outcomes of patients and promote
faster visual recovery.”
Such microsurgery demands an operating microscope that is designed to support small-incision procedures. But many structures and transparent objects, such as fragments of the eye’s natural lens or the eye’s capsular bag, are not visible under normal light. Stereo coaxial illumination (SCI) is changing that.
“The stereo coaxial illumination allows surgeons to visualize transparent structures in a highly contrasted way,” said Mazzo. “Apochromatic correction of all major optical components results in improved resolution and a high level of contrast.”
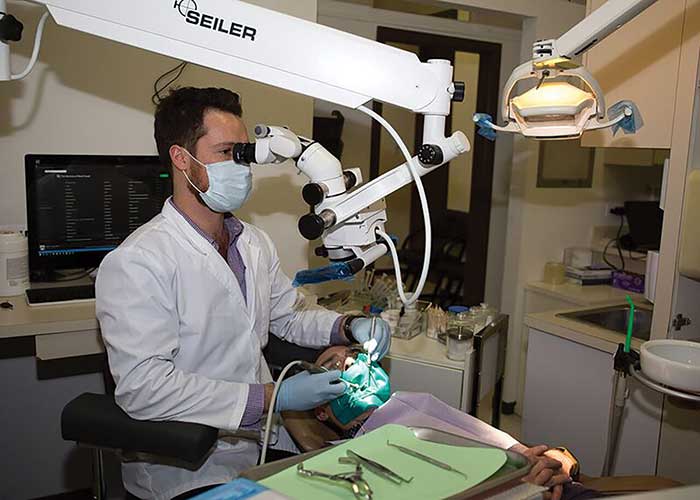
Operating microscopes have evolved over the last few decades into highly sophisticated devices, providing a range of useful digital technology add-ons. Courtesy of Alen Jakob, D.M.D., Midtown Root Canal Specialist, New York.
In addition, coaxial illumination provides a shadow-free view of the
area of interest and a variety of magnification settings that allow a
surgeon to adjust magnification and field of view throughout a
procedure.
“The illumination system is housed in the floor stand to keep the bulb heat away from the operating field,” he added. “The light is transmitted to the operating field by a fiber optic cable.”
Combining technologies in real time
From the beginning, high-end surgical microscopes have been packed full of high-tech innovations. These offered features such as enhanced illumination, intraoperative fluorescence and optical coherence tomography (OCT), computer-assisted guidance, high-definition video recording and touchscreen control.
Now, manufacturers are taking that one step further, said Kevin Cooley, director of new product sales and development at Prescott’s Inc. “The most recent advances come from combining technology that was otherwise separate and not in real time.”
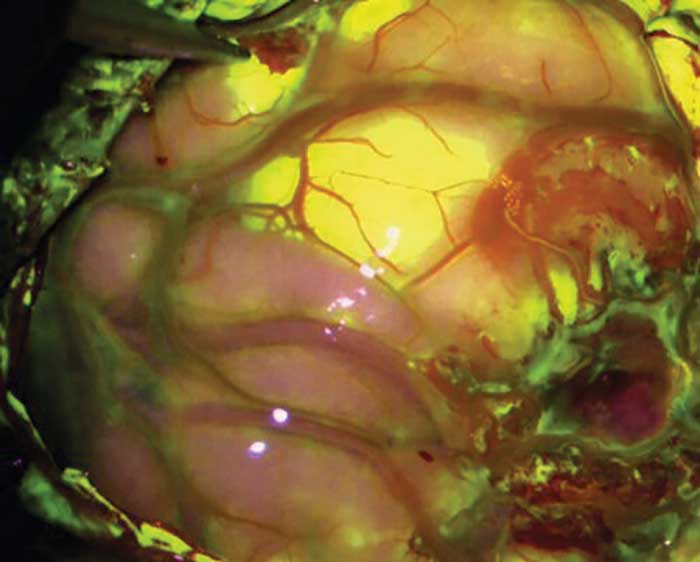
YELLOW 560, another Zeiss product that is approved for research use in the U.S., is the first fluorescence module highlighting the fluorescence-stained structures while viewing nonstained tissue in its natural color. Courtesy of Dr. Aaron A. Cohen-Gadol, Indiana
University, Department of Neurosurgery, Indianapolis, and Carl Zeiss Meditec.
Prescott’s, a surgical microscope specialist in Monument, Colo., has developed the OmniPlus/OSM200, which has an integrated 4K streaming video camera, still-image-capturing capability and 64 G memory. The integrated camera can be paired with a smartphone, tablet or remote-control-designated HDMI cable for monitor display.
