
Treating battlefield injuries with light
Closing wounds with
stitches and staples could one day be a thing of the past, thanks to work being
done on treating airmen’s battlefield injuries with a light-activated technology.
The technique results from research managed by the US Air Force Office of Scientific
Research and supported by funds from the Office of the Secretary of Defense.
The new treatment includes photochemical tissue bonding, a process
that could replace conventional sutures, staples and glues in repairing skin wounds
and reconnecting severed peripheral nerves, blood vessels, tendons and incisions
in the cornea.
Harvard Medical School professor and Massachusetts General Hospital
Wellman Center researcher Dr. Irene Kochevar and her colleague at Wellman, associate
professor Robert Redmond, are pleased with the initial lab bench experiments that
led to a pilot clinical study.
They have demonstrated that this technology is very helpful in
medicine for the Air Force because it produces better healing and functional outcomes
than those for the same wounds that were treated with conventional materials, Kochevar
said.
The process of creating the bonding or nanosutures is accomplished
by applying Rose Bengal dye to the wound or damaged tissue and then exposing it
briefly to green light from a 532-nm KTP laser. The researchers also have used LED
arrays. The dye absorbs most strongly between 510 and 570 nm, helping it to molecularly
bond proteins on the tissue surface.
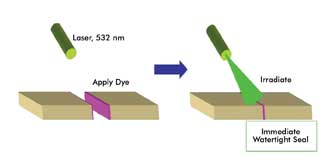
Healing with light is a two-stage process.
“No glues, proteins or other materials are used that might
stimulate an inflammatory response,” Kochevar said. “An immediate, watertight
seal is formed between the tissue surfaces, leading to reduced inflammation in the
near term and better scar formation in the long term.”
The researchers plan to continue to evaluate the effectiveness
of the new technology and the ways in which it can be even more effective in theater.
They are seeking a shorter treatment time that will yield an even stronger bond.
Currently, Kochevar said, “typical radiation times are 1.5 to 5 minutes. For
skin closures, the irradiation time is 200 s (100 J/cm2).”
Kochevar said that the researchers have published more than “a
dozen studies, mostly in animal models of different types of surgery (reattachment
of peripheral nerves, blood vessels), sealing of corneal wounds and transplants,
sealing skin incisions and excisions.
She noted that the two basic types of applications involve bonding
tissue surfaces together. “One is rejoining tissue – for example, surgical
incisions in tissues such as cornea – the other is patching over a tissue
site. For rejoining tissue surfaces, an aqueous solution of the dye is applied to
the surfaces, which are then brought into contact and the area irradiated.
“For ‘patching,’ a membrane (amniotic is our
favorite) is stained with the dye and then placed over the tissue site. For example,
to rejoin a severed peripheral nerve, the two ends are held together with one or
two stay sutures, and then the joint is wrapped with dye-stained amnion and irradiated
to seal the amnion to the epi-neurium. We follow the animals for up to four months
and assess the appropriate end points (histology, electrophysiologic measurements,
scar formation, et cetera.”
For now, the work has been confined to animals. However, Kochevar
said, they have begun to work with humans in a pilot clinical study for sealing
skin surgical wounds.
“We are approaching this challenge by identifying the basic
molecular mechanisms responsible for light-activated cross linking. We believe that
this information will show us how to improve the efficiency and effectiveness of
the nanosuturing technology on the battlefield,” Kochevar said.
Published: September 2010