Compiled by BioPhotonics staff
Coronary atherosclerosis could someday
be more easily diagnosed and treated, thanks to a new version of the intravascular
imaging technology optical coherence tomography that provides a resolution 10 times
greater than that of standard OCT.
The new version, developed at the Wellman Center for Photomedicine
at Massachusetts General Hospital, is called microOCT, and it provides the contrast
and resolution required to show individual arterial and inflammatory cells within
coronary artery samples, including subcellular features that may identify vulnerable
plaques.
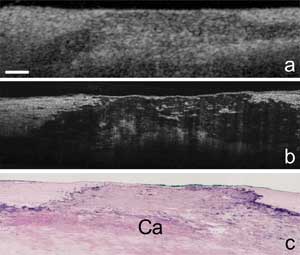
These are images of a coronary artery plaque (Ca in image c) produced by (a) standard OCT, (b) microOCT and (c) tissue histology. Courtesy of Nature Medicine and the Wellman Center
for Photomedicine at Massachusetts General Hospital.
OCT, a catheter-based technology, uses reflected near-infrared
light to create detailed images of a blood vessel’s internal surfaces. Standard
OCT is used to identify arterial plaques that are likely to rupture, but it can
only clearly image structures larger than 10 μm. Now, using new types of lenses
and advanced imaging components, microOCT can image structures as small as 1 μm.
The technique reveals an intact tissue’s detailed information in three dimensions
– and does so much more quickly than with the prepared tissue slides of traditional
pathology.
Using microOCT, researchers were able to image human and animal
coronary artery tissue, revealing inflammatory cells that contribute to the formation
of coronary plaques, endothelial cells that line coronary arteries, smooth muscle
cells that produce collagen in response to inflammation, and fibrin proteins and
platelets that are involved in the formation of blood clots.
The technology also can distinguish between bare-metal stents
and drug-eluting stents placed in coronary arteries. During the study, defects in
the drug-eluting coating were identifiable using the technology.
The researchers anticipate that observation of cells with microOCT
could be performed in humans in roughly three to five years. They are hopeful that,
with the ability to follow and track cells in 3-D, they can prove or disprove many
theories of coronary artery disease, as well as better understand how clots form
on a microscopic level.
In addition, improved definitions of high-risk plaques could lead
to greater accuracy in identifying those that could rupture or block coronary arteries.
The researchers also said that being able to monitor the healing of implanted stents
could reduce the number of patients who must be on anticlotting medications, which
have major side effects and are very costly.
Findings were described in the July 10 online edition of Nature Medicine (doi: 10.1038/nm.2409).