Manufacturers also are integrating OCT into surgical microscopes to further support visualization during ophthalmic surgery, particularly for retinal and corneal procedures. Zeiss was the first to integrate real-time high-definition OCT in 2014 into the eyepiece of the OPMI LUMERA 700 microscope, which provided surgeons with unprecedented views right down to the transparent structures in the anterior and posterior segments of the eye. Leica, too, is getting into the market.
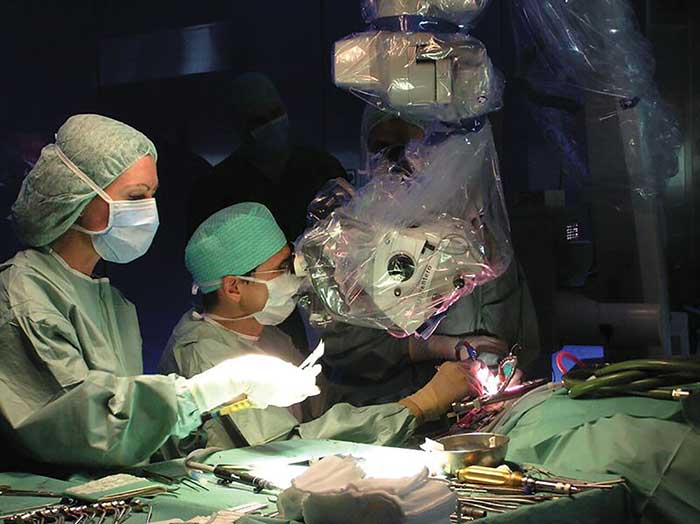
Zeiss OPMI Pentero in action in a real-time surgical scenario. The Pentero is part of the company’s suite of advanced surgical microscopes. Courtesy of Carl Zeiss Meditec.
“In ophthalmic surgery, while diagnostic OCT has been in place for many years, it is only recently that intrasurgical OCT has been seen as a valuable tool in the surgical suite,” said Patrick Wolf, senior product manager, Ophthalmology, Medical Division at Leica Microsystems, Heerbrugg, Switzerland.
“Several studies have been conducted to evaluate the intrasurgical benefits of OCT and have demonstrated a positive impact on surgical process and outcomes,” said Wolf. “The PIONEER study1, for example, showed that intrasurgical OCT altered surgical understanding of underlying tissue and affected decision-making in 48 percent of lamellar keratoplasty cases and 43 percent of membrane peeling procedures.”
Innovations in surgical microscopes are also providing eye surgeons with more flexibility to treat eye conditions such as macular degeneration, cataracts and glaucoma. If the patient’s cornea no longer lets light enter the eye properly because of scarring or disease, a transplant may be the only solution. But operating on opaque corneas can be difficult.
Surgical techniques for transplants have evolved dramatically over the past several years. For example, Descemet’s membrane endothelial keratoplasty (DMEK) has emerged as a promising, but more challenging, alternative to older techniques such as penetrating keratoplasty (PK).
During a PK, a perfectly round circle of cornea is removed and replaced with donor tissue. Unlike PK, DMEK allows for a pure anatomical replacement of scarred and damaged tissue and the possibility of even better vision with quicker recovery.
“However, surgeons using this technique often experience obstacles such as opaque corneas. Even with our high-end microscopes, surgeons would not be able to see through the cornea and perform surgery accordingly,” said Zeiss’ Mazzo. “Using intraoperative OCT with our Zeiss OPMI LUMERA 700 and RESCAN 700, surgeons are able to visualize structures of the eye’s anterior chamber — even if the view is blocked.”
Integrated images
In the meantime, displays are creating a high-resolution augmented reality for surgeons to work from.
“Technologies such as image injection, 4K video, robotics and advanced fluorescence-based digital processing have transformed the classical optical surgical microscope into a cutting-edge tool that not only shows the clinical team a great image but by providing additional information can help the surgeon make decisions,” said Dirk Brunner, global head of the Microsurgery Division at Carl Zeiss Meditec.
In ophthalmology, microscope-integrated image injection, such as with the Zeiss Cataract Suite markerless, allows for patient data transfer between examination equipment and intraoperative instruments. Overlays are projected right into the eyepiece of the microscope, providing surgeons with computer-assisted surgical guidance.
Similarly, Leica offers a markerless cataract guidance system, IOLcompass Pro, which injects guidance templates into the eyepieces of its ophthalmic microscopes.
In the field of neurosurgery, Leica’s new CaptiView image injection system overlays images in full high definition from image-guided surgery (IGS), otherwise known as neuronavigation software, into the microscope eyepieces.
