
Laser-Based Tool Tells Normal Tissue From Tumors
ANN ARBOR, Mich., & CAMBRIDGE, Mass., Sept. 5, 2013 — A new laser tool can microscopically distinguish between normal and cancerous brain tissue in real time. Since it doesn't miss cells that could trigger new tumor growth, the method could make brain cancer surgery much more effective.
 The approach, called SRS (stimulated Raman scattering) microscopy, was developed by the University of Michigan Medical School and Harvard University and funded by the National Institutes of Health. The work is featured this week on the cover of Science Translational Medicine.
The approach, called SRS (stimulated Raman scattering) microscopy, was developed by the University of Michigan Medical School and Harvard University and funded by the National Institutes of Health. The work is featured this week on the cover of Science Translational Medicine.
A multidisciplinary team of chemists, neurosurgeons, pathologists and
others worked to develop and test the tool, which marks the first time
SRS microscopy has been used in a living organism to see tumor margins —
the boundary area where tumor cells infiltrate among normal ones.
That's the hardest area in which a surgeon operates, especially when a
tumor has invaded a region with an important neurological function.
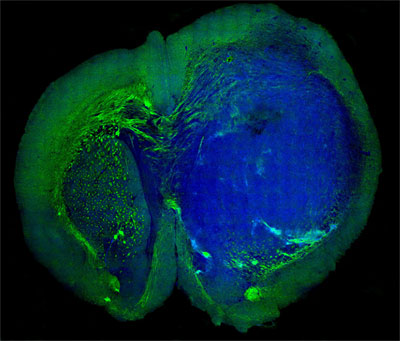
This image of a human glioblastoma brain tumor in the brain of a mouse was made with stimulated Raman scattering, or SRS, microscopy. The technique allows the tumor (blue) to be easily distinguished from normal tissue (green) based on faint signals emitted by tissue with different cellular structures. Courtesy of Xie lab, Harvard University.
The team used the tool to "see" the tiniest areas of a human glioblastoma brain tumor in a live mouse's brain tissue. They were also successful in imaging tissue removed from a patient with glioblastoma multiforme, one of the most deadly brain tumors. On average, patients with this type of tumor live only 18 months after diagnosis. Surgery is one of the most effective treatments, but less than one-fourth of operations achieve the best possible results, according to a study published last fall in the Journal of Neurosurgery.
“Though brain tumor surgery has advanced in many ways, survival for many patients is still poor, in part because surgeons can’t be sure that they’ve removed all tumor tissue before the operation is over,” said co-lead author Daniel Orringer, M.D., a lecturer in the U-M department of neurosurgery.
“Biopsy has been the gold standard for detecting and removing these types of tumors,” Harvard's Sunney Xie, Ph.D., the co-lead author of the paper, told the Harvard Gazette. “But this technique, we believe, is better because it’s live. Surgeons can now skip all the steps of taking a biopsy, freezing, and staining the tissue. This technique allows them to do it all in vivo.”
With the SRS technique, they can detect a weak light signal that comes out of a material after it's hit with light from a noninvasive laser. By carefully analyzing the spectrum of colors in the light signal, the researchers can tell a lot about the chemical makeup of the sample.
Over the past 15 years, Xie has advanced the technique for high-speed chemical imaging. By amplifying the weak Raman signal by more than 10,000 times, it is now possible to make multicolor SRS images of living tissue or other materials. The team can even make 30 new images every second — the rate needed to create videos of the tissue in real time.
The authors suggest that SRS microscopy may be as accurate for detecting tumor as the approach currently used in brain tumor diagnosis, called H&E staining. Comparing the two approaches, three surgical pathologists had nearly the same level of accuracy, no matter which images they studied. But unlike H&E staining, SRS microscopy can be done in real time, and without dyeing, removing or processing the tissue.
Currently, the SRS microscopy system is not small or stable enough to be used in an operating room. The team is collaborating with a startup company formed by members of Xie’s group, called Invenio Imaging Inc., which is developing a laser to perform SRS through inexpensive fiber optic components. The team is also working with AdvancedMEMS Inc. to reduce the size of the probe that makes the images possible.
A validation study, to examine tissue removed from consenting U-M brain tumor patients, may begin as soon as next year.
For more information, visit: www.umich.edu or http://chemistry.harvard.edu/
Published: September 2013