James Hermanowski, Nathaniel Group, Inc.
Xenon light sources represent the benchmark for medical illumination, but they cannot couple light through the small channels used for microendoscopes.
Significant research has been undertaken to improve imaging sensors for endoscopy, but little work has been done to maximize the performance of the light sources and the light delivery system required to support them. Xenon light systems suffer from weak light delivery through small fibers in spite of continuous sensitivity improvements to image sensors. A new endoscopic illumination system can significantly reduce the size of traditional video endoscopes.
Physical space constraints continue to affect advanced procedures such as single-incision laparoscopic surgery, robot-assisted surgery and other minimally invasive surgical procedures. More functionality and instruments are desired and are being squeezed through the smallest possible incisions. Space continues to tighten with the migration of larger-diameter 3-D, high-definition endoscopic imaging systems into minimally invasive procedures. Fortunately, a significant portion of the endoscope, the light delivery channel, can be reduced in size to allow the space to be used for other purposes or to allow the shrinking of the endoscope itself.1
For many years, illumination systems have teamed with endoscopic imaging systems for medical applications to help image inside body cavities (colon, abdomen, heart, throat, nose, ear, eye); to assist in the placement of internal medical devices such as gastric bands; and even to perform work such as ablation of unwanted or diseased tissue as in laser eye surgery or laser atrial fibrillation treatment. The use of in vivo illumination sources for medical applications has expanded recently to even more revolutionary technologies, including spectrophotometry, fluorescence analysis,2 near-infrared lipid core plaque detection and optical coherence tomography.
Functions of light
Viewing tissues using white light alone is effective in detecting many lesions and in determining the general health of the tissue. In contrast, some bacterial infections, lipid plaque, and precancerous and subtle inflammatory conditions are difficult to visualize under white light. Furthermore, it can be challenging to position an illumination and imaging system in the vicinity of the organ to be viewed. Once there, it is desirable and advantageous to use light to do more than illuminate the object: Radiation in the form of visible light, infrared or ultraviolet wavelengths can be used to do work.3 The delivered radiation can be used to assist in the diagnosis of disease using fluorescence or spectroscopy, to cut diseased4 tissue for removal, to ablate stones, to initiate a reaction between a therapeutic molecule and its target reaction site, or to provide physically based phototherapy.
Fluorescence imaging techniques use a generally nondestructive property exhibited by some materials. Fluorescence occurs when a material absorbs radiation of one wavelength, converts some portion of that radiation to a slightly different and usually longer wavelength, and then re-emits it. For example, when normal oral cavity tissues are illuminated with violet light (405 nm), they have a fluorescence emission that appears light blue. The effect is small but can be noticeable and help discriminate between healthy tissue and tissue with underlying problems.5 Fluorescence can be the result of tissue labeling using fluorophores or the result of autofluorescence, where the specimen naturally exhibits the property.
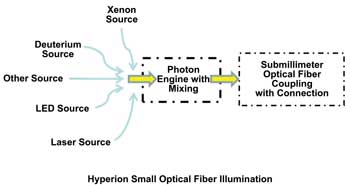
Figure 1. The new Hyperion 300 submillimeter optical fiber illumination system enables smaller instruments for endoscopy, microsurgery and other applications. Images courtesy of Nathaniel Group Inc.
For endoscopic diagnostic tests, narrowband illumination can provide a sharper image or better contrast. Hemoglobin has peak absorption at specific wavelengths in the blue and green bands, so illumination using these wavelengths improves visibility and identification of blood vessels and capillaries. Additionally, the different light absorption of hemoglobin bound with oxygen versus hemoglobin without oxygen can be used to calculate oxygen saturation when absorption is measured at two different wavelengths. Narrowband illumination has also been helpful in identifying Barrett's esophagus6,7 and a typical dysplastic colon cells, and in differentiating between malignant and benign cells of the urinary bladder.
Photochemotherapy or photodynamic therapy involves the administration of a sensitizing agent followed by the action of light on tissues where the photosensitizer is localized.8 The need for ample illumination through small optical fibers is one limiting factor of this promising technique.
Physical phototherapy normally involves using infrared radiation to penetrate deep within tissue to deliver heat and stimulate blood vessel expansion. Often infrared radiation is used because it can penetrate through tissues easily. Infrared lasers are a preferred embodiment, allowing large doses to be delivered in short times under controlled positioning of the therapy.
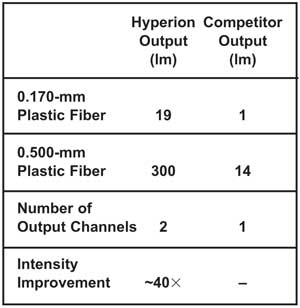
Table 1. Measured optical output from Hyperion 300 small optical fiber illuminator (output from each of two channels) compared with standard fiber illumination source.
Optical fibers and imaging systems
A new approach couples radiation from a variety of sources into individual submillimeter optical fibers or fiber bundles for medical and industrial applications. The Hyperion 300's patent-pending technology from Nathaniel Group Inc. allows integration and mixing of multiple sources into an optical fiber, including infrared, white-light, ultraviolet and solid-state sources. The flexibility of the system allows the optimum source or sources to be selected for each application. For example, a xenon source for general illumination can be combined with the stable UV output from a deuterium lamp for semiquantitative spectroscopy; or solid-state LED sources can be combined for general illumination and fluorescence imaging with an infrared laser source for ablation, allowing the visualization,9 analysis and removal of diseased tissues.