“Surgeons can fully concentrate on their patient, have all the data in front of their eyes and do not need to look away from the surgical field during the procedure,” said Ohm Savanayana, director of imaging, medical division at Leica Microsystems.
In recent years, breakthroughs in LED technology have led to safer and more efficient lighting for surgical microscopes and to the integration of LED in the microscope.
“Light sources continue to become brighter and more powerful, approximating daylight, at an affordable price — such as LED cold light,” said Prescott’s Cooley. But, he added, the advance brings its own drawbacks. “Light toxicity remains an issue in certain procedures and illumination of the surgical field is very important to the surgeon.”
Light toxicity has always been a particular challenge in ophthalmology because damage to the retina could take place during lengthy procedures as light enters the eye through a dilated pupil. Overheating of tissue became an issue in other specialties such as neurosurgery, as Xenon light became brighter and more powerful.
Filters can enable delicate procedures to be carried out, and so can technology that limits the brightness depending on the working distance. This helps to control the exposure of heat to tissue as well as to metallic objects such as instrumentation.
Although perhaps not as bright, LEDs are cheaper, longer lasting, can approximate Xenon in color and can be used for all surgery.
Another advance that has proved popular in recent years is an objective lens with a variable focus range. Previous objective lenses were infinity corrected with a fixed-front focal length and a limited fine focus adjustment of less than 25 mm. Variable focus objective lenses offer a variable front focal length with a range as much as 150 mm. One such lens is available from Seiler Instrument & Mfg Co. Inc. in St. Louis.
“The VarioFocus objective lens has a range from 200 to 350 mm,” said Bryan Signaigo, a design engineer at Seiler. “This improved focus range makes it easier for users to focus the system and reduces the need to reposition the microscope.”
Expanding uses
General dentistry is still an emerging application for surgical microscopes, with the vast majority of general dentists not yet incorporating a surgical microscope into their practice2.
Signaigo said, “Whereas 90 percent of endodontists use the microscope in their practice, in dentistry, the microscope can be used for much more than just endodontic procedures, including oral examinations, crown and veneer preparations, tooth extraction and dental implants.”
Another lesser known use of surgical microscopes makes use of fluorescence for vascular procedures and neurosurgery. Fluorescence-guided surgery (FGS), which has been possible for many years, combines the use of an injected or ingested fluorescing agent with a light filter from the microscope. It helps surgeons visualize diseased tissue and blood vessels.
Zeiss partnered with Prof. Dr. Andreas Raabe to develop fluorescence-based angiography technology with its INFRARED 800, which was introduced in 2006 for intraoperative visual assessment of blood flow and vessel patency. Devices such as this one and Leica’s FL800 enable visualization of blood flow dynamics during aneurysm surgery.
In-depth analysis and interpretation is further facilitated by FLOW 800 from Zeiss, which compiles fluorescence video sequences from INFRARED 800 into visual maps, diagrams and side-by-side comparisons.
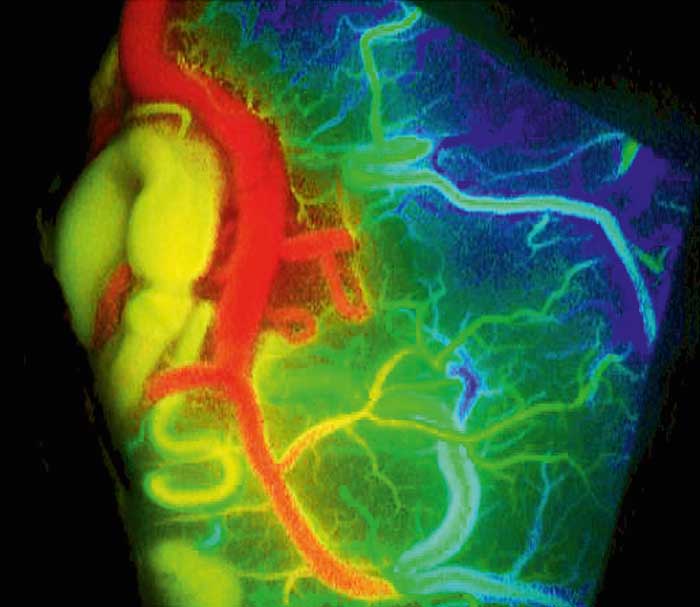
FLOW 800 from Zeiss generates overview maps and diagrams and permits an interpretation of the fluorescence videos and an analysis of the blood flow dynamics through comparative views. The image shows a color map visualization of vascular blood flow to identifying drainers and feeders in a vascular condition. Courtesy of Yasushi Takegi M.D., Ph.D., Department of Neurosurgery, Kyoto University, Kyoto, Japan, and Carl Zeiss Meditec.
Among the most advanced microscopes are those that use intraoperative fluorescence technologies for neurosurgery, where exact localization of a tumor is critical. The challenge with cancerous brain cells in particular is that they are exceptionally difficult to discern from normal brain cells. Even under a powerful surgical microscope, tumor perimeters are hard to differentiate from healthy tissue.
Zeiss was the first to develop intraoperative fluorescence technologies in the field of neurosurgery. Together with Prof. Dr. Walter Stummer, the company introduced fluorescence-based tumor resection with its OPMI Neuro FL in 1998 for differentiation between diseased and healthy tissue. In 2005, the company introduced the Blue 400, which is approved for research use in the U.S.
Zeiss BLUE 400, which is in research use in the U.S., distinguishes between diseased and healthy tissue during surgery on a brain tumor, for example. The malignant tissue glows red. Courtesy of Prof. Dr. Walter Stummer, University Clinic Münster, Germany, and Carl Zeiss Meditec.
Leica also is coming into this market with the FL400, which has not yet been approved in the U.S, and the FL560, which is for research purposes. As with the Zeiss technologies, the devices combine a surgical microscope with fluorescing agents to help a surgeon visualize malignant tissue during complete tumor resection.
“In the future, fluorescence-guided surgery and other navigation-enhancing technologies will continue to provide more data to the surgeon in the operating room,” said Leica’s Savanayana. “The more data surgeons have, the more precisely they can implement surgical procedures to support optimal patient outcomes.”
References
1. J.P. Ehlers et al. 2014. The Prospective Intraoperative and Perioperative Ophthalmic Imaging with Optical Coherence Tomography (PIONEER) Study: 2-Year Results. Am J Ophthalmol, Vol. 158, Issue 5, pp. 999–1007. http://dx.doi.org/10.1016/j.ajo.2014.07.034.
2. D. D. Kersten et al. 2008. Use of the microscope in endodontics: results of a questionnaire. J Endod, Volume 34, Issue 7,
pp. 804-807.
Surgical Microscopes: Then and Now
The first commercial surgical microscope was developed by Zeiss in the 1950s under the guidance of physicist Hans Littmann. Leading ENT surgeon Prof. Dr. Horst Wullstein provided ideas to enhance the device, and in 1953, Zeiss introduced the OPMI 1 at the ENT World Congress in Amsterdam. Within five years, the surgical microscope was being used for nasal surgery, and by the 1960s, its use extended to ophthalmic surgery and many other disciplines such as neurosurgery.
Another major advance came in 1994, when Zeiss introduced a fighter-jet-like head-up display into its first computerized surgical microscope, the OPMI ES. This allowed surgeons to inject critical patient data such as neurosurgical navigation. Since then, the displays have become high-resolution, high-contrast color systems that allow the surgeon to work in an augmented reality world superimposed on top of the classical microscope image.
And just three years ago, Zeiss’s OPMI LUMERA 700 broke new ground by integrating real-time high-definition OCT into its eyepiece.
A Wide Range of Applications
Surgical microscopes were originally used for ear, nose and throat (ENT) surgery, and continue to be used in these fields. However, today’s surgical microscopes are improving patient outcomes in other areas of medicine as well:
• Precise ophthalmic surgeries — Innovation in eye care enables better decision-making during retina, cataract and corneal surgeries.
• Demanding neurosurgical applications — During brain surgery, surgeons often have to make decisions that can have far-reaching consequences for patients. Surgical microscopes help them make such decisions, for example allowing surgeons to assess the degree of openness of a blood vessel to determine if a tumor can be completely removed.
• Simplifying ENT surgery — Efficiency is critical for surgeons who often face back-to-back ENT surgeries. By simplifying the procedure, more surgeries can be performed.
• Spinal surgery — Seeing more through small incisions is vital where minimally invasive surgery is employed for better patient care, reducing trauma and increasing recovery.
• Plastic and reconstructive surgery — Microsurgery minimizes the trauma experienced by the patient and improves patient results.
• Effective diagnostics and dental treatments — Surgical microscopes for dentistry visualize details and fine structures that are otherwise difficult to see. Ergonomically designed dental microscopes help prevent back and neck pain.
• Gynecology — Colposcopes can be used for early detection and correct diagnosis of pre-invasive and invasive epithelial anomalies of the genital tract that assist in curing cervical cancer.