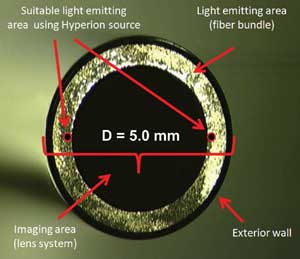
Figure 2. A traditional endoscope tip showing the imaging area, light-emitting area and protective exterior wall. Significant space is consumed by the lighting function.
A primary use for the new device is reducing the size of the light channel in endoscopic imaging systems for both traditional endoscopes and the latest generation of millimeter-dimensioned medical camera systems such as the Awaiba sensor.
Table 1 compares the measured radiometric output of a Hyperion 300 small optical fiber illumination system to other fiber illumination sources on the market. The data was measured for white light in lumens at the distal end of a 1-m fiber connected to the source. The new device was in a configuration with two output channels optimized for coupling radiation into optical fibers ≤0.5 mm. The data demonstrates exceptional performance for fiber diameters down to 170 µm.
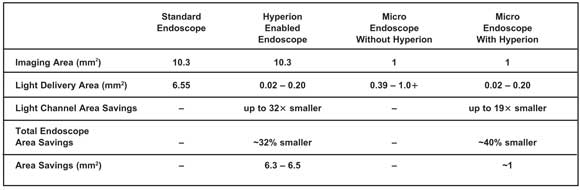
Table 2. Comparison of endoscope sizes using Hyperion as light source; here, a microendoscope uses an Awaiba NanEye 2B video camera. The Hyperion reduces the standard endoscope size by up to 6.5 mm2, enough to make space for another instrument.
Figure 2 is a photograph of a traditional endoscope tip showing the imaging area, light-emitting area and protective exterior wall. Significant space is consumed by the lighting function. The figure shows at scale the amount of space required for the new device to deliver suitable illumination. The light source consumes only 0.43 to 3 percent of the endoscope area, depending upon implementation (see Table 2). Switching to the new source reduces the standard endoscope size by up to 6.5 mm2, enough to make space for an instrument.
Figure 3 shows a side-by-side color rendering comparison of an endoscope setup using the new source and a standard xenon source, considered to be the benchmark for medical illumination. The image clearly demonstrates that both sources provide comparable color matching, while the Hyperion source shows improved color saturation.

Figure 3. A comparison of Hyperion 300 endoscopic light source (left) to a commercial xenon source shows good color matching and improved color saturation. Color comparison was carried out using an X-Rite color card, a Weck endoscope and a Richard Wolf HD three-chip camera system.
There is a continuous drive to reduce the size of imaging systems for medical applications. Smaller imaging systems allow exploration of ever-smaller cavities and reduce the impact on living organisms. A new small fiber illumination light source was studied to determine its capabilities as a light source enabling microendoscopic imaging systems.
Radiometric measurements of the new light source showed performance up to 40 times better than that of other systems.
The light source was coupled with two imaging systems. The first imager was a NanEye ultrasmall 1 x 1-mm, 250 x 250-pixel sensor from Awaiba. The second camera consisted of a three-sensor high-definition camera illuminated through a 500-µm fiber. In both cases, the new light source allowed for a significant reduction in endoscope size without deteriorating function.
Meet the author
James Hermanowski is vice president of business development at Nathaniel Group Inc. in Vergennes, Vt.; email: [email protected]. The author thanks Jeff Cogger at Nathaniel Group Inc. for mechanical designs and data collection, and the staff of Awaiba GmbH for support relating to its imaging system.
References
1. J. Hermanowski (August 2011). High Intensity Illumination from Small Fibers for In-Vivo Medical Lighting, www.nathaniel.com.
2. R. Schwarz et al (April 2009). Noninvasive evaluation of oral lesions using depth-sensitive optical spectroscopy. Cancer, Vol. 115, pp. 1669-1679.
3. A. Mendez (Jan. 1, 2011). Medical applications of fiber optics: Optical fiber sees growth as medical sensors, OptoIQ.
4. D. Roblyer and R. Richards-Kortum (January 2010). Optical diagnosis for early detection of oral cancer, American Dental Hygienists' Association Access, pp. 22-25.
5. Q. Nguyen (October 2011). Color-Coded Surgery, TEDMED Conference.
6. R. Singh et al (Oct. 14, 2011). Advanced endoscopic imaging in Barrett's oesophagus: A review on current practice. World Journal of Gastroenterology, pp. 4271-4276.
7. S. Tanaka and Y. Sano (May 23, 2011). Aim to unify the narrow band imaging (NBI) magnifying classification for colorectal tumors: Current status in Japan from a summary of the Consensus Symposium in the 79th Annual Meeting of the Japan Gastroenterological Endoscopy Society. Digestive Endoscopy, pp. 131-139.
8. A. Dietze (November 2004). Preclinical evaluation of photochemical treatment on rheumatoid arthritis and soft tissue sarcomas, Institute for Cancer Research at the Norwegian Radium Hospital.
9. S. Park et al (January/February 2008). Automated image analysis of digital colposcopy for the detection of cervical neoplasia. Journal of Biomedical Optics, Vol. 13, 014